In the Literature
A new Commonwealth Fund–supported study finds that the structure of physician groups can influence the quality of patient care.
In "Do Integrated Medical Groups Provide Higher-Quality Medical Care than Individual Practice Associations?" (Annals of Internal Medicine, Dec. 5, 2006), researchers report that integrated medical group practices provided higher-quality care compared with individual practice associations (IPAs). The study—the first to evaluate the link between organizational structure of physician groups and quality of care—was conducted by Ateev Mehrotra, M.D., M.P.H, of RAND Health and the University of Pittsburgh School of Medicine, and Arnold M. Epstein, M.D., M.A., and Meredith B. Rosenthal, Ph.D., both of the Harvard School of Public Health.
Structure Makes a Difference
Organizational structure is an important characteristic of physician groups. At one end of the spectrum are integrated medical groups (IMGs)—centralized organizations which employ physicians in partnership arrangements, with facilities owned and managed by the group. In contrast, physicians in IPAs work under non-exclusive contracts and typically manage their own offices. Physician groups in the middle of the spectrum are termed "hybrids" by the researchers.
Using data from physician groups that contract with PacifiCare, a large health plan in California, the researchers examined three preventive measures (percentage of eligible patients who had mammography, Pap tests, and chlamydia screening) and three chronic disease management measures (percentage of diabetic patients receiving a retinal examination, asthma patients receiving controller medication, and patients receiving a beta blocker after acute myocardial infarction). They also asked the CEO or medical director of each group about organizational characteristics and use of quality-improvement strategies.
IMGs Score Higher Than IPAs on Four Quality-of-Care Measures
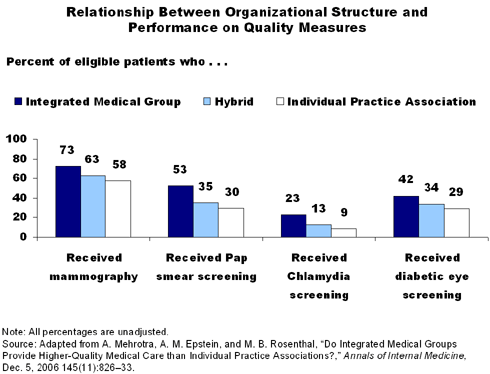
The researchers found patients in IMGs were more likely than those in IPAs to receive four of six services: mammography, Pap test, chlamydia screening, and diabetic eye screening. On these four measures, hybrid groups performed in the middle range between IMGs and IPAs. Even after adjusting the scores for factors including number of eligible patients, use of electronic medical records (EMRs), and proportion of board-certified physicians, IMGs had higher quality-of-care scores on the same four measures than IPAs, with hybrids in the middle. Nearly all physician groups performed well on two quality measures: use of beta blockers after a myocardial infarction and use of a controller medication for asthma.
Leaders of IMGs were more likely to report using EMRs than leaders of hybrids and IPAs (37% vs. 18% and 2%, respectively). They also reported using, on average, 7.2 out of a possible 11 quality-improvement strategies, compared with 5.3 in hybrids and 4.5 in IPAs. However, in all but one instance, neither the reported number of quality-improvement strategies overall, nor use of specific strategies, were associated with higher quality. The exception was an asthma feedback program, which was linked to higher use of asthma controller medications.
Shared Decision-Making and Collaboration May Contribute to High-Quality Care at IMGs
While other researchers have theorized that the way in which physician groups are organized can affect the quality of care, the Annals study is the first to demonstrate this relationship. The authors suggest that the use of centralized decision-making and close collaboration in IMGs may be a factor in their provision of higher-quality care.
Moreover, physician groups that cared for a larger volume of patients were more likely to deliver higher-quality care than lower-volume groups, perhaps because the former groups have greater resources to invest in improving care. These findings are of particular importance, say the authors, because most physicians in the United States work independently in small practices.
While substantial effort has been focused on encouraging physicians to use EMRs and quality-improvement strategies, this study demonstrates that organizational setting can also have a significant influence on the quality of care provided.
Facts and Figures
- All of the integrated medical groups (IMGs) surveyed reported collecting data on patient satisfaction, while less than half (47%) of the independent practice associations (IPAs) said that they solicited such data.
- Two of five (42%) eligible patients in IMG practices received diabetic eye screening, compared with 34 percent of eligible patients in hybrid practices and 29 percent in IPAs.
- More than half (53%) of eligible patients
in IMGs received a Pap test, compared with 35 percent in hybrid practices and 30 percent in IPAs.