Executive Summary
Given the strong correlation worldwide between low income and poor health—including disability, chronic disease, and acute illness—it is especially critical for people with limited incomes to have ready access to medical care. Inequities in access can contribute to and exacerbate existing disparities in health and quality of life, creating barriers to a strong and productive life.
Low-income patients in any country are likely to be particularly vulnerable to policies related to health insurance. Gaps in coverage, patient cost-sharing, and limited benefits can all act as barriers to care. To the extent that higher income enables patients to avoid waiting lists, complex administrative processes, or community shortages, nonfinancial barriers may also contribute to inequities in care experiences.
Cross-national comparisons of health care experiences by income can help in the assessment of relative performance and can provide guidance to policymakers seeking to reduce health and health care disparities. To compare experiences in countries with different health insurance and care delivery systems, The Commonwealth Fund 2004 International Health Policy Survey interviewed adults in Australia, Canada, New Zealand, the United Kingdom, and the United States about their primary care experiences. A 2004 report based on the survey found shortfalls in the delivery of timely, effective, safe, or patient-centered care, with significant differences across all five countries. Although country rankings varied, on average the U.S. often ranked low, particularly with regard to stability of physician–patient relationships, concerns with coordination of care, and cost-related barriers.
This report goes beyond the averages to compare experiences within and across the five countries by income. The study examines how adults with below-average incomes fare within each country's health system and how their experiences compare with those of adults with above-average incomes.
Overall, the report finds a health care divide separating the U.S. from the other four countries. The U.S. stands out for income-based disparities in patient experiences—particularly for more negative primary care experiences for adults with below-average incomes. On most measures of primary care access, coordination, and doctor–patient relationships, below-average-income adults in the U.S. had the worst experiences compared with their counterparts in the other four countries. Only on selective preventive care measures did below-average-income adults in the U.S. fare better than in the other countries.
In the U.S., disparities—many of them wide—between below-average- and above-average-income adults' experiences were evident on 21 of 30 measures. At the other end of the spectrum, the U.K. was the most equitable in terms of reported care experiences. Compared with the U.S., there were also relatively few disparities by income in Australia, Canada, and New Zealand; in these countries, significant differences arose most often for access to services not fully covered by public insurance.
Among the five countries, the U.S. was unique in the extent to which differences by income extended to patient–physician care relationships and ratings. In the other four countries, lower-income and higher-income adults tended to report similar physician experiences.
The study also finds that uninsured adults in U.S. are at sharply elevated risk for access barriers, coordination gaps, and other primary care deficiencies. Yet, being uninsured is only part of the story: even when insured, below-average-income American adults under age 65 were more likely to report access problems and delays than insured, above-average-income adults.
Following are some key highlights from the study.
Low-Income Adults Across Five Countries
- Below-average-income adults in the U.S. ranked last on 16 of 30 measures of health care experiences. The more negative experiences spanned primary care access, coordination, and care ratings.
Compared with below-average-income adults in the other countries, those in the
U.S. were:
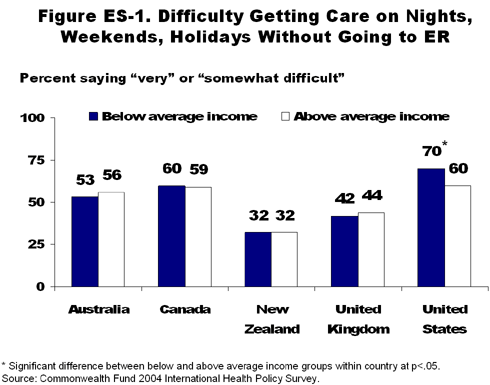
- the most likely to have difficulty getting care at night, during weekends, or on holidays without going to the emergency room (70% vs. 32%–60% in the other countries) (Figure ES-1);
- the most likely to go without care because of costs (57% vs. 12%–44% in the other countries);
- the most likely to report duplication of medical tests (17% vs. 5%–8% in the other countries); and
- the most likely to rate their doctor as fair/poor (22% vs. 9%–12% in the other countries).
