The Health Affairs article is available at: http://content.healthaffairs.org/cgi/content/abstract/hlthaff.28.4.w533
Synopsis
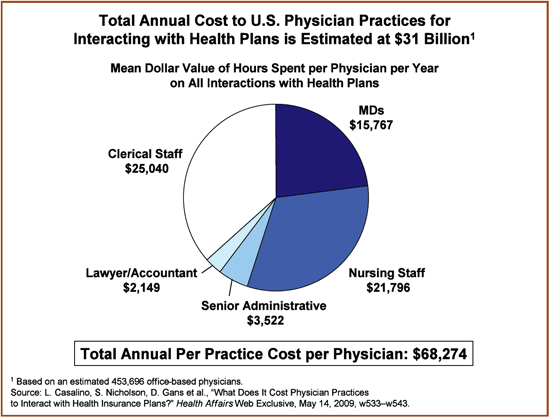
A national study of nearly 900 U.S. physicians and medical group administrators found that physicians spent on average 142 hours annually interacting with health plans, at an estimated annual cost to physician practices of $31 billion, or $68,274 on average per physician, per year.
The Issue
Administrative costs are high in health care. While those incurred by physician offices are a contributor to overall administrative costs, very little information has been available regarding the costs physician practices incur when they interact with health insurance plans. The authors surveyed a national sample of physicians and medical group administrators to ascertain how much time physician practices spent interacting with health plans on prior-authorization requirements, pharmaceutical formularies, claims, credentialing, contracting, and quality data. The study examines in depth the extent of such interactions, generating both time and dollar value estimates for such administration.
Key Findings
- Physicians, on average, spent nearly three weeks per year interacting with health plans, or 3.0 hours per week. Primary care physicians spent significantly more time (3.5 hours per week) than medical specialists (2.6 hours) or surgical specialists (2.1 hours).
- Nursing staff spent an additional 23 weeks per year per physician interacting with health plans, while clerical staff spent 44 weeks.
- Compared with other interactions, physicians, on average, spent more time dealing with formularies (1.7 hours per week for primary care doctors, for example), and the least on submitting or reviewing health plan quality data (0.04 hours per week for all physicians).
- Converted into dollars, practices spent an average of $68,274 per physician per year interacting with health plans; primary care practices spent $64,859 annually per physician, nearly one-third of the income, plus benefits, of the typical primary care physician. This results in an estimated $31 billion per year spent by physician practices on interactions with health plans.
Addressing the Problem
 The estimated $31 billion in costs physician practices incur in their interactions with health plans comprises 6.9 percent of all U.S. expenditures for physicians and clinical services. While administrative costs are often portrayed as waste, the authors note that such interactions may produce benefits, too. Prior authorization and formulary requirements, for example, may reduce health care costs and increase the quality of care. The authors suggest that researchers explore the benefits these high costs bring, as well as the possible policy and administrative procedure changes that would make physician–plan interactions more efficient. This could include, for example, centralizing the credentialing of physicians.
The estimated $31 billion in costs physician practices incur in their interactions with health plans comprises 6.9 percent of all U.S. expenditures for physicians and clinical services. While administrative costs are often portrayed as waste, the authors note that such interactions may produce benefits, too. Prior authorization and formulary requirements, for example, may reduce health care costs and increase the quality of care. The authors suggest that researchers explore the benefits these high costs bring, as well as the possible policy and administrative procedure changes that would make physician–plan interactions more efficient. This could include, for example, centralizing the credentialing of physicians.
About the Study
The authors randomly selected 1,310 private practice physicians working in solo or two-physician practices and those working in practices with three or more doctors. Physicians employed by academic medical centers, health maintenance organizations (HMOs), those with a large number of self-pay patients, and certain others were excluded from survey. Administrators from 629 medical groups were also surveyed. The survey was conducted in the second half of 2006 and had an adjusted overall response rate of 57.5 percent.
The Bottom Line
Although health plans claim to have reduced the administrative burden they place on physicians, evidence shows that the average physician spends nearly three weeks a year interacting with plans, at an estimated annual cost to practices of $31 billion. Primary care physicians, especially those in small practices, spend larger amounts of time interacting with plans than those in other specialties.