By Sarah Klein
Issue: The business improvement techniques known as Six Sigma and Lean manufacturing have been used to identify and reduce defects in production methods for more than two decades. Though commonly used in the automobile and manufacturing industries to reduce costs and increase profits and efficiency, they have only recently been used to identify and reduce variance in care processes within physician offices. Part of the reason is that medical professionals tend to believe that the complexity of health care routines defies the type of categorization necessary to eliminate process variation—and thus, waste. But, with the help of consultants, a large ophthalmology practice proved it could be done.
Organization and Leadership: Lansing Ophthalmology has 14 physicians and seven optometrists, and a staff of 144 employees who provide clinical and administrative support. The practice has a base of 100,000 patients, of whom 75,000 are seen annually. Nearly 80 percent of patients visit the East Lansing office, a 35,000-square-foot facility where clinicians conduct eye exams, perform surgery, and dispense eyewear. The remaining patients are examined in six satellite offices within a 67-mile radius.
Charles Dobis, CMPE, has been executive director of the practice for more than 20 years. Teresa Prior, R.N., who has been the practice's clinical director for almost eight years, oversaw the project. The practice relied on the consulting advice of David Lalain, director of life sciences for the Automotive Action Industry Group (AIAG), a Southfield, Mich.–based member organization that applies quality and process improvement techniques to auto industry suppliers, including those in the health care sector, and David Watkins, executive vice president and director of international operations for OMNEX Inc., an Ann Arbor, Mich.–based training, software, and consulting company, who has advised manufacturing, advertising, and shipping companies about process improvement.
Target Population: The practice's process improvement was focused on its main office in East Lansing, which handles roughly 63,000 patient visits annually. The practice sees patients of all ages, nearly 40 percent of whom are age 65 or older and, as such, covered by Medicare.
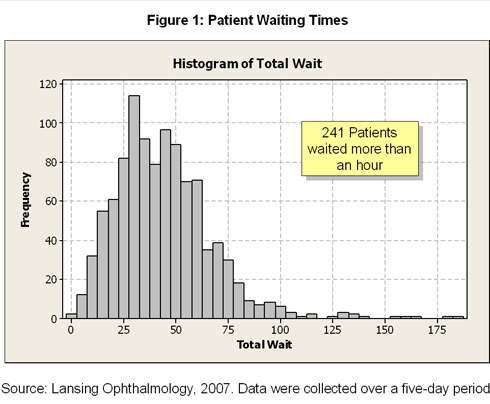
Process of Change: In early 2007, Lansing Ophthalmology volunteered to take part in a pilot project sponsored by AIAG, which aimed to demonstrate the value of applying Lean Production and Six Sigma techniques to the health care industry. The administrative leaders at Lansing hoped to use the methodology to streamline the flow of patients through its main clinic. At the time, patients were waiting as long as 90 minutes to see a doctor; they tended to bunch outside the physicians' offices, putting additional pressure on doctors (Figure 1).
The group had tried without success to find its own solution to the problem. "People would try to schedule their way out of it. That never worked," Dobis says. For example, doctors had tried to schedule their more difficult cases in the afternoon and the simpler ones in the practice's early hours. But that strategy only overwhelmed the technicians, who were faced with handling the most difficult cases all at once. "It might have worked if [the doctors] were in a solo practice or worked with one other person. But they were a spoke within a wheel," Prior says.
Drawing on Six Sigma methods, the consultants recommended collecting patient flow data for a period of seven business days, measuring how long it took patients to advance through every step of the process. Clinic staff kept a separate time sheet for each person, noting how long it took to register the patient, gather a history, perform a refraction, and provide other services. The chart also captured how long patients waited between these care processes.
Before project leaders began gathering data, they held meetings to gain the cooperation and support of the practice's physicians and staff. "That was the most difficult part," Dobis says. Although the clinicians and staff agreed patient flow was a problem, they were reluctant to change the existing system, which allowed physicians great latitude in how they prioritized patients and managed their time. "No one wanted to give up control of his or her own schedule," he says. It wasn't strictly self-interest. There was also a prevailing sense that wait times might increase. "They thought things might get worse; that instead of seeing improvement, things might degenerate further," Dobis says.
