In the Literature
Many studies have documented that minority patients receive lower-quality health care than non-minority patients at the same medical facilities. Relatively few, however, have attempted to explain the source of racial and ethnic disparities in care. Are observed disparities due to racial discrimination or bias? Do they result from a lack of cultural understanding on the part of health care providers? Or do minority patients receive care from lower-quality providers? According to a study supported by The Commonwealth Fund, disparities are largely the result of differences in where minority and non-minority patients seek health care.
In "Disparities in Health Care Are Driven by Where Minority Patients Seek Care" (Archives of Internal Medicine, June 25, 2007), a research team including Romana Hasnain-Wynia, Ph.D., of the Health Research and Educational Trust, Joel Weissman, Ph.D., of Harvard Medical School, and Fund senior program officer Anne Beal, M.D., M.P.H., examined quality-of-care data reported by U.S. hospitals participating in the Hospital Quality Alliance, a public–private collaboration formed to measure and publicly report on the quality of hospital care. The researchers found minority patients receive lower quality care, especially counseling services, and that lower-performing hospitals tend to serve a larger proportion of minority patients. "An underlying cause of disparities may be that minority patients are more likely to receive care in lower-performing hospitals," the authors write.
Who You Are, or Where You Seek Care?
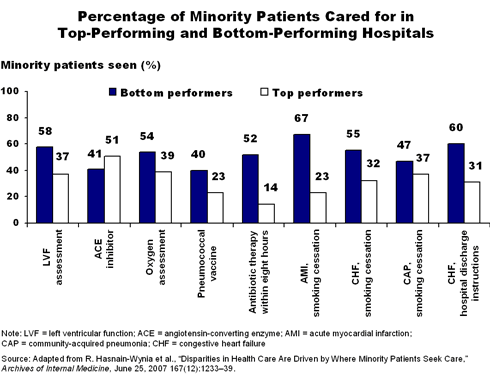
The study looked at the quality of care received by 320,970 patients age 18 and older at 123 teaching hospitals nationwide. Of these, 40 percent were minority patients. The Hospital Quality Alliance measures included recommended treatments (e.g., providing aspirin, beta blockers, or antibiotic therapy) for three clinical conditions: acute myocardial infarction, congestive heart failure, and community-acquired pneumonia, as well as patient counseling. The study divided the hospitals into top-performers and low-performers for 13 measures, then determined the percentage of minorities served by each.
The researchers found small but statistically significant disparities for 12 of 13 measures. After adjusting for site of care, the magnitudes of disparities decreased substantially—suggesting, say the authors, that minority patients are more likely to receive care in lower-performing hospitals.
The most pronounced disparities were for counseling services—discharge instructions or smoking cessation counseling—which require time, interaction with patients, and documentation. Noting that these disparities exist even within hospitals, the authors suggest that "communication training may improve the rates of the counseling measures for minority patients." Previous research suggests communication training benefits can be enhanced by considering patients' race, ethnicity, and culture.
The study also found that hospitals that performed less well on the measures tend to serve a higher percentage of minority patients. For example, on the indicator that measured smoking cessation counseling for acute myocardial infarction patients, only 20 percent of patients were minorities in the top-performing hospitals, compared with almost 70 percent of patients in the lower-performing hospitals.
Moving Forward
Low-performing hospitals may be "underresourced" in a number of ways, from a shortage of nurses to inadequate budgets and a lack of health information systems. "Yet these same hospitals may have providers who are hardworking and efficient, providing care with fewer resources to more disadvantaged patients," write the authors. They suggest future research is needed to determine which factors contribute to low performance in hospitals and how performance may be related to disparities in care. "Policy recommendations may need to focus on pay-for-improvement metrics for those underresourced providers caring for the most disadvantaged populations," the authors write, concluding that programs and polices to reduce and potentially eliminate disparities should be informed by research that identifies and targets the underlying causes of lower performance in hospitals.