Children in the Medicaid Program
States are required to cover all children under age 19 whose family income is below the federal poverty level ($19,350 for a family of four in 2005) and all children under age 6 whose family income is 33 percent above poverty.1 Many states opt to cover additional children (Figure 1).
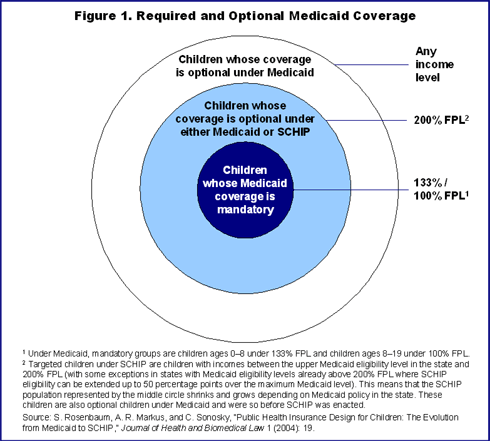
- Medicaid pays for over one-third of all U.S. births, making the program the single largest insurer of prenatal, delivery, and newborn care, including neonatal intensive care.2
- Medicaid covers 30% of infants and young children, making it the largest insurer of well-baby care and preventive services for healthy development.3
- Medicaid enrolls over 70% of all poor children.3
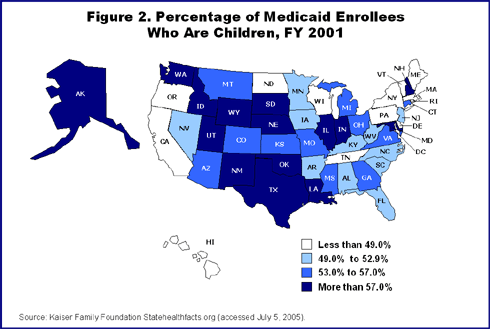
- Children make up 50% or more of the Medicaid population in most states (Figure 2).
Children with Special Health Care Needs
Like all children, those in Medicaid range from healthy children with modest needs to children with serious conditions and greater health needs in early childhood. Children with special health care needs have, or are at increased risk for, chronic physical, develop-mental, behavioral, or emotional conditions and require services beyond those required by children generally.4
Medicaid's Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) program offer the nation's most comprehensive coverage for children with special needs. Many enrollees have low income; qualify through Medicaid's special "spend down" program for medically needy persons; or qualify through the home and community care waiver program, which states use for children of any income level who have serious disabilities.
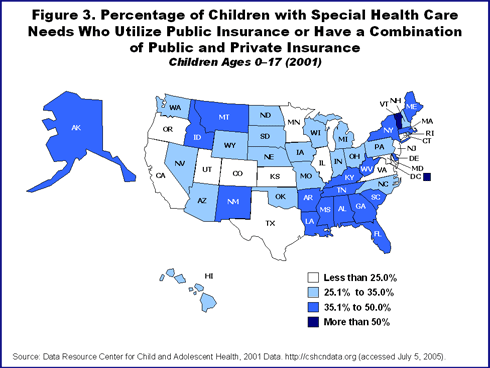
Nationally, 12.8 percent of children are considered to have special needs.5 These children depend on a combination of federal, state, and local programs to meet their needs (Figure 3).
EPSDT Aids Healthy Development of Special-Needs Children
EPSDT helps children with special health care needs in several ways:
- The program's comprehensive benefits include all services recognized as part of Medicaid's medical assistance definition, including rehabilitative services, extended inpatient care, physical and speech therapy, eyeglasses, hearing aids and other durable medical equipment, private duty nursing, medically necessary prescription drugs, and targeted case management.
- EPSDT covers treatments needed to ameliorate a condition that would affect a child's growth and development—a coverage standard far broader than those observed by commercial insurers.
Medicaid and Child Development Programs
Medicaid plays a key supporting role in child health and development programs. Medicaid covers a broad range of services and, unlike commercial insurance, will pay for care in settings that are not traditionally "medical." For example, Medicaid will pay for covered benefits when delivered in schools or early childhood development centers. Through EPSDT, Medicaid finances the health care component of programs that furnish educational and supportive services for children with special developmental needs.
Two key examples of child development programs supported in part by Medicaid are the Individuals with Disabilities Education Act (IDEA) and the Title V Maternal and Child Health Services Block Grant (Title V). IDEA requires states to ensure a free, appropriate public education to children with disabilities.6 It also supports early intervention programs for infants and toddlers at risk for disability and delay. Under IDEA, schools must: 1) develop an individualized education plan that identifies the educational and supportive services a child needs; 2) provide related services that help the child benefit from education, including developmental support services, transportation, and necessary medical care; and 3) in the case of pre-school children receiving early intervention services, provide for the development of an individualized family service plan. In 2001, approximately 6.7 million children received IDEA services.7 IDEA does not provide states with funding for medical and health care needs. For this reason, federal law provides for payment under Medicaid for the health care services that may be identified in a Medicaid-enrolled child's education plan or family service plan.8 Similarly, IDEA requires that educational and early intervention programs coordinate with Medicaid.
The Maternal and Child Health Services Block Grant (Title V)
provides grants to states to support primary and preventive care for mothers, infants, and children, as well as health and supportive services for children with special health care needs. Administered through state health departments, Title V agencies serves more than 28 million mothers and children.
Federal Title V funds are modest. In FY 2005, state health agencies received $596.8 million in federal allotments. Thus, the success of Title V programs depends greatly on the extent to which Medicaid is available to fund the health care states need.
State Title V agencies also coordinate closely with Medicaid programs by aiding Medicaid programs in the development of benefits and pediatric health care standards, conducting outreach, paying for developmental and supportive services not covered by Medicaid, and helping to finance care for low-income women and children who may be ineligible for Medicaid or the State Children's Health Insurance Program (SCHIP).
1 Federal Register, vol. 70, no. 33, Feb. 18, 2005, pp. 8373–75.
2S. Rosenbaum, A. Markus, and C. Sonosky, "Public Health Insurance Design for Children: The Evolution from Medicaid to SCHIP," Journal of Health and Biomedical Law 2004 1(1):1–47.
3 B. Brown, M. Weitzman et al., Early Childhood Development in a Social Context: A Chartbook (New York: The Commonwealth Fund, Sept. 2004).
4 Maternal and Child Health Bureau, Health Resource and Services Administration, U. S. Department of Health and Human Services, http://mchb.hrsa.gov.
5 Data Resource Center for Child and Adolescent Health, http://cshcndata.org (accessed July 10, 2005).
6 The text of IDEA can be found at: 20 U.S.C. §1400 et seq.
7 OSERS's Annual Report to Congress, 2003, at http://www.ed.gov/about/reports/annual/osep/2003/25th-vol-1-sec-1.pdf.
8 20 U.S.C. § 1412(12)(a), § 1440; 42 U.S.C. § 396b(c).