Such resistance to change is common among professionals such as lawyers, engineers, and doctors, Watkins says. "They say, 'There is no such thing as a process. What we do is an art form.'" That was the case at Lansing as well. "They were adamant there were no processes," Lalain says.
The data would show otherwise, but until they could collect it, Dobis and Prior had to convince the physicians and staff they needed outside help. The two stressed that the patient flow problem was a longstanding one, which the practice had not previously been able to solve. In essence, Prior argued: "Now we have experts. We have to try it."
The staff had other concerns. Because so many of their activities were being measured and timed, they were concerned that the data would be used to reward high performers and punish low performers. To address those concerns, the project leaders emphasized that the overall goal was to improve efficiency and not to target individual employees. "We did that repeatedly," Prior says.
The staff collected data on 1,227 patients, using the previously described time sheet, which was attached to each patient chart during the data collection period. The time required for each exam was entered into an Excel spreadsheet and analyzed by the consultants. The data showed that 241 patients—or 19.6 percent of those measured—had spent more than one hour waiting during their visit. The data also showed that, while there were some 149 exam combinations required by patients, nearly 50 percent followed one of five set patterns. The 242 patients who came for a history, a refraction, dilation, and an exam with the doctor spent an average of 79 minutes in the office, of which 45 minutes was spent waiting (Figure 2).
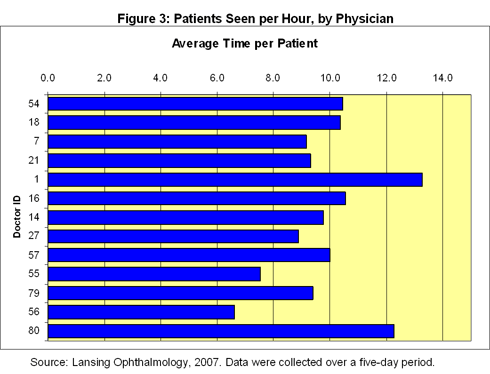
The consultants found great variability in the time taken to perform various procedures. The number of patients seen by doctors per hour ranged from less than two to nearly six (Figure 3). The practice made a decision not to try to alter that variation at the outset. In some cases, there were good reasons for the variability: some physicians were performing more complex procedures or seeing long-term patients who required more face time with doctors. "Eventually they are going to get pulled into the process," Lalain says. But not at first. "Once they are sold on eliminating variation with technicians and everything else, then they might swallow the pill that says they are part of the problem," Lalain says.
Among the technicians, there was also great variability in the time taken to gather histories from patients and perform refractions. Histories took from five to 16 minutes, while EPIC exams (a refraction to measure the degree of a patient's nearsightedness or farsightedness, if any) took from five to 21 minutes, depending on the technician. That variation made it difficult to present a patient to the doctor at the appropriate time.
Another problem revealed by the data was the variation in patient arrival times. Some were as much as an hour early and others were up to 45 minutes late. Because the clinic had a policy of seeing patients when they arrived, patients were inadvertently encouraged to game the schedule, which had tremendous downstream consequences for staff trying to predict the flow of patients and manage their care appropriately.
The data also confirmed what physicians had complained about: patients were bunching outside doctors' offices in large numbers. The problem, consultants pointed out, was caused by the fact that patients were being moved through the system without any recognition for the pace at which doctors were seeing those patients.
To reduce variation in the patient-flow process, the practice:
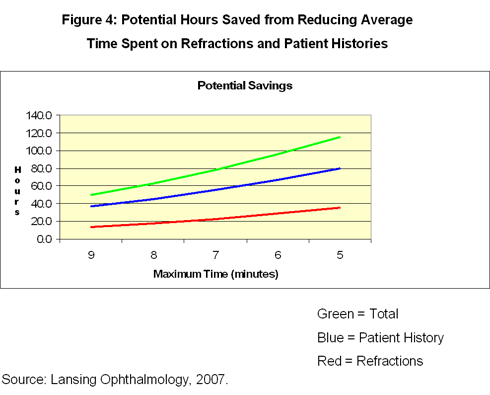
Technician time: The goal is 10 minutes for each exam (the previous range was five to 21 minutes). "Everyone is hitting it except for some new people," says Prior. The consultants determined that if the clinic could train the technicians to complete both the history and the refraction in eight minutes each, they could save the equivalent of one and one-half staff positions per year (Figure 4). Prior says that, because the clinic is growing, it would not lay off staff but would use any extra staff to meet the needs of new physicians.
