Synopsis
In studying the use of six best practices for providing care to the chronically ill, researchers found that fewer than half of the evidence-based care management processes were used by large physician organizations in the United States. Higher use was correlated with participation in quality improvement programs, having a patient-centered focus, and ownership by a hospital or health maintenance organization, among other factors.
 The Issue
The Issue
A key to improving the quality of health care while reducing costs is reforming the way care is delivered to the more than 90 million Americans with chronic illnesses. Seventy-five percent of the $1.4 trillion spent on health care in the U.S. is for treatment of the chronically ill. Studies have found that use of evidence-based care management processes (CMPs), such as compiling lists or electronic registries of patients, providing physicians with feedback on quality of care, sending reminders to physicians for recommended care and to patients for preventive or follow-up care, and giving patients access to educators to help them manage their illness, can improve care and reduce costs. For this study, researchers sought to measure the prevalence of CMP use among large physician organizations.
Key Findings
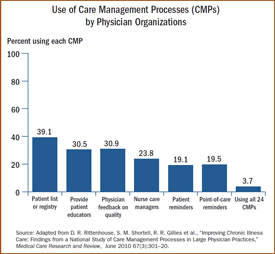
- The organizations used, on average, 46 percent of the six CMPs studied, with the most prevalent being patient lists or electronic registries (39.1%), feedback to physicians on care quality (30.9%), and use of patient educators (30.5%). CMP use was highest for diabetes and lowest for depression.
- Organizational characteristics, such as a focus on patient-centered care, participation in quality improvement demonstration programs, and ownership by a hospital or health maintenance organization (HMO), were correlated with increased CMP use.
- Of the organizations studied, very large medical groups (more than 440 members) had a higher CMP usage than smaller groups, as did independent practice associations (IPAs) of any size.
- Other factors positively associated with CMP use by physician organizations included a high prevalence of CMP use by health plans, evaluation by health plans on patient satisfaction, and capitated payment for hospital expenses.
Addressing the Problem
 The study found that large physician organizations have been slow to adopt practices that improve quality and reduce the cost of care for the chronically ill. Purchasers, insurers, and policymakers need to devise strategies, including financial and other incentives, to leverage the external factors that encourage CMP use. Physician–leaders, meanwhile, "play the central role in developing the organizational structures and cultures capable of translating those incentives into improved care for their patients," say the authors.
The study found that large physician organizations have been slow to adopt practices that improve quality and reduce the cost of care for the chronically ill. Purchasers, insurers, and policymakers need to devise strategies, including financial and other incentives, to leverage the external factors that encourage CMP use. Physician–leaders, meanwhile, "play the central role in developing the organizational structures and cultures capable of translating those incentives into improved care for their patients," say the authors.
About the Study
The researchers surveyed all large physician organizations in the U.S.—both medical groups and IPAs—about their use of six CMPs in 2006–07, achieving a response rate of 60.3 percent (538 of an estimated 892 eligible organizations). They focused on diabetes, asthma, congestive heart failure and depression, all of which have high incidences and associated care costs. The authors also looked at the effect of external influences and internal characteristics on the organizations' use of CMPs. The study was supported by The Commonwealth Fund, the Robert Wood Johnson Foundation, and the California HealthCare Foundation.
The Bottom Line
Practices that improve quality of care and decrease costs for chronically ill individuals have not been implemented fully by large physician organizations. External incentives and internal reforms need to be employed strategically to spur their adoption.


