A recent government report on the Pre-Existing Condition Insurance Plan (PCIP) found overall enrollment is lower than projected, and that total enrollment in the 24 federally administered programs is much lower than in the 27 programs administered by states. Some news coverage of the Government Accountability Office (GAO) report suggested the program, which has been operational for about a year, is not meeting expectations and that the federally administered programs are less effective than the state programs. But a closer look at the drivers of enrollment does not support this interpretation.
Under the PCIP—a temporary national high-risk pool established under the Affordable Care Act that makes insurance available to people with preexisting conditions who cannot access coverage in the individual market and who have been uninsured for at least six months—states had the option to run their own programs or take part in the federally administered program. PCIP coverage is intended to serve as a bridge until 2014 when the state health insurance exchanges become operational and the regulation ensuring people can no longer be denied coverage based on their health status is in place.
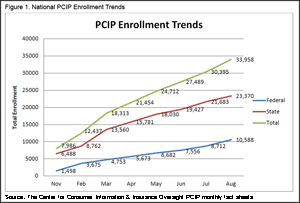 According to the GAO report, PCIP enrollment has grown steadily since implementation, and now stands at nearly 34,000 people nationally (see Table 1 and Figure 1). This number is low relative to the projected enrollment of 375,000 published by the actuary at the Centers for Medicare and Medicaid Services (CMS) in late 2009. However, the CMS projections may not have been realistic given the historically low enrollment in state-based high-risk pools and the six-month uninsurance requirement. This uninsurance requirement is likely limiting enrollment substantially because many individuals with chronic conditions would probably prefer to enroll in or stay with limited benefit plans than risk going uninsured for six months to qualify for the more comprehensive and potentially more affordable PCIP coverage. Because the uninsurance requirement is in the law, PCIP administrators do not have the ability to bypass or modify the provision.
According to the GAO report, PCIP enrollment has grown steadily since implementation, and now stands at nearly 34,000 people nationally (see Table 1 and Figure 1). This number is low relative to the projected enrollment of 375,000 published by the actuary at the Centers for Medicare and Medicaid Services (CMS) in late 2009. However, the CMS projections may not have been realistic given the historically low enrollment in state-based high-risk pools and the six-month uninsurance requirement. This uninsurance requirement is likely limiting enrollment substantially because many individuals with chronic conditions would probably prefer to enroll in or stay with limited benefit plans than risk going uninsured for six months to qualify for the more comprehensive and potentially more affordable PCIP coverage. Because the uninsurance requirement is in the law, PCIP administrators do not have the ability to bypass or modify the provision.
The GAO report also finds that 72 percent of PCIP enrollees are in programs administered by the states. Media reports have suggested that this disparity indicates the federal program has been less accessible and less effective at outreach. But to fully understand enrollment trends, one must consider the baseline insurance situation in each state. For example, two of the federally administered states, Massachusetts and Vermont, already had near-universal programs that did not deny coverage based on preexisting conditions when the PCIP was implemented, and therefore had few candidates for PCIP coverage. Similarly, two other federally administered states, Minnesota and Texas, had the two largest state high-risk pool programs in place when PCIP was implemented. Another factor favoring enrollment in the state programs is that state administrators more fully understand the local uninsured populations and related programs. The state-administered program in Pennsylvania, for example, targeted individuals on a waiting list for a state-financed safety-net insurance program.
A significant barrier to enrollment for all of the PCIP programs, both federal and state-administered, is the relatively high cost of the coverage. Even though PCIP regulations cap premiums at the local standard market rate, many of the uninsured with chronic conditions are individuals with incomes less than 400 percent of the federal poverty level, who may simply find those rates unaffordable. Unlike future enrollees in the exchanges, the Affordable Care Act does not subsidize premiums or out-of-pocket spending for PCIP enrollees. The federally administered plans, however, have aggressively pursued reducing premium costs within program guidelines to maximize affordability of coverage, which should attract more enrollees.
While the PCIP is not enrolling everyone potentially eligible, enrollment continues to grow and the program will continue to provide critically needed coverage to thousands of people until the exchanges become operational in 2014.