Wait times: "We met the benchmark for a complete eye exam, which is one hour and 16 minutes," says Prior. The average prior to implementation was three minutes more. The clinic expects to see greater time savings when it fully implements the new scheduling system.
Bunching: Doctors only see one or two patients waiting for their visit at any given time. That doesn't mean more patients aren't waiting, as there can still be clusters of patients after 11 am or 4 pm. In those cases, the clinic managers or patient coordinator tries to assign patients to different doctors to smooth out the flow. The goal is to pull patients through the system at the pace at which doctors can see them, rather than push them through without regard for such timing.
Implications: There are some general lessons to learn from the Lansing practice's use of these manufacturing techniques, as outlined below.
Financing: The consultants' services were provided to the clinic at no cost through the AIAG pilot project and, while Prior devoted up to a year on the project, spending anywhere from 10 to 20 hours per week on the improvements, she did this in addition to her regular job. Thus, the practice spent no money for the project. The consultants' fee would have amounted to $20,000, says Lalain. Would the practice have been willing to pay for these services? Only if there was a track record proving that the procedure would be financially worthwhile, answers Dobis. "The issue also is that the process has to have some efficiency in the minds of the doctors, because ultimately they are the ones who are paying for it. They have to be convinced there would be value. I think long term, yes. But the track record has to be (established)," he says.
Having learned process improvement techniques, Prior says the group could apply it to another problem—provided it could find staff with the time to do it. "We would have to take a simple project with a simple goal," she says.
As for savings, the changes allowed the clinic to add slightly fewer support staff when it hired two additional doctors for the practice this year. The ratio of staff to doctors in the main office dropped to 3.1 to 1 from 3.3 to 1.
Applicability to other practices: It's easier to implement such programs in specialties that compete for patients, such as ophthalmology and plastic surgery, as well as practices where the provided services are more routine. It's not impossible to make the same improvements in a primary care practice, says Watkins. "Even in an apparently unpredictable system, there's predictability," he says.
Because of employee resistance to change, it's important to have a highly motivated person shepherding the project. This leader also needs reinforcement. When Prior was frustrated, for example, she could turn to one of the consultants, who would remind her that the things she was experiencing were typical.
For Further Information: Contact David Lalain, director of life sciences for the Automotive Industry Action Group, [email protected], or Teresa Prior, clinical director, Lansing Ophthalmology, [email protected].
Issue: The business improvement techniques known as Six Sigma and Lean manufacturing have been used to identify and reduce defects in production methods for more than two decades. Though commonly used in the automobile and manufacturing industries to reduce costs and increase profits and efficiency, they have only recently been used to identify and reduce variance in care processes within physician offices. Part of the reason is that medical professionals tend to believe that the complexity of health care routines defies the type of categorization necessary to eliminate process variation—and thus, waste. But, with the help of consultants, a large ophthalmology practice proved it could be done.
Organization and Leadership: Lansing Ophthalmology has 14 physicians and seven optometrists, and a staff of 144 employees who provide clinical and administrative support. The practice has a base of 100,000 patients, of whom 75,000 are seen annually. Nearly 80 percent of patients visit the East Lansing office, a 35,000-square-foot facility where clinicians conduct eye exams, perform surgery, and dispense eyewear. The remaining patients are examined in six satellite offices within a 67-mile radius.
Charles Dobis, CMPE, has been executive director of the practice for more than 20 years. Teresa Prior, R.N., who has been the practice's clinical director for almost eight years, oversaw the project. The practice relied on the consulting advice of David Lalain, director of life sciences for the Automotive Action Industry Group (AIAG), a Southfield, Mich.–based member organization that applies quality and process improvement techniques to auto industry suppliers, including those in the health care sector, and David Watkins, executive vice president and director of international operations for OMNEX Inc., an Ann Arbor, Mich.–based training, software, and consulting company, who has advised manufacturing, advertising, and shipping companies about process improvement.
Target Population: The practice's process improvement was focused on its main office in East Lansing, which handles roughly 63,000 patient visits annually. The practice sees patients of all ages, nearly 40 percent of whom are age 65 or older and, as such, covered by Medicare.
