More than 11 million people in the United States depend on long-term services and supports (LTSS) to assist them with everything from routine personal care and home modifications such as adding ramps to nursing home care. As the population ages and methods to manage chronic diseases improve, the demand for long-term services continues to grow. Yet given limited resources, it is increasingly important not only to improve these services but also to facilitate independence for patients who would rather stay in their own homes than live in nursing homes or other facilities.
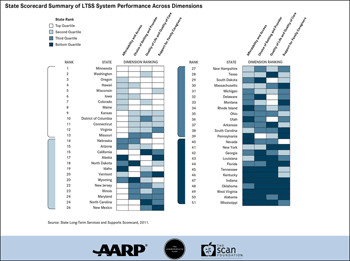
On October 3, the Alliance for Health Reform and The Commonwealth Fund held a briefing for 200 congressional staff and other stakeholders on the opportunities and challenges in the LTSS system. The event incorporated the findings of first-ever State Scorecard on Long-Term Services and Supports, which was published last month by The Commonwealth Fund in partnership with AARP’s Public Policy Institute and The SCAN Foundation. The Scorecard examined four key dimensions of state performance: affordability and access to services, patient choice of setting and provider, quality of life, and support for family and other informal caregivers.
 At the briefing, featured panelists included Bob Hornyak of the Administration on Aging, Cynthia Woodcock of the research firm IMPAQ International, and Carol Raphael of the Visiting Nurse Service of New York.
At the briefing, featured panelists included Bob Hornyak of the Administration on Aging, Cynthia Woodcock of the research firm IMPAQ International, and Carol Raphael of the Visiting Nurse Service of New York.
Mary Jane Koren, M.D., vice president of the Long-Term Care Quality Improvement program at The Commonwealth Fund and co-moderator for this event, opened the briefing by describing key findings from the Scorecard. She noted that the authors faced challenges in compiling the Scorecard due to differences in the ways that states collect and report data, as well as gaps in data. Dr. Koren encouraged federal officials to develop common definitions of services, create uniform measures for determining states' effectiveness in coordinating the delivery of primary, acute, and long-term services and supports, and strengthen data collection requirements to monitor quality and assess value received for public expenditures. Likewise, she noted that federal policies could provide states with incentives and financial assistance to improve their LTSS systems, such as shared savings programs.
The Administration on Aging's Bob Hornyak gave an overview of the wide range of agencies and people involved in delivering home- and community-based services. Through this network of 69,000 trained caregivers and 855,000 informal caregivers, over 11 million patients receive some level of assistance, including the delivery of more than 241 million meals. His department is working to bolster the LTSS system by supporting its many volunteers and offering a single point of entry to a network of patient-centered services. The Administration on Aging also hopes to serve more people by integrating its services with other agencies such as public health departments and improve services through evidence-based research.
Cynthia Woodcock discussed states' efforts to coordinate long-term services and manage spending by "rebalancing," a term used to describe the shift from full institutional care to supports in home- and community-based settings. Currently, most states spend less than one-third of their long-term care dollars on home- and community-based supports—with the majority of funds going to nursing home care. However, as states adopt managed care models for long-term services to achieve savings, community and home care is more likely to be covered. In fact, states with mature managed care programs ranked highest on the Scorecard. Ms. Woodcock cautioned that there are still few evaluations of these programs and limited research on best practices. Still, she is hopeful that many of the provisions in the Affordable Care Act will give states the opportunity to continue to "rebalance" and expand upon the quality and delivery of LTSS.
As the president of the largest nonprofit home care agency in the U.S., Carol Raphael offered a provider's perspective. She described the challenges providers face in coordinating care for elderly and disabled adults, many of whom are dually eligible for Medicaid and Medicare, and most of whom suffer from at least three chronic conditions and often the same number or more functional deficits, including cognitive impairments and behavioral health problems. She also highlighted workforce issues, observing that almost 90 percent of home health aides leave after two years due to low pay and poor working conditions.
Ms. Raphael, who is also co-chair of the long-term care workgroup for the New York Medicaid Redesign team, discussed states' options for expanding managed care in an effort to reduce costs and increase quality and efficiency in Medicaid, given budgetary constraints and misaligned incentives for providers dealing with dual eligibles. In order to have a truly integrated system to meet peoples' long-term needs, she said the country must cultivate a competent and committed workforce, develop an efficient and affordable delivery system, and incorporate informal caregivers into the system.
The briefing concluded with a robust discussion on properly managing and integrating care for individuals in both Medicare and Medicaid. Speakers emphasized that while there are some cost savings to be had by better integrating care, typically people using LTSS represent a "sicker" population, with more medical and functional problems than the average Medicare beneficiary and therefore higher health care bills. Ms. Woodcock and Ms. Raphael stressed the need to simplify the system by providing patients with one insurance card that would cover all services.
During the discussion, an audience member asked a question about the future of the Affordable Care Act's CLASS (Community Living Assistance Services and Supports) Program, given some policymakers' concerns about its fiscal viability. While no one on the panel felt able to predict the future of this program, they all agreed that long-term insurance, along with affordable services in general, is important: the Scorecard found the average cost of nursing home care exceeds 240 percent of the average annual household income of older adults.
For more information on this briefing, including speaker biographies, additional resources, and video of the event, please visit the Alliance for Health Reform Web site.





