When Hurricane Katrina hit the greater New Orleans area on August 29, 2005, it devastated the local health care system. Access to primary care and behavioral health services was severely limited. The Medical Center of Louisiana at New Orleans, the city’s large safety-net hospital system, was flooded and forced to shutter its doors for 14 months, devastating the city's health care infrastructure. The Charity Hospital building, which is part of the historic safety-net clinic complex, remains closed to this day. The city’s inpatient bed capacity plummeted by more than 50 percent, and the number of ambulatory care clinics declined from 90 to 19. The disruption in care also caused a massive dislocation of the health care work force. An estimated 4,500 physicians were temporarily dislocated by the storm, approximately 35 percent of them primary care physicians. While the number of physicians per resident has improved, the ratio is still below pre-Katrina levels.
With the closure of the major public hospital and its adjacent ambulatory care sites, several nonprofit health care organizations stepped into the void to help care for the city’s poor and uninsured. What has emerged is a growing network of independent, neighborhood primary care clinics. In 2007, the U.S. Department of Health and Human Services awarded the state of Louisiana a $100 million Primary Care Access and Stabilization Grant, or PCASG, to restore and increase access to primary care by stabilizing and expanding this growing neighborhood system of primary and behavioral health care. The specific goals of the grant are to increase access to care, develop sustainable business entities, provide evidence-based, high-quality health care, and develop an organized system of care. The state selected the Louisiana Public Health Institute (LPHI) to administer the grant as the state’s local partner. As such, LPHI is responsible for devising a payment methodology in collaboration with federal and state governments, disbursing grant dollars, and providing or arranging for technical support for quality and process improvement. In the wake of the devastation of Katrina came an opportunity to test a new model for organizing primary care for the poor and uninsured in New Orleans.
In an effort to assess the quality of care given to patients who are served by the burgeoning network of clinics receiving PCASG funding, The Commonwealth Fund conducted a survey of a sample of clinic patients in 2009, 18 months after the initial PCASG funds were disbursed. This report examines the patients' experience with access, coordination, preventive care, chronic-disease management, and relationships with personal clinicians. The goal of the survey is to monitor federal and local efforts intended to reorganize the primary care infrastructure following Hurricane Katrina and to determine the impact of those efforts on patients. The report should help to keep national attention on the devastation of Hurricane Katrina and its long-term effect on health care services. Simultaneously, the findings can provide valuable lessons for national and state leaders interested in strengthening primary care for extremely vulnerable patients.
Key Findings
Clinics in New Orleans serve a particularly vulnerable population, yet few patients forgo necessary care or report inefficiencies in care.
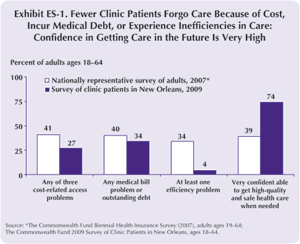
Although more and more families across the country have seen their health insurance coverage deteriorate and medical bill problems or cost-related delays in getting needed care escalate, the survey finds that fewer clinic patients forgo care because of cost or have accumulated medical debt than adults in the country as a whole (Exhibit ES-1). Even though health care expenses continue to rise as a share of income across the country and within all income groups, the New Orleans clinic patients express greater confidence than most patients elsewhere in the country in their ability to afford the health care that would be needed if they were to develop a serious illness.
As patients of free or low-cost care clinics, survey respondents would be expected to experience fewer problems accessing care and lower medical debt burden than the general population who may not have the same access to free or low-cost care. Still, these findings are striking given that the vast majority of clinic patients are uninsured during the year (72%), low-income (51% of respondents have incomes below 200% of the federal poverty level), and minority (89%). Clinic patients’ reports of fewer problems paying medical bills affirm the value of providing care regardless of ability to pay in staving off unmanageable debt burdens in low-income and uninsured patient populations. Indeed, the study results are a testament to the fact that it is possible to deliver well-organized, high-quality, efficient, and sustainable care for the poor and uninsured.
Nearly four of 10 clinic patients have an "excellent" experience, nearly nine of 10 patients reported they had enhanced access to care, and more than three-quarters reported excellent patient–clinician communications.
In order to assess the quality of patients' clinical experiences, this study measured how patients evaluated all four components of what can be considered a well-organized, patient-centered system of care: 1) having a clinician in the clinic who understands important information about the patient's medical history; 2) experiencing no difficulty contacting their clinician by telephone during regular practice hours or in getting care or medical advice on weekends or evenings or in being given same- or next-day appointments when sick; 3) having a clinician who helps coordinate or arrange care to be delivered by other doctors, including helping patients decide which specialist to see and interpreting information received from specialists; and 4) having a clinician in the clinic who always listens carefully, explains things in a way the patient can understand, spends enough time with the patient, involves the patient in treatment decisions, and never leaves the patient with unanswered questions about treatment.