Process of Change: In early 2007, Lansing Ophthalmology volunteered to take part in a pilot project sponsored by AIAG, which aimed to demonstrate the value of applying Lean Production and Six Sigma techniques to the health care industry. The administrative leaders at Lansing hoped to use the methodology to streamline the flow of patients through its main clinic. At the time, patients were waiting as long as 90 minutes to see a doctor; they tended to bunch outside the physicians' offices, putting additional pressure on doctors (Figure 1).

The group had tried without success to find its own solution to the problem. "People would try to schedule their way out of it. That never worked," Dobis says. For example, doctors had tried to schedule their more difficult cases in the afternoon and the simpler ones in the practice's early hours. But that strategy only overwhelmed the technicians, who were faced with handling the most difficult cases all at once. "It might have worked if [the doctors] were in a solo practice or worked with one other person. But they were a spoke within a wheel," Prior says.
Drawing on Six Sigma methods, the consultants recommended collecting patient flow data for a period of seven business days, measuring how long it took patients to advance through every step of the process. Clinic staff kept a separate time sheet for each person, noting how long it took to register the patient, gather a history, perform a refraction, and provide other services. The chart also captured how long patients waited between these care processes.
Before project leaders began gathering data, they held meetings to gain the cooperation and support of the practice's physicians and staff. "That was the most difficult part," Dobis says. Although the clinicians and staff agreed patient flow was a problem, they were reluctant to change the existing system, which allowed physicians great latitude in how they prioritized patients and managed their time. "No one wanted to give up control of his or her own schedule," he says. It wasn't strictly self-interest. There was also a prevailing sense that wait times might increase. "They thought things might get worse; that instead of seeing improvement, things might degenerate further," Dobis says.
Such resistance to change is common among professionals such as lawyers, engineers, and doctors, Watkins says. "They say, 'There is no such thing as a process. What we do is an art form.'" That was the case at Lansing as well. "They were adamant there were no processes," Lalain says.
The data would show otherwise, but until they could collect it, Dobis and Prior had to convince the physicians and staff they needed outside help. The two stressed that the patient flow problem was a longstanding one, which the practice had not previously been able to solve. In essence, Prior argued: "Now we have experts. We have to try it."
The staff had other concerns. Because so many of their activities were being measured and timed, they were concerned that the data would be used to reward high performers and punish low performers. To address those concerns, the project leaders emphasized that the overall goal was to improve efficiency and not to target individual employees. "We did that repeatedly," Prior says.
The staff collected data on 1,227 patients, using the previously described time sheet, which was attached to each patient chart during the data collection period. The time required for each exam was entered into an Excel spreadsheet and analyzed by the consultants. The data showed that 241 patients—or 19.6 percent of those measured—had spent more than one hour waiting during their visit. The data also showed that, while there were some 149 exam combinations required by patients, nearly 50 percent followed one of five set patterns. The 242 patients who came for a history, a refraction, dilation, and an exam with the doctor spent an average of 79 minutes in the office, of which 45 minutes was spent waiting (Figure 2).
Figure 2: Top Five Traffic Flow Patterns | |
| Pattern 1 Check-in Podium (a routing station) History EPIC exam (refraction, or measurement of near- or far- sightedness) Dilation Doctor's exam Check-out |
242 patients, Average time: 79 minutes (45 spent waiting) |
| Pattern 2 Check-in Podium History Doctor's exam Check-0ut |
159 patients, Average time: 58 minutes (37 spent waiting) |
| Pattern 3 Check-in Podium History Dilation Doctor's exam Check-out |
90 patients, Average time: 68 minutes (45 spent waiting) |
| Pattern 4 Podium History Doctor's exam Check-out |
64 patients, Average time: 55 minutes (35 spent waiting) |
| Pattern 5 Check-in Podium History EPIC exam Dilation Doctor's exam Test Check-out |
45 patients, Average time: 94 minutes (53 spent waiting) |
| Source: Lansing Ophthalmology, 2007. |
The consultants found great variability in the time taken to perform various procedures. The number of patients seen by doctors per hour ranged from less than two to nearly six (Figure 3). The practice made a decision not to try to alter that variation at the outset. In some cases, there were good reasons for the variability: some physicians were performing more complex procedures or seeing long-term patients who required more face time with doctors. "Eventually they are going to get pulled into the process," Lalain says. But not at first. "Once they are sold on eliminating variation with technicians and everything else, then they might swallow the pill that says they are part of the problem," Lalain says.

