The goal of the Social Security Disability Insurance (SSDI) program is to provide a safety net for workers who must stop working because of a disability. There is, however, a significant hole in that safety net with respect to health care coverage and access to care: although Medicare coverage is available to people with disabilities, most beneficiaries must wait for that coverage until 24 months after their eligibility for SSDI begins. Previous studies have provided information about SSDI beneficiaries' characteristics, health insurance coverage, and experiences in accessing health care during the 24-month Medicare waiting period. Far less is known about the extent to which SSDI beneficiaries have adequate health care coverage and access during the years preceding their entry into the SSDI program.
In this study, we profile the characteristics, health insurance status, and health care access and utilization patterns of SSDI beneficiaries during the years before and after their entry into the program. Using data from the 1994–1996 National Health Interview Survey (NHIS) linked to SSDI, Medicare, and death records, we focus on SSDI beneficiaries during the three years prior to their SSDI entry and three years after entering the program. The study builds on the body of previous research on the 24-month Medicare waiting period after SSDI entry by more broadly examining the circumstances of SSDI beneficiaries in the years immediately before their eligibility for benefits. It considers a policy to expand Medicare to workers with significant medical conditions. The rationale for considering such policies is based partly on the work disincentives inherent in the current system for people with disabilities. For those with disabilities, lack of adequate coverage and access to care might contribute to their decision to stop working and instead apply for SSDI.
Characteristics. Even three years before entering the SSDI program, beneficiaries differ from other working-age adults in many respects: they are older; have lower levels of education; are more likely to be divorced, widowed, or separated; are more likely to be black; are more likely to be in laborer and service occupations and less likely to be in managerial/professional occupations; have lower average earnings; are in poorer health; are more likely to be uninsured; and have higher reported rates of health care access problems. Yet, in several important respects, beneficiaries observed three years before SSDI entry are similar to all working-age persons: they are about as likely to be employed, have health coverage through their own employment, live in households with incomes below the federal poverty level, and have Medicaid coverage.
Sources of Health Insurance. Among beneficiaries observed during the years prior to SSDI entry, a large share (about 22%) was uninsured (Table ES-1). By contrast, about 16 percent of the general population of adults ages 18 to 64 is uninsured. Rates of uninsurance remain fairly constant and high until the second year after SSDI entry. By the third year after entry, only a small share of SSDI beneficiaries reports being uninsured, primarily because all of them have become eligible for Medicare. The non-Medicare sources of health insurance coverage change from the period before SSDI entry to the period after: there is a marked decline in coverage obtained through beneficiaries' own employment, a less-marked decline in coverage obtained through a family member, and a marked increase in reliance on Medicaid.
|
Prior to SSDI Entry |
After SSDI Entry | ||||
|
25–36 |
13–24 |
1–12 |
1–12 |
13–24 |
25–36 |
Source of Health Insurance (%) |
|
|
|
|
|
|
None (uninsured) |
22 |
21 |
23 |
23 |
17 |
4 |
Medicaid |
6 |
7 |
8 |
17 |
21 |
29 |
Own employer |
40 |
41 |
37 |
26 |
21 |
16 |
Family member employer |
39 |
37 |
33 |
30 |
35 |
31 |
Note: SSDI beneficiary cohorts include NHIS sample members ages 18–64 who became entitled to SSDI based on their own work histories within 36 months (before or after) the month the household was interviewed in the NHIS. The SSDI entitlement (entry) month is based on the date associated with the latest entitlement occurring during the 36-month period before and after the interview month. Coverage status could not be ascertained for approximately 10 percent of sample members in each SSDI 12-month group. Percentages do not sum to 100 because not all sources are shown, and because individuals may have multiple sources of coverage.
Poverty. Prior to SSDI entry, the poverty rate among beneficiaries is comparable to the rate for all working-age adults. Immediately after SSDI entry, poverty rates among beneficiaries jump, with rates in the years after entry nearly doubling from those in the years before.
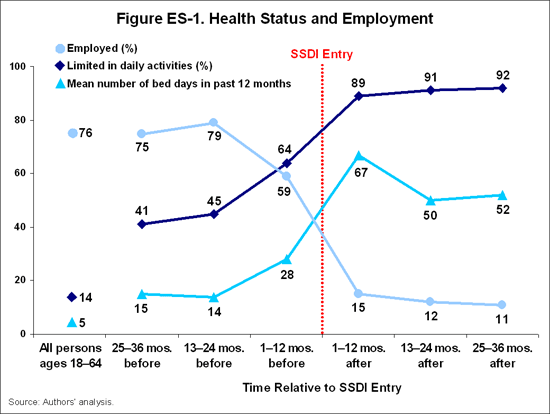
Health Status and Employment. During the years leading up to and following SSDI entry, many beneficiary characteristics change, primarily in ways that might be expected to accompany the onset or worsening of a disabling health condition. There is a marked decline in health status (based on a number of indicators) and a marked decline in employment (Figure ES-1). But even three years prior to SSDI entry, a large share of eventual beneficiaries report activity limitations (41%) relative to all working-age adults (14%).
Mortality. Mortality rates during the first three years after SSDI entry are high. For those beneficiaries observed in the NHIS before entry, the cumulative mortality rates by the 13th, 25th, and 37th month after entry are approximately 9 percent, 13 percent, and 15 percent, respectively. One implication of this finding is that an estimated 13 percent of entrants never receive Medicare benefits, even though they likely contributed to Medicare’s financing for many years.