The U.S. performs comparatively well on clinical preventive care measures, regardless of income level. In these indicators, U.S. below-average-income adults tended to lead rather than lag their counterparts in other countries.
Disparties by Income
- The U.S. stands out for pervasive disparities by income. On 21 of 30 measures, there were significant and often wide gaps between below-average- and above-average-income adults' experiences, with the former more likely to report negative experiences.
- In the U.S., significant gaps by income were seen across all but one access question, (i.e., did not have a regular doctor or place of care). Compared with above-average-income adults, those with below-average incomes were more likely to wait six days or more for an appointment with a doctor when sick (24% vs. 13%) and to go without needed care because of costs (57% vs. 25%). They were also more likely to have gone to an emergency room for care and to report difficulty getting care after hours.
- There were also significant disparities for coordination of care—including duplicate tests and delays in receipt of lab tests. Compared with above-average-income adults, those with below-average incomes were more likely to report duplication of medical tests (17% vs. 9%), lab test errors (19% vs. 10%), or delays in receiving test results (25% vs. 17%).
- The U.S. was the only country among the five in which below-average-income patients often reported more negative doctor–patient care experiences, including physicians' failure to listen or to explain or make goals of care clear.
- Lack of health insurance intensified disparities. In the U.S., uninsured adults often went without needed care and also experienced more fragmented and disconnected care.
- Uninsured adults were most at risk for access barriers to care: three of four reported going without care because of costs (76%) and difficulty getting care after hours (74%).
- Uninsured adults were also significantly more likely than those with insurance to report duplication of tests (23% vs. 10%), experience medical record delays (26% vs. 15%), not receive test results or have results clearly explained (31% vs. 19%), and report lab test errors (27% vs. 13%) (Figure ES-2).
- The survey findings also reveal that lack of insurance can undermine doctor–patient relationship and communication. Compared with insured U.S. adults, uninsured adults were significantly more likely to report negative experiences on all six key measures of doctor–patient relationship. They were also significantly more likely to leave the doctor's office without getting important questions answered (35% vs. 23%) and to rate their doctor as fair or poor (27% vs. 11%).
- Although gaps narrow with insurance, the study finds that below-average-income insured adults under 65 continued to report access problems at twice the rate of insured adults with above-average incomes.
- Even when insured, U.S. nonelderly adults still faced heightened access problems compared with nonelderly adults in the other four countries.
- Among the five countries, the U.K. health care system appears to provide the most equitable access. Differences by income across primary care measures were typically small, with few significant disparities. The U.K is also notable for protecting low-income adults, as well as high-income adults, against financial burdens.
- However, both below-average- and above-average-income adults in the U.K. lag behind other countries on clinical preventive care measures.
- Compared with the U.S., Australia, Canada, and New Zealand provide relatively equitable access to primary care. The income differences that emerged were associated with cost-sharing features or benefit gaps in national health insurance.

Summary
Despite health care spending that far outstrips that of the other four countries, the U.S. lags behind in provision of timely, patient-centered, and efficient care for its below-average-income population. The U.S. also stands out for systemic differences in access to care and primary care experience by income.In the U.S., health insurance coverage is associated with access to care and better care experiences. Uninsured adults were the most likely of adults in all five countries to go without care because of costs and to experience coordination problems that put their health at risk and undermine the efficiency of care. The cross-country findings further indicate that below-average income adults are likely to be particularly sensitive to insurance design, including cost-sharing and benefits. In Australia and New Zealand, disparities by income level emerged for services less well covered by national plans, despite fees that would be considered modest by U.S. standards. Within the U.S., the persistence of access problems among below-average-income adults with insurance coverage likely reflects the shift in insurance design toward higher deductibles and cost-sharing.
Finding policy solutions to extend coverage and improve primary care for lower-income adults is a critical step toward improving the performance of the U.S. health care system. The experiences of other countries indicate that it is possible to do better.


