Executive Summary
Since the late 1990s, accelerated growth in health care spending has translated directly into increased burdens on family budgets. Between 1996–97 and 2001–02, the average family's out-of-pocket (OOP) spending rose in direct proportion to total medical spending and nearly twice as fast as did family income. As a result, many more families now face high costs relative to income. When rising premium costs associated with employer-based coverage or nongroup insurance are added into the equation, even more families are devoting a substantial share of their resources to health care expenses.
By 2002, nearly one-quarter of all families and one of six nonelderly families devoted high levels of their total income on OOP plus premium costs. The rates were notably high among low- and modest-income working families. Having insurance reduced the likelihood of high OOP costs. But, here too, low- and modest-income families remained at risk for costs that were high relative to their incomes.
This report uses data from the Medical Expenditure Panel Survey (MEPS)—as did an earlier Commonwealth Fund report on this subject, Family Out-Of-Pocket Spending for Health Services: A Continuing Source of Financial Insecurity (Merlis 2002). MEPS is a household survey continuously conducted by the Agency for Healthcare Research and Quality, providing nationally representative data on health care utilization and spending, insurance coverage, and other characteristics of the civilian noninstitutionalized population.
Throughout the report, OOP costs include deductibles, coinsurance or copayments, and payments for services not covered by insurance. Health care costs including premium payments are featured in the final section.
Key Findings
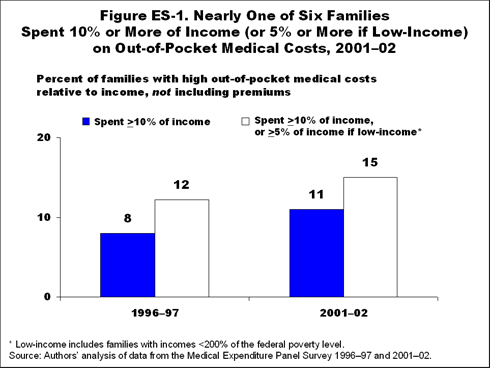
- In 2001–02, an average of 13 million families per year—11 percent of all families—had direct OOP costs equal to or exceeding 10 percent of family income, compared with 8 percent in 1996–97.
- Another 5 million families per year, with incomes below 200 percent of the federal poverty level, had direct costs equal to 5 percent to 10 percent of their income.
- Altogether, an average of 18 million families per year—made up of 35 million individuals—faced OOP medical care costs that were high relative to their incomes.
- The share of families with high OOP costs is up sharply since 1996–97, increasing from 12 percent with spending above the combined income thresholds to 15 percent in 2001–02.
When the family's share of private health insurance premiums is added to OOP spending for medical care, 18 percent of families had costs greater than 10 percent of income, and nearly one-fourth had costs above the combined threshold (i.e., OOP costs equal to or exceeding 10 percent of family income or, for families with income below 200 percent of the federal poverty level, costs equal to 5 percent to 10 percent of income) in 2001–02. This amounts to 27 million families.
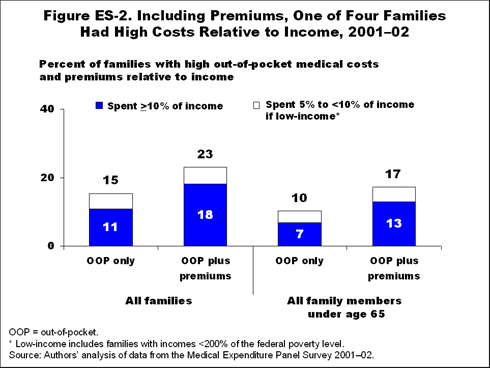
Families with any member age 65 or older were much more likely than other families to have high medical care and premium costs relative to income. This is partly due to gaps in Medicare benefits, such as the lack of catastrophic coverage and—in the period covered by this study—almost no coverage of outpatient prescription drugs. It is also due to the fact that beneficiaries pay part or all of the premiums associated with employer-provided or nongroup Medicare supplemental coverage. Still, 10 percent of families without elderly members—close to 10 million families—had high OOP medical care cost relative to their incomes. When premium costs are included, 17 percent had high costs relative to income. Because the gaps in health coverage for the elderly have been extensively documented, the remainder of this report focuses on nonelderly families—those without members age 65 or older.
Nonelderly Families: Poor Health and Low Income Place Families at Risk
As of 2001–02, an average of 9.5 million nonelderly families per year, consisting of 21 million people, had OOP expenses that were high relative to their family income, using the combined threshold.Health status. When any member of a nonelderly family has a health or functional problem, the family is much more likely to have high OOP costs. Families of people whose self-reported health or mental health is fair or poor are much more likely to have high costs than families with no problems. The same is true of families with a member who requires assistance with activities of daily living (ADLs), such as bathing or dressing, or instrumental activities of daily living (IADLs), such as cooking or paying bills.
Income. Nonelderly families with low incomes are much more likely to pay a high share of income for direct OOP costs. The disparity is especially large for low-income families reporting any health or disability problems. However, even low-income families with no such problems are paying high OOP costs relative to income.
Insurance coverage and coverage source. The prevalence of high OOP costs is growing most rapidly among fully insured nonelderly families—those in which all members have coverage throughout the year. As of 2001–02, nearly 10 million people in such families had expenses that were high relative to income. Prevalence of high costs is still higher when any or all family members go without coverage for all or part of the year. But fully insured families have seen a larger proportional increase, because their uncovered costs are rising faster than income.
Insurance and health status combined. Regardless of insurance coverage, having a family member with a health problem or ADL/IADL limitation significantly increases the likelihood that a family will have high OOP costs relative to income. Among nonelderly families with fully insured members, the incidence of high costs for families with health problems was close to four times as large as for families reporting no problems.
Persistence of high costs. Overall, 32 million people were in families with high OOP costs in 2001, 2002, or in both years. Of these, over 8 million people were in families with high costs in both years. Families with high direct OOP costs are much more likely than other nonelderly families to report that they went without needed services because they needed the money to pay for other necessities. They are also more likely to report that they postponed obtaining care or had other difficulties.
Adding in premiums. When family contributions to premiums for employer-based plans or other private coverage are added, the proportion of families with high costs relative to income rises markedly. The effect is especially notable for families with nonemployer coverage: two of five (40%) have high costs relative to income when both premiums and direct OOP spending are included. Even among families with employer coverage, an average of one of eight experienced high costs in 2001–02.
Conclusion
This report uses MEPS cost data through 2002. It is likely that spending on OOP and premium costs has been growing even more rapidly since then. Employee contributions toward family premiums increased by 27 percent between 2002 and 2005, and many employers have imposed similar increases in coinsurance and copayment levels. Medicaid beneficiaries have generally been protected against high costs, but the budget reconciliation bill that is scheduled for consideration by Congress in February 2006 will allow states to require more cost-sharing by many participants.Given these trends, it can be expected that many more families—especially low-income families—will need to devote a steadily larger share of their budgets to health care. Some may choose to drop their health insurance, while others will face increased debt and the threat of bankruptcy. Some analysts contend that requiring consumers to pay more of their own costs will encourage them to become more prudent or savvy users of medical services. Creating financial incentives for consumers may play some part in the solving the problem of growing health care costs, but it is also vital to ensure that the most vulnerable families are adequately protected against the risk of unsustainable medical bills.


