Synopsis
Employers are increasingly looking to wellness programs to encourage healthy behaviors among their employees and control health care spending. A study examining the effects of a wellness program on workers’ health service use found a substantial decrease in hospitalizations for targeted conditions, but the resulting cost-savings were counterbalanced by increased spending for prescription drugs and outpatient care, in addition to the costs of the program and incentives themselves.
The Issue
Many employers offer voluntary wellness programs to encourage employees to undergo health screenings, join fitness centers, quit smoking, or pursue other health goals. It is widely believed that such programs improve health and control spending, but experience thus far has shown that employers need to offer strong financial incentives to encourage participation. The Affordable Care Act raises the amount by which employers may vary employees’ premium contributions to encourage wellness program take-up. In this Commonwealth Fund–supported study, researchers examine the effects of one such program begun in 2005 for employees and dependents of a hospital system in St. Louis, Mo. As an incentive to join, the hospital system limited enrollment in its most generous health plan to program participants. Participants had to complete a health risk assessment, sign a pledge promising to maintain a healthy diet and exercise regularly, report their smoking status, and enroll in a smoking cessation program if a smoker. The hospital also held health fairs for all employees.
Key Findings
- Participation in the wellness program was strong―82 percent of employees joined―as was attendance at the health fairs.
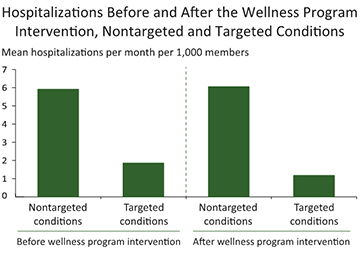
- Rates of hospitalization with at least one of the six conditions targeted by the program (diabetes, hypertensive heart disease, ischemic heart disease, cerebrovascular disease, acute pulmonary infections, and chronic obstructive pulmonary disease) declined 41 percent relative to the comparison group. There were no significant changes in hospitalizations for nontargeted conditions.
- The intervention was associated with a 1.9 percent increase in overall medication days (particularly for antihypertensive and cholesterol-lowering drugs). The number of new outpatient visits for targeted conditions also rose significantly among the intervention group, but not for the comparison group.
- Inpatient health claims among hospital system beneficiaries dropped $22 a month, but this was counterbalanced by an increase of $19 in non-inpatient claims costs. When considering these costs combined with the total wellness program costs—which were slightly over $500,000 for each year—it is unlikely that the program saved money.
Addressing the Problem
Employees appeared to be motivated by the financial incentive to participate in the wellness program and the “culture of health” promoted by their institution. Reduced hospitalizations may have resulted from earlier detection and treatment, better self-management of conditions, smoking cessation, or healthier lifestyles. Further analyses of wellness programs are needed to evaluate their effects on health spending over the long term.
About the Study
Researchers compared health service use among hospital system beneficiaries for one year before and two years after the introduction of the wellness program with a comparison group of employees at two other large St. Louis employers that did not offer wellness incentives. The analysis controlled for baseline health characteristics as well as for age, sex, and other demographics.
The Bottom Line
Employer wellness programs have the potential to improve employees’ health and productivity, but they are unlikely to substantially reduce employers’ health care spending in the short term.