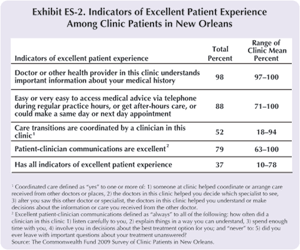
In total, using these indicators, nearly four in ten patients (37%) evaluated all four components positively and thus could be considered to have an "excellent patient experience." (Clinic averages for excellent patient experience ranged from a low of 10 percent to a high of 78 percent at different facilities.) According to study findings, almost all clinic patients said that the doctor or health provider in the clinic understood important information about their medical history (Exhibit ES-2).
Nearly nine of 10 patients (88%) reported that they had easy access to care, and as many as eight of 10 (79%) patients reported excellent patient–clinician communications. Fewer patients (52%) reported that a clinician coordinated the care they received in the clinic with care from other places or physicians, including specialists.
Adults with a suboptimal patient experience are at a disadvantage for receiving preventive services.
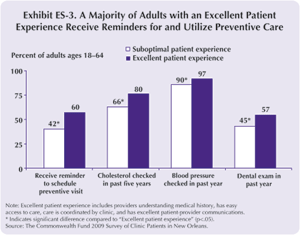
The Commonwealth Fund survey finds that adults who report “excellent patient experiences” are significantly more likely to receive reminders from their doctors to make appointments for preventive care visits, and they are also more likely to get preventive care, including cholesterol and blood-pressure checks and cancer screenings (Exhibit ES-3).
- Six of 10 adults with an excellent patient experience received reminders about preventive care compared with just 42 percent of adults with a suboptimal patient experience.
- Adults with an excellent patient experience have significantly higher rates of cholesterol screenings than adults with suboptimal patient experiences (80% vs. 66%).
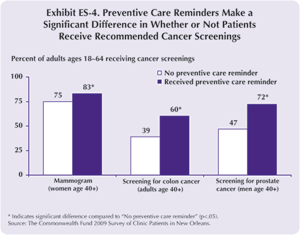
- Patients who receive reminders to make appointments for preventive care have significantly higher rates of screening tests for breast cancer (83% vs. 75%), colon cancer (60% vs. 39%), and prostate cancer (72% vs. 47%) than those who do not receive them (ES-4).
Chronically ill adults with an excellent patient experience are more likely than those with suboptimal experiences to have their conditions well managed.
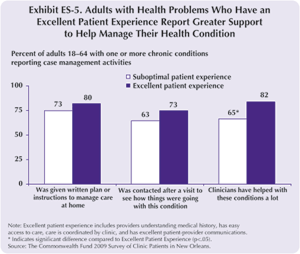
New Orleans clinics are working hard to provide high-quality primary care to their chronically ill patient population. The survey finds that chronically ill adults are significantly more likely than those with no chronic conditions to have an excellent patient experience (40% vs. 33%, data not shown). It also finds that those who report having an excellent patient experience feel more supported by clinicians who help manage their chronic conditions (Exhibit ES-5).
- Nearly three-fourths of adults (73%) with an excellent patient experience were contacted by a clinician after a clinic visit to see how things were going compared with 63 percent of adults with a suboptimal patient experience.
- A large share (82%) of chronically ill adults with an excellent patient experience indicated that clinicians had helped them manage their conditions, while just over six of 10 (65%) adults with a suboptimal patient experience felt clinicians had helped them manage their conditions.
As the health care sector of New Orleans re-forms and recovers in the aftermath of Hurricane Katrina, a new organizational structure for primary care is being tried—shifting from a large, hospital-based provider to a network of independent, neighborhood primary care and behavioral health clinics. The patients' responses to the change are encouraging thus far and suggest that the new paradigm can effectively meet the primary care needs of New Orleans' most vulnerable patients. The findings can inform federal, state and local policymakers' deliberations after PCASG grant funding ends in 2010 about how best to support a viable primary care infrastructure in Greater New Orleans in the future. In addition, building a stronger system of primary care is a central strategy of the leading federal health care reform proposals currently under consideration. In general, a comprehensive approach to improving primary care that is carefully planned and locally implemented—with ample support for primary care sites through financial incentives, common data-reporting requirements, and technical assistance—has the potential to improve primary care and to improve health outcomes for our nation's most vulnerable populations.