In the Literature
Do hospitals that make improvements to their patient safety practices provide better care and achieve better outcomes for their patients? That is the question addressed by a Commonwealth Fund-supported study conducted by Ashish K. Jha, M.D., of the Harvard School of Public Health, who examined hospitals targeted by the Leapfrog Group, a coalition of 65 employers and agencies that purchase health care for approximately 34 million Americans. The organization has garnered considerable attention in recent years for its efforts to encourage hospitals to adopt evidence-based practices to improve patient safety.In the article, Does the Leapfrog Program Help Identify High-Quality Hospitals? (The Joint Commission Journal on Quality and Patient Safety, June 2008), Jha and colleagues found that hospitals that implemented patient safety practices endorsed by the Leapfrog Group reported better quality of care and lower mortality rates. These results demonstrate that "hospitals can clearly improve quality and safety together without need for a trade-off," the authors say.
Examining the Data
Jha and his team began their study with data from the April 2006 Leapfrog Group survey of 1,860 hospitals in 29 regions, focusing on three patient safety practices: implementing computerized physician order entry (CPOE) systems, which communicates physicians' orders over a computer network to decrease delays and reduce errors; staffing intensive care units (ICUs) with intensivists (physicians specially trained in critical care); and relying on evidence in making referrals and treatment decisions—for example, using commonly accepted treatment guidelines, measuring outcomes, and offering high-risk surgical procedures (like coronary artery bypass graft surgery) only when the hospital meets a minimum threshold for patient volume.
The researchers combined these data with the Hospital Quality Alliance's quality performance scores for management of acute myocardial infarction (AMI), congestive heart failure (CHF), and pneumonia. In addition, they gathered information on hospital characteristics and patient demographics from the American Hospital Association's annual survey and the 2003 MedPAR survey of Medicare beneficiaries.
Of the 1,860 hospitals targeted by Leapfrog, 790 chose not to disclose their patient safety practices. The 682 hospitals that had begun to implement at least one Leapfrog patient safety practice tended to be larger, private not-for-profit, or teaching hospitals located in urban areas, compared with hospitals that did not report or had not implemented any of the practices.
Patient Safety and Quality Care
Hospitals that had begun to implement CPOE had higher performance on AMI and CHF measures than those that chose not to report. The differences were much smaller in pneumonia care. The authors found a very similar pattern for the other patient safety initiatives: Hospitals with ICUs staffed with intensivists or those that used evidence-based referrals generally had better care for AMI and CHF.
Lower Mortality Rates
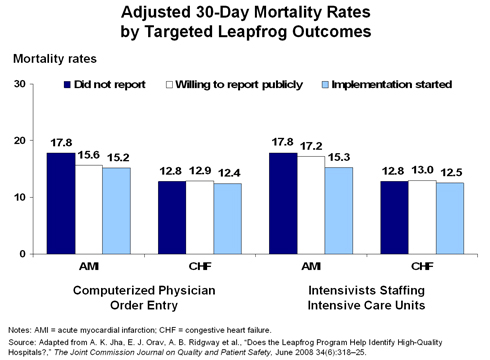
The hospitals that used these patient safety practices had lower risk-adjusted mortality rates for patients admitted with AMI or pneumonia. Patients admitted for an AMI to hospitals that had begun CPOE implementation were less likely to die within 30 days, compared with patients admitted to hospitals without CPOE or to nonreporting hospitals, the authors said. These hospitals also had lower mortality rates for patients admitted with pneumonia. Mortality rates for CHF, however, were not significantly different. The researchers discovered similar patterns when they examined hospitals that staffed ICUs with intensivists and those that used evidence-based referrals.
The authors conclude that these findings suggest hospitals do not have to choose between improving quality and safety. Further, they help reinforce the validity of the Leapfrog patient safety measures, noting that "if consumers use the Leapfrog rating system, not only will they likely choose hospitals with better patient safety practices—but also with modestly better process quality and lower mortality."
Facts and Figures
- The Leapfrog Group was founded in 2000 and includes more than 65 employers and agencies that purchase care for more than 34 million people.
- Leapfrog makes its patient safety data publicly available on www.leapfroggroup.org.
- Of the 1,860 hospitals targeted by Leapfrog, 790 chose not to disclose their patient safety activities, and 1,070 were willing to report their activities publicly.