Evidence of racial disparities in access to health care is well documented, with studies noting inequities for a wide array of conditions, medical treatments, and care settings. Coronary artery bypass graft (CABG) surgery, in particular, has received much attention recently, with researchers focusing on inequalities between minorities and non-minorities in terms of access, outcomes, and care practices.
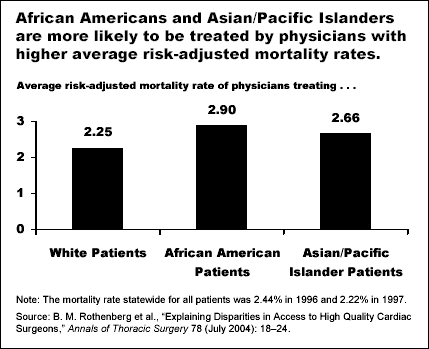
In the article "Explaining Disparities in Access to High Quality Cardiac Surgeons," (Annals of Thoracic Surgery, July 2004) researchers from the University of California, Irvine and the University of Rochester School of Medicine and Dentistry, with support from The Commonwealth Fund, find that African Americans and Asian/Pacific Islanders were more likely to be treated by surgeons and hospitals with higher risk-adjusted mortality rates than whites. This finding suggests that policy makers must improve access to high-quality providers when addressing health care disparities.
The researchers sought to explain the inequities by investigating several factors surrounding CABG surgeries. Specifically, the study considers whether the observed racial differences in access to high-quality surgeons were due to socioeconomic differences, racial differences in referrals to high-quality hospitals, or racial differences in referrals to low-volume surgeons.
Past studies have shown widespread disparities in access, outcomes, and quality of care. Among patients at Duke University, for instance, African Americans were 32 percent less likely to undergo CABG surgery than whites, even after controlling for severity of disease and other factors. Minorities are also more likely to experience worse health outcomes. In New York, minorities are more likely to be readmitted for complications following CABG.
In addition, care practices, like the administering of beta blockers following an acute myocardial infarction, or quality of providers (physicians and hospitals) can vary with the race of patient. This means that minorities may be disadvantaged even when they gain access to care.
About the Study
The researchers in this study examined a sample group of 27,969 patients who underwent CABG surgery in New York State in 1996 and 1997. These data were then augmented with risk-adjusted mortality rates calculated by New York State. This rate, which is interpreted as a measure of the quality of the surgeon, reflects the average performance of a surgeon relative to his or her peers after taking into account differences in disease severity and comorbidities (e.g., ejection fraction). Patients treated by surgeons with lower risk-adjusted mortality rates are assumed to receive better care than those treated by surgeons with higher risk-adjusted mortality rates.
Data Findings
The data show that African Americans and Asian/Pacific Islanders were significantly more likely to be treated by surgeons and hospitals with higher risk-adjusted mortality rates than were whites. Specifically, African Americans were treated by surgeons with risk-adjusted mortality rates 13.8 percent higher and Asian/Pacific Islanders were treated by surgeons with risk-adjusted mortality rates 17 percent higher than whites. The differential in risk-adjusted mortality rates between whites and minorities translates to an additional 170 minority deaths per year on a national basis. The impact is likely not limited to these 170 deaths. Because the risk-adjusted mortality rate is indicative of quality in general, it could extend to adverse outcomes other than in-hospital mortality, like complications or 30-day mortality.
Questions of Inadequate Risk Adjustment
The researchers counter the contention that race is a risk factor in predicting CABG mortality and that their findings simply reflect inadequate risk adjustment for race. Using data from their own analyses, and from other studies of CABG mortality, the researchers found that connections between race and CABG mortality is tenuous, present in only some samples, and not robust to choice of clinical risk factors. To further eliminate potential factors of inadequate risk adjustment, the authors examined the distribution of African American patients across physicians to determine whether a disproportionate number of minority patients were flocking to the same surgeons, dominating their practices, and possibly skewing results. In 1996, the mean percentage of African Americans in surgeons' practices in New York State (excluding surgeons with fewer than six CABG patients per year) was 7.8 percent. The researchers repeated their analyses excluding the top 5 percent of surgeons with the most African American patients (i.e., those with more than 18 percent African American patients) and found similar results before and after these surgeons were excluded.
Hospital Choice, Socioeconomic Status, and Surgeon Volume
Choice of hospital was the factor with the most significant impact of the variables considered in the study. Approximately 50 percent to 60 percent of the association between race and surgeons' risk-adjusted mortality rates is explained by the hospitals where the patients were treated. However, hospital choice does not fully explain the disparity in access to high-quality surgeons, the researchers say. The two remaining factors, socioeconomic status and surgeon volume, had only a minimal effect on the relationship between race and surgeons' risk-adjusted mortality rates. The importance of hospital choice in explaining the racial disparities in the study suggests that general referral patterns may be important determinants of where minorities receive treatment, the authors write. These patterns likely depend on many factors, including geographic proximity of patients to hospitals and the referral networks of the health care system within which patients receive their care. Such referral patterns may contribute to the disparities between groups. The researchers suggest that policy interventions may need to address the factors underlying these patterns.
Improving access to high-quality providers may also help lower the disparity in utilization, as well. If minorities tend to be treated by lower-quality providers, they would have lower expectations of favorable outcomes compared with non-minority patients. These expectations, in turn, may lead to an increased reluctance to undergo treatment. Addressing disparities in access to high-quality providers may have the added benefit of decreasing the disparity in procedure rates.
Conclusions
Eliminating racial and ethnic disparities in health care will require addressing not only the disparities in access to care but also the disparities in access to high-quality providers. The policy agenda should be expanded to include these issues of quality and to identify the factors that present barriers to access to high-quality care providers.