Among the technicians, there was also great variability in the time taken to gather histories from patients and perform refractions. Histories took from five to 16 minutes, while EPIC exams (a refraction to measure the degree of a patient's nearsightedness or farsightedness, if any) took from five to 21 minutes, depending on the technician. That variation made it difficult to present a patient to the doctor at the appropriate time.
Another problem revealed by the data was the variation in patient arrival times. Some were as much as an hour early and others were up to 45 minutes late. Because the clinic had a policy of seeing patients when they arrived, patients were inadvertently encouraged to game the schedule, which had tremendous downstream consequences for staff trying to predict the flow of patients and manage their care appropriately.
The data also confirmed what physicians had complained about: patients were bunching outside doctors' offices in large numbers. The problem, consultants pointed out, was caused by the fact that patients were being moved through the system without any recognition for the pace at which doctors were seeing those patients.
To reduce variation in the patient-flow process, the practice:
- instituted a policy of seeing patients at the appointed time. If patients came early, they were told the clinic had to see patients who were scheduled before them. If patients came later than 20 minutes, their visit had to be approved by their physician. Patients are gradually learning that they can't game the system by arriving at a different time than their scheduled visit. This makes it easier to predict what tests will be needed and at what time.
- The clinic formalized its training for technicians to reduce the variation in exam times. The goal was not to bring everyone to the pace of the fastest technicians but rather to address the education and training needs of the outliers. "We really felt we could work on the work-up times," Prior says. "We produced standardized practices for each and had structured training." Among the problems, says Lalain: "They had never taught people how to cut off a conversation gracefully." The result was that patients who chatted with technicians would throw off the schedule.
- The clinic also created a queuing system that limited the number of patients entering the doctors' waiting area. Although this did not address overall wait times for patients, it substantially reduced the stress that doctors felt upon seeing six, seven, or eight patients waiting outside their door. The system they used was relatively simple: A staff member created color-coded cards for each doctor. The number allotted to each was based upon the number of patients he or she could see in one hour. The cards were placed at a desk, which patients were allowed to pass only when a card for his or her doctor was available.
- The scheduling system itself is being restructured to anticipate the time patients require to complete vision tests before meeting with their doctors. This means, in essence, that there are two appointment times: one for meeting with the technician to gather the history and perform a refraction and any additional tests and a second for the time at which the patient will see the physician. Depending on the tests required, the arrival time may be as little as five minutes and as much as 60 minutes before the exam. Because the clinic's software system does not allow schedulers to put two different appointment times in for one patient, the schedulers now have to call patients to notify them of their arrival time. But practice leaders are hopeful that its next software program will automate the process.
Technician time: The goal is 10 minutes for each exam (the previous range was five to 21 minutes). "Everyone is hitting it except for some new people," says Prior. The consultants determined that if the clinic could train the technicians to complete both the history and the refraction in eight minutes each, they could save the equivalent of one and one-half staff positions per year (Figure 4). Prior says that, because the clinic is growing, it would not lay off staff but would use any extra staff to meet the needs of new physicians.

Wait times: "We met the benchmark for a complete eye exam, which is one hour and 16 minutes," says Prior. The average prior to implementation was three minutes more. The clinic expects to see greater time savings when it fully implements the new scheduling system.
Bunching: Doctors only see one or two patients waiting for their visit at any given time. That doesn't mean more patients aren't waiting, as there can still be clusters of patients after 11 am or 4 pm. In those cases, the clinic managers or patient coordinator tries to assign patients to different doctors to smooth out the flow. The goal is to pull patients through the system at the pace at which doctors can see them, rather than push them through without regard for such timing.
Implications: There are some general lessons to learn from the Lansing practice's use of these manufacturing techniques, as outlined below.
Financing: The consultants' services were provided to the clinic at no cost through the AIAG pilot project and, while Prior devoted up to a year on the project, spending anywhere from 10 to 20 hours per week on the improvements, she did this in addition to her regular job. Thus, the practice spent no money for the project. The consultants' fee would have amounted to $20,000, says Lalain. Would the practice have been willing