Nursing home residents are being prescribed antipsychotic drugs at an increasingly high rate. According to a Commonwealth Fund–supported study in the Archives of Internal Medicine, more than one of every four Medicare beneficiaries in nursing homes (28%) received antipsychotics in 2000–2001—the highest reported rate in nearly a decade.
After a period of marked decreases, antipsychotic drug prescribing in nursing homes has been rising again, says a team of researchers led by Becky Briesacher, Ph.D., of the University of Massachusetts Medical School. In "The Quality of Antipsychotic Drug Prescribing in Nursing Homes,"(Archives of Internal Medicine, June 13, 2005), Briesacher and colleagues find that antipsychotics have become the most costly drug class for Medicaid programs, the main payer of medications prescribed in nursing homes. In 2001, the researchers say, Medicaid spent over $3 billion for antipsychotics, more than it spent on antimicrobial agents, cardiovascular drugs, or antidepressants.
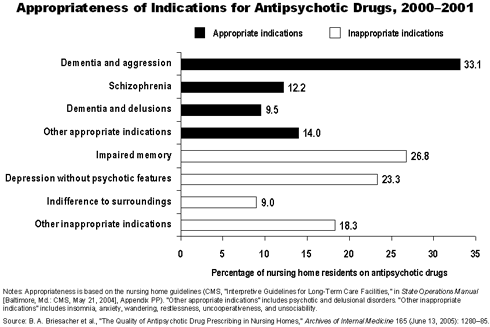
This increase may be attributed to the availability of second-generation antipsychotics, known as "atypical" agents, which have replaced older drugs and may be prescribed for a wider range of indications. However, this increase raises concerns about quality of care, the researchers say, especially when the drugs are not prescribed in accordance with guidelines. Most atypicals have shown to be effective in treating schizophrenia, but in nursing homes they are increasingly prescribed for other, less appropriate conditions, like memory problems, nonaggressive behaviors, or depression without psychotic features.
Methods
The research team set out to determine the extent of antipsychotic prescribing in nursing homes, as well as the appropriateness of this prescribing and the outcome of treatment. They used nationally representative data from the 2000–2001 Medicare Current Beneficiary Survey, along with diagnostic information from Medicare claims; drug name, dose, and scheduling data; and health and behavioral assessments from the Minimum Data Set. The study sample included 1,263 individuals.
Results
Of the 693,000 nursing home residents who received antipsychotics, more than one-half (58%) took doses exceeding maximum levels, received duplicative therapy, or had inappropriate indications. While the most common reasons for prescribing antipsychotics were dementia with aggressive behaviors and schizophrenia (both appropriate indications), one-third of residents had inappropriate indications including impaired memory and depression. Prescribing for these conditions has been strongly discouraged by a recently convened panel of experts.
Nearly 197,000 nursing home residents received excessive doses of antipsychotics, although the high doses were slightly more common with appropriate indications than with inappropriate ones (32% vs. 24%). Around 13 percent of all drug users received both conventional drugs and atypical agents; in one-third of these cases, this amounted to duplicative therapy. Most residents receiving antipsychotics in compliance with guidelines experienced no change or stable symptoms (83%), while a smaller amount improved (6%) and others deteriorated (12%). Residents with dosing and/or indication violations showed similar levels of behavioral change.
Conclusions
Appropriate use of antipsychotic drugs in nursing homes has been an issue since a 1986 report by the Institute of Medicine cited widespread misuse of these agents to sedate or discipline residents. After Congress passed the 1987 Omnibus Budget Reconciliation Act (OBRA-87) to create oversight of these medications, there were marked declines in their use. This study, however, finds that reported rates of antipsychotic prescribing are the highest they have been in a decade and within the range of rates documented prior to the passage of OBRA-87.
While the compliance issues may represent justifiable differences of opinion between practicing physicians and the nursing home guidelines, the researchers believe this subject merits additional investigation. "There are considerable gaps between the medications clinical evidence recommends and the medications clinical practice delivers," they say. With Medicare preparing to inherit Medicaid's role in paying for prescriptions for this population, now is an opportune time to evaluate the current uses of antipsychotics in nursing homes and the role of prescribing guidelines.
Facts and Figures
- In 1999, 19 percent of nursing home residents received antipsychotic drugs compared with 16 percent in 1995.
- During the study period, more than 200,000 nursing home residents received antipsychotic drugs but did not have appropriate indications.
- Nearly 40 percent of the study population using antipsychotic drugs still regularly resisted taking medications or eating meals.