Synopsis
The U.S. system of billing for health care is complex, expensive, and inefficient. Excessive administrative complexity costs physicians nearly 12 percent of their net patient service revenue, according to a Commonwealth Fund–supported study. Streamlining administrative processes associated with the billing and payment of medical providers could save $7 billion annually, and save four hours per week of physicians' time and five hours of support staff time.
The Issue
 The administrative costs involved in paying health care providers are a well-known contributor to rising health care costs overall. In most cases, a third party—a health plan or insurance company—handles the payment transaction between the provider and patient. This system requires certain administrative controls or processes to ensure financial security, yet there is evidence that the complexity exceeds what is necessary to comply with the rules and ensure accurate and timely payment. Such excessive complexity adds costs and additional work hours for physicians and their staff, without adding any benefit. In this study, researchers analyzed the administrative costs of a large multidisciplinary physician organization that works with multiple payers, each with different requirements and rules. After identifying all the functions identified with billing, processing, and payment, they then devised a new, streamlined model to determine the burden of excessive administrative complexity.
The administrative costs involved in paying health care providers are a well-known contributor to rising health care costs overall. In most cases, a third party—a health plan or insurance company—handles the payment transaction between the provider and patient. This system requires certain administrative controls or processes to ensure financial security, yet there is evidence that the complexity exceeds what is necessary to comply with the rules and ensure accurate and timely payment. Such excessive complexity adds costs and additional work hours for physicians and their staff, without adding any benefit. In this study, researchers analyzed the administrative costs of a large multidisciplinary physician organization that works with multiple payers, each with different requirements and rules. After identifying all the functions identified with billing, processing, and payment, they then devised a new, streamlined model to determine the burden of excessive administrative complexity.
Key Findings
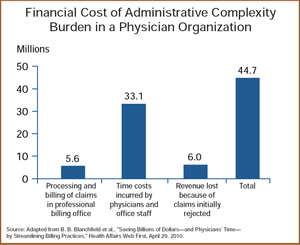
- For the organization studied, the cost of excessive administrative complexity, including both expenses (i.e., the labor costs) and lost revenue (i.e., revenue lost when claims are inappropriately rejected, delayed, and reprocessed or when the reimbursement rate is lowered) was nearly $45 million in 2006, or 12 percent of net patient revenue.
- The largest portion of the administrative complexity burden, 74 percent, was attributed to time spent by physicians and their office staff in preparing paperwork and contacting payers about prescriptions, diagnoses, treatment plans, and referrals.
- About 12.5 percent of the total burden, or $5.6 million, was directly associated with the processing and billing of claims in the professional billing office.
- On a national scale, adopting streamlined administrative rules would translate into $7 billion of savings annually. It would also save four hours of physician time and five hours of support staff time per week.
Addressing the Problem
 While some administrative tasks will always be necessary to process claims for payment, among other tasks, the U.S. health care system is plagued by "byzantine systems of rules and regulations." The result is a costly and growing bureaucracy that takes resources away from patient care. The authors recommend streamlining administrative services by developing a single, transparent set of payment rules for multiple payers, a single claim form, and standard rules of submission. They point out that these innovations would not necessarily decrease the diversity of insurance product offerings or adversely affect choice.
While some administrative tasks will always be necessary to process claims for payment, among other tasks, the U.S. health care system is plagued by "byzantine systems of rules and regulations." The result is a costly and growing bureaucracy that takes resources away from patient care. The authors recommend streamlining administrative services by developing a single, transparent set of payment rules for multiple payers, a single claim form, and standard rules of submission. They point out that these innovations would not necessarily decrease the diversity of insurance product offerings or adversely affect choice.
About This Study
The authors analyzed the administrative workload at a physicians' organization affiliated with a large, urban, academic teaching hospital. The organization works with multiple payers, all with different payment requirements. First, the authors identified administrative functions, staffing, and associated costs related to the billing, processing, and payment of claims in 2006. Then, using a model that was stripped of the excessive complexity, they estimated the costs of processing the same claims.
Bottom Line
Streamlining administrative costs associated with the billing and payment of medical providers could save $7 billion annually, and save four hours per week of physicians' time and five hours of support staff time.


