Data Brief
As the U.S. population ages and lifespans increase, informal caregiving by family members has become a vital component of the health care delivery system. A recent national study estimates the value of unpaid caregiving at approximately 19 percent of total health care expenditures, or $194 billion. Women continue to provide the majority of this informal caregiving, even though most working-age women now participate in the work force. The trend toward smaller families and more working women, however, is beginning to strain the supply of potential caregivers.
The Commonwealth Fund 1998 Survey of Women's Health probed the extent of women's caregiving roles, enabling comparisons by income, health, and access to health care. The survey finds that although women across all income groups are almost as likely to fill a caregiving role, lower-income caregivers are less likely to have opportunities for a respite from their responsibilities. Overall, women caregivers themselves are often in need of care: they report relatively high rates of poor health, disability, and depression.
Nearly One of 10 Women are Primary Caregivers
Today, 9 percent of American women—more than 9 million women—and 4 percent of men are caring for a sick or disabled child, spouse, parent, or other relative, based on the survey. The already significant proportion of the population who serve as informal caregivers is likely to increase substantially as baby boomers age. According to the U.S. Bureau of the Census, by 2020 the number of elderly over age 80 is expected to rise by nearly 50 percent, leading to a dramatic increase in people living with chronic conditions and needing longterm care.
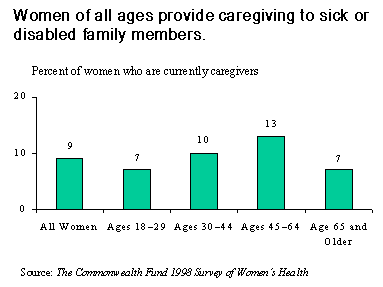
Caregiving cuts across all demographic groups.Women with annual incomes above the national median of $35,000 are about as likely as women below the median to be caregivers (9% vs.11%),and white women are as likely as minority women to be caregivers (9% vs. 10%). Similarly, single women (8%) and divorced, separated, or widowed women (7%) are almost as likely as married women (11%) to be caregivers. Women of all ages care for sick or disabled family members. Rates are highest among women ages 45 to 64—perhaps because they are more likely to have elderly parents.
Lower-Income Woment Devote Substantial Time to Caregiving with Little Respite
Caregiving requires a substantial commitment of resources and time. Nearly one-third of all caregivers (31%) report a decrease in their family's savings because of caregiving responsibilities. Overall, two of five women caregivers devote more than 20 hours per week to caring for a sick or disabled family member. This time burden falls most heavily on women in the bottom half of the income distribution. More than half (52%) of women caregivers with incomes $35,000 or below spend in excess of 20 hours each week providing care. Reflecting this larger time commitment, lower-income caregivers are almost twice as likely to care for a sick or disabled relative in their own home as caregivers with higher incomes (62% vs. 36%). In addition to their more intensive caregiving role, lower-income caregivers are half as likely as higher-income caregivers to have paid home health care or assistance available to provide support for and relief from their caregiving functions (18% vs. 35%). Among all caregivers, less than one-quarter have paid home health care to supplement the care they provide to a sick or disabled family member.
Impact of Caregiving on Health and Access to Health Care
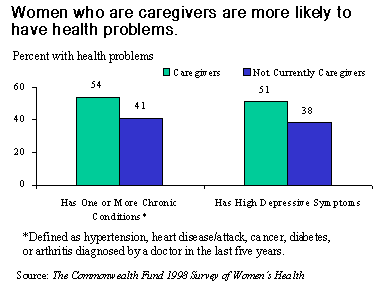
Oftentimes the caregiver is also in need of care. One-quarter (25%) of women caring for a sick or disabled family member rate their own health as fair or poor, compared with one-sixth (17%) of other women. More than half (54%) of women caregivers have one or more chronic healthconditions, compared with two-fifths (41%) of other women. In addition, half (51%) of all caregivers exhibit high depressive symptoms, while 38 percent of other women do so.
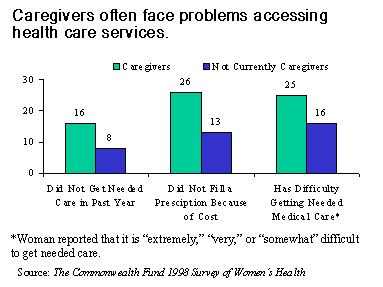
Perhaps because of the significant time and expense that caring for others demands, women caregivers are also at risk for encountering barriers to health care. Compared with other women, caregivers were twice as likely in the past year to not get needed medical care (16% vs. 8%) and not fill a prescription because of the cost (26% vs. 13%). One-quarter (25%) of women who were caregivers has difficulty getting medical care, versus one-sixth (16%) of other women.
With shorter hospital stays becoming more common, discharged patients may require a more intensive level of care over a longer period upon their return home. According to the survey, one-third of family members hospitalized in the past year required care at home following their discharge. One-third of the women and one-quarter of the men interviewed said they were the caregiver for their sick family member; three of 10 women and men reported that their family paid someone to provide this post-hospital care.