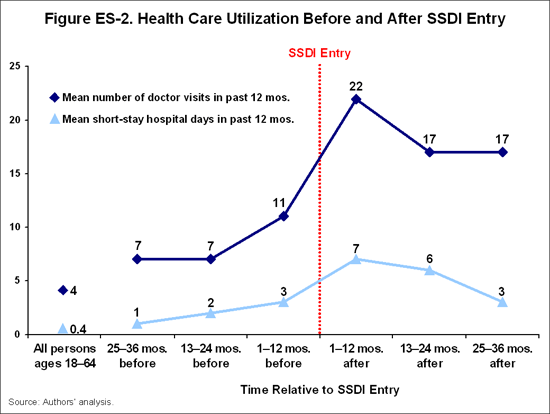
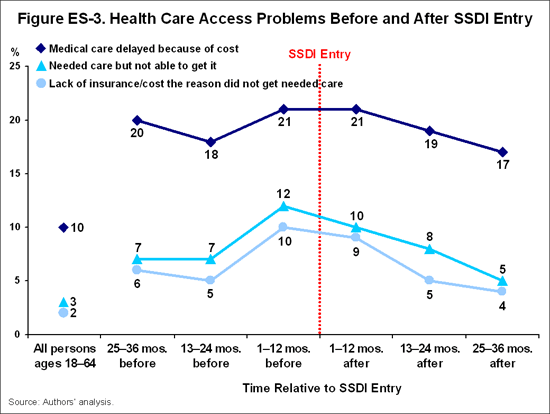
Health Care Utilization and Access. At the same time beneficiary health status is declining, there are increases in health care utilization and reported health care access problems (Figures ES-2 and ES-3). Beneficiaries experience problems accessing care at rates that are two or more times those of all adults ages 18 to 64. Rates of health care utilization and access problems follow a pattern of gradually increasing and peaking during the year before and the year after SSDI entry, then declining somewhat thereafter. Using a logistic regression model, we find that poverty, poor health, and lack of health insurance are significant predictors of cost-related health care access problems among beneficiaries, with lack of insurance having the largest effect.
Medicare Waiting Period. The majority of beneficiaries in our sample entered SSDI retroactively; that is, the month in which their application was allowed was after the first month in which they were entitled to benefits. Because of the length of time it takes for SSDI applications to be reviewed and approved, many beneficiaries receive benefits that are retroactive to the first month they were entitled to receive them. For example, a person may find out in May 2009 that she is eligible for SSDI benefits as of July 2008—the first benefit check (presumably received in June or July 2009) would include retroactive benefits back to July 2008. The Medicare waiting period begins the first month beneficiaries are entitled to benefits. About one-third of SSDI entrants had completed 12 months or more of the Medicare waiting period by the time their SSDI claim was allowed, including 11 percent who had completed the entire 24-month waiting period. Therefore, while elimination of the waiting period for Medicare would help many SSDI beneficiaries, it would be of less help to those with significant health care needs who are waiting review of their SSDI claims—even if Medicare benefits were awarded retroactively. This is because their health care decisions would have been made in the absence of having the Medicare coverage. Of course, elimination of the waiting period also would not provide access to care during the months and years leading to SSDI entry.
The findings diminish some of the arguments justifying the Medicare waiting period. They suggest that private insurance crowd-out due to the extension of public coverage would be limited to a minority of beneficiaries: those with inferior private coverage and those for whom COBRA, with its high premiums, was the only coverage option—less than one-third of all beneficiaries in the waiting period. Our estimates indicate that it would cost about $12 billion per year (based on program year 2006) to eliminate the Medicare waiting period (including the costs for Medicare Parts A, B, and D) (Table ES-2). While a substantial sum, this is only a small share (3%) of all Medicare program expenditures. This estimate assumes that Medicare coverage would be retroactive to the month of SSDI entitlement. If Medicare coverage was not retroactive to the entitlement month, the annual cost of eliminating the waiting period would be approximately $7 billion.
Component |
Estimate |
Annual cost of eliminating the Medicare waiting period net of federal Medicaid savings (range) |
$11.1–$11.9 billion |
Annual cost of eliminating the Medicare waiting period net of federal Medicaid savings if coverage were not retroactive to SSDI entitlement date (range) |
$6.9–$7.4 billion |
* See Appendix C in full report for details of the cost estimation methodology.
Other Policy Options. We provide cost estimates for policy options that would expand access to Medicare to other groups of workers and former workers with significant medical conditions that might eventually lead to SSDI eligibility. The rationale for considering such policies is partly to reduce the work disincentives inherent in the current system and partly to address health insurance market failures and current trends in employer-sponsored health insurance coverage that result in limited access to health care among workers with significant medical needs. Earlier and more consistent access to health care for such workers might reduce or delay their exit from the labor force and application for SSDI. Our analysis finds that, while expanding coverage to broader populations of workers with significant disabilities would be costly, individuals and employers now spend considerable sums on the health care of workers with disabilities. A very large share of the costs of expanding Medicare coverage could potentially be financed from this pool of private funds under a well-designed worker/employer premium system. in which workers and employers share the costs of Medicare premiums.
Governments of several states are taking steps to reduce the number of uninsured, but it is not yet clear whether these efforts will help individuals gain and retain health insurance. Federal policymakers are also debating the need for mechanisms to address uninsured Americans. It is uncertain whether these efforts will aid those with disabilities who are struggling to obtain coverage for their often intensive health care needs. One important criterion for judging the adequacy of any proposal to cover the uninsured is the extent to which it will meet the needs of workers with significant health conditions—and whether it will continue to meet their needs if they must exit the labor force and apply for SSDI.


