In the Literature
While individuals who qualify for both Medicare and Medicaid represent a relatively small share of the population—about 7 million Americans in 2000—they consume a disproportionate amount of health care resources. In 2000, "dual eligibles" accounted for 24 percent of total Medicare spending, and, in 2002, 42 percent of Medicaid spending. Not surprisingly, they are often the focus of fiscal struggles between the federal and state governments, with each side looking to shift its responsibilities to the other.
Yet despite the attention they receive, many dual eligibles still struggle with unmet long-term care needs, a Commonwealth Fund–supported study finds. In "Unmet Long-Term Care Needs: An Analysis of Medicare-Medicaid Dual Eligibles" (Inquiry, Summer 2005), researchers report that dual eligibles who do not get help with basic life tasks face serious—and sometimes dire—consequences, like falling, being unable to bathe, or going hungry. The authors, Harriet Komisar, Ph.D., and Judith Feder, Ph.D., of Georgetown University, and Judith Kasper, Ph.D., of Johns Hopkins University, examined data from a 1999 survey, cofunded by the Robert Wood Johnson Foundation, of community-based (i.e., not living in nursing homes) elderly dual eligibles in six states: Georgia, Iowa, Massachusetts, New Jersey, Washington, and Wisconsin.
About Dual Eligibles
Community-based elderly dual eligibles are disproportionately poor, sick, and living alone. The survey found that many (77%) are women and over one-half are widowed. Nearly one-quarter have household income of less than $5,000 per year, and 87 percent have annual income of less than $10,000. The most common services that Medicaid covers for dual eligibles are long-term care and prescription drugs.
Health and Long-Term Care Needs
Health care problems are common among dual eligibles. One-half of the survey respondents said they are in fair or poor health. Ninety-two percent reported at least one chronic condition and one-half reported three or more. Most (88%) take prescription medication and over one-third (35%) take five or more prescription drugs.
In addition to medical care, one-third (32%) of these community-based dual eligibles require long-term care—that is, help from another person with activities of daily living (ADLs), like bathing, dressing, eating, using the toilet, getting out of bed or chairs, and moving around inside the house. One of seven respondents needs help with at least three ADLs.
Access to Care
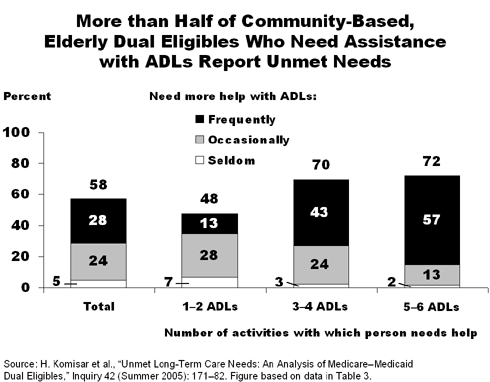
Very few community-based dual eligibles have problems obtaining medical care. Only 3 percent report not having a regular physician or other regular sources of care. In addition, while many report financial hardships, only 4 percent said they delayed getting medical care or went without medications because of financial problems. However, the survey results are more troubling, say the authors, when it comes to the provision of long-term care services. There are widespread shortfalls, with more than one-half (58%) of respondents who need assistance with ADLs reporting unmet needs.
These unmet needs can result in serious problems. Overall, 56 percent of people with unmet needs for help with ADLs reported at least one of the following five adverse consequences: not being able to bathe or shower, not being able to put on clean clothes, falling out of bed or a chair, wetting or soiling oneself, or going hungry.
Use of Paid Long-Term Care
Because of their very low income, dual eligibles rely heavily on state-supported paid services. Among dual eligibles who need help with ADLs, more than one-half (54%) receive paid assistance (state-supported and other) from home care agencies or other sources. Still, slightly less than half (46%) of dual eligibles with long-term care needs do not receive paid care. Many rely on unpaid family members or friends, while others (4%) receive no help at all.
While paid care varies considerably among states, the survey indicates that greater use of paid home care lowers the likelihood of unmet needs, suggesting that state Medicaid policies promoting paid care may lead to more people getting the long-term care they need. Ultimately, though, say the authors, support for dual eligibles will require a change in federal policy—including increased spending and greater uniformity across states—to better meet these critical long-term care needs.
Facts and Figures:
- In a 1995 study of four states, 78 percent of Medicaid spending for elderly dual eligibles was for long-term care while 8 percent was for prescription drugs.
- Of the community-based dual eligibles who need assistance with ADLs, 28 percent said they frequently need more help, 24 percent occasionally need more help, and 5 percent seldom need more help.
- Among the six states in the study, Georgia has the lowest percentage of dual eligibles who need help with ADLs receiving paid assistance at home (31%) and the highest proportion with unmet need (65%).