Synopsis
This cross-sectional study of urban hospitals in Texas found that those with automated clinical information systems had fewer complications, lower mortality rates, and lower costs.
The Issue
Health information technology is a viable solution to improve health care quality, enhance communication, and reduce costs and waste in the system. Research has shown such benefits, but few studies have examined multiple hospitals to gauge the effect of clinical information systems in inpatient settings. Focusing on a diverse group of Texas hospitals, this study examined the association between a hospital's use of automation—specifically notes and records, test results, order entry, and decision support—and inpatient mortality, complications, costs, and length of stay for four medical conditions.
Key Findings
- Among the four clinical conditions studied—myocardial infarction, congestive heart failure, coronary artery bypass grafting, and pneumonia—higher technology scores were generally associated with decreased adjusted odds ratios for fatal hospitalizations.
- Among all hospitalizations, a 10-point increase in automation of notes and records was associated with a 15 percent decrease in the adjusted odds of hospital death.
- Hospitals with more advanced order entry capability experienced decreases of 9 percent and 55 percent, respectively, in the adjusted odds of death for myocardial infarction and coronary artery bypass graft procedures.
- Facilities with higher scores in decision support were associated with a 16 percent decrease in the adjusted odds of complications for all causes of hospitalizations.
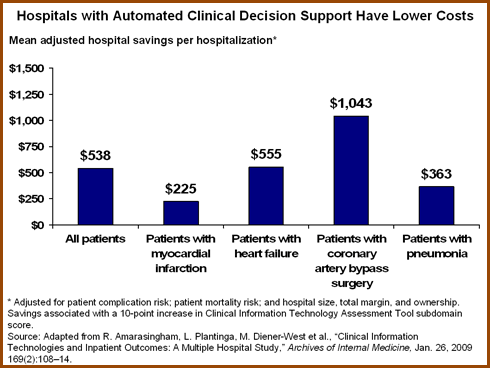
- For nearly all clinical conditions, higher scores on automated test results, order entry, and decision support were overwhelmingly associated with lower hospital costs.
Addressing the Problem

The authors warn that insufficient user training, difficult-to-use technology, or misaligned physician and organizational routines may prevent hospitals from fully realizing the benefits of health information technology despite expensive investments in IT. The assessment tool described and used by the authors goes beyond a simple measurement of technology, but also reflects the harmony between the technology, people, and processes of an organization by examining how physicians interact with an information system on a daily basis. If such systems are properly designed around clinical workflows, they can reduce mortality, complications, and costs, the authors conclude.
About the Study
The researchers conducted a cross-sectional study of 41 urban Texas hospitals using the Clinical Information Technology Assessment Tool, which measures a hospital's level of automation based on physician interactions with the information systems. Adjusting for potential confounders, the team examined whether greater hospital automation of information was associated with reduced rates of impatient mortality, complications, costs, and length of stay for 167,233 patients older than 50 years at responding hospitals between December 1, 2005, and May 30, 2006.
The Bottom Line
Hospitals with automated notes and records, test results, order entry, and clinical decision support experience fewer complications, lower mortality rates, and lower costs.


