
Synopsis
A study seeking to explain the variation in how patients rate their experiences with primary care providers concluded that individual physicians themselves account for the largest share of this variation, particularly in terms of the quality of their communication with patients and their support for health promotion. Other major contributing factors are the practice sites (e.g., how patient care is organized) and local primary care markets (e.g., physician supply).
The Issue
Programs used to evaluate individual physicians and guide quality improvement efforts increasingly rely on patient experience data. Because it would be unfair to assess and reward individual physicians based on factors that are beyond their control, it is important to identify all possible sources of variation in physician performance in order to target performance improvement activities. This study assessed the relative contribution of individual physicians, practice sites, medical groups, and primary care service areas to differences in patient experience.
Key Findings
- Compared with the other factors studied, individual physicians accounted for a higher share of the variation in patients' reports related to the quality of physician–patient interactions (communication, health promotion support) and to patients' global ratings of individual physicians (willingness to recommend physician and overall rating). The share of variation attributed to physicians on these measures ranged from 45 percent to 49 percent.
-
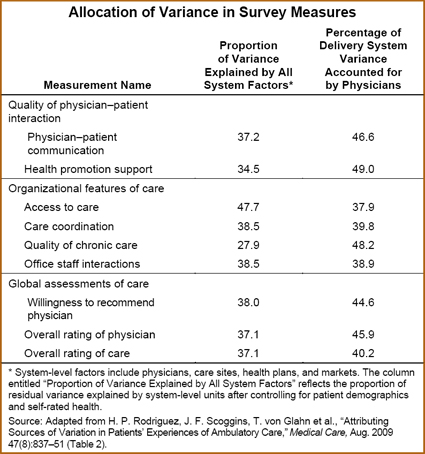 Care sites accounted for a substantial proportion of the performance variation regarding access to care (29%), care coordination (26%), and interactions with office staff (32%).
Care sites accounted for a substantial proportion of the performance variation regarding access to care (29%), care coordination (26%), and interactions with office staff (32%). - The patient experience measures for which medical groups had the greatest influence were health promotion (21%) and global assessments of care, including overall rating of the physician (21%), and overall rating of care received by all clinicians (24%).
- Primary care markets accounted for the largest proportion of variance with respect to measures of access to care (20%), care coordination (21%), and quality of chronic care (25%).
Addressing the Problem
Knowing the relative contribution of sources of variation in ambulatory care experience can inform efforts to target interventions designed to improve patient care. This study showed that the lion's share of variation can be explained by the "lowest system-level units assessed," that is, care sites and individual physicians. Thus, care delivery redesign efforts that aim to improve, for example, access to appointments and care coordination — functions that are typically the responsibilities of the doctor's office — would likely be effective in improving patient experiences. The authors also recommend additional research into which specific market factors — such as the quality of insurance coverage or the supply of primary care physicians — impede performance.
About the Study
The researchers drew on Ambulatory Care Experiences Survey (ACES) data (2007) from 61,839 commercially insured patients of 1,729 primary care physicians belonging to 39 medical groups in California. Their goal was to determine the proportion of explainable performance variation attributable to various organizational units in composite measures of physician–patient interaction, organizational features of care, and global assessments of care.
The Bottom Line
Individual physicians and their care sites should be the primary focus of efforts to improve patients' care experiences. Further research is needed to determine whether organizational features of patient care that are affected by health care markets can also be improved.


