For other Fund publications about health information technology (IT), visit our Health IT Resources page.
In the Literature
Most experts agree that electronic health records (EHRs) can improve the efficiency and quality of health care. But what about the costs and benefits associated with the technology, particularly for solo or small group practices, where more than two-thirds of U.S. physicians work? Commonwealth Fund-supported research by Robert Miller, Ph.D., and colleagues at the University of California, San Francisco, finds that for small group practices with EHRs, initial costs average $44,000 per physician (or nurse practitioner), with ongoing costs averaging $8,400 per physician per year.
While these expenses may seem steep, the researchers estimate that the average practice would cover its costs in under three years and, after that, profit considerably. Still, most physician offices spend more time at work initially. And some practices faced substantial financial risks, including long payback periods, billing problems, and data loss.
For the study, "The Value of Electronic Health Records in Solo or Small Group Practices," (Health Affairs, Sept./Oct. 2005) Miller and his team conducted 14 case studies of solo or small primary care practices that had used EHRs for one to three years. They interviewed EHR champions, observed providers' use of EHRs, and reviewed vendor contracts and practice reports from July 2004 through May 2005.
Financial Costs and Quality of Life
The study found that initial costs ranged from $37,056 to $63,600 per physician (or nurse practitioner). Disparities in expenses mostly reflected the varying levels of existing office hardware before EHR implementation and the technical and negotiating skills of the office champions. Average yearly costs of $8,400 per physician (or nurse practitioner) were mainly for software maintenance and support, hardware replacement, and payments to information systems staff and contractors.
In addition to some initial lost revenue, providers reported that they worked longer hours for an average of four months, as they entered data and became more familiar with the software. EHR champions had especially heavy time costs. But following the implementation period, some providers reported time savings and improved quality of life, and many liked accessing records from home.
Improved Billing, Efficiency Lead to Benefits
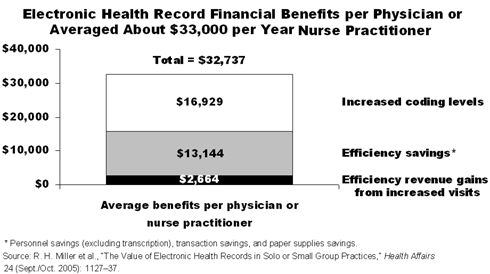
Despite the substantial startup costs, the average practice would pay for its initial and ongoing EHR costs within 2.5 years, the authors found. For the physician practices studied, the financial benefits averaged $33,000 per physician per year. These savings came from two main sources: increased coding levels that led to improved billing, and greater efficiency from a decrease in personnel costs. All practices reported some savings, ranging from $1,000 to $42,500 per physician (or nurse practitioner) per year.
On the other hand, a few practices would not fare as well. According to the study's estimates, one would take nine years to cover its costs, while two would never pay for their EHR systems, assuming no change in yearly benefits.
EHRs Not Extensively Used for Quality Improvement
Using EHRs provides physicians with some "automatic" quality benefits, the authors say, like improved data organization, accessibility, and legibility. Moreover, all the study practices engaged in at least some quality improvement (QI)–related EHR activities. However, only two extensively used EHR capabilities to systematically improve chronic and preventive care. Twelve practices reported using computerized reminders, but only five had practice-set reminders for patients with at least one type of chronic condition. Just four practices had created lists of patients who required needed services, like diabetics overdue for hemoglobin tests, and two practices generated reports on provider performance.
Policy Implications
To use EHRs for QI requires providers' time, ability, and willingness to make complementary process changes and to learn advanced EHR features. Lack of financial compensation for these tasks helps explains why extensive QI changes were limited.
Pay-for-performance policy initiatives that offer financial incentives and reward a wide array of clinical measures could help to increase QI gains, while particularly benefiting practices that use EHRs. At the same time, the authors suggest that policies promoting support services for practices, like technical and office redesign, could reduce providers' time and financial costs for QI-related EHR activities — particularly for those physicians with less technological or business savvy — while expanding the extent of their use.
Facts and Figures:
- Electronic health record software training and installation costs averaged $22,038 per physician (or nurse practitioner). Software alone accounted for about one-third of overall costs.
- Efficiency-related revenue gains from increased visits accounted for 8.1 percent of financial benefits, but only three practices reported them.
- Almost all providers used electronic health records for common tasks, including prescribing, viewing, within-practice messaging, and billing. Few practices used them for quality improvement, performance reporting, or patient–provider communication.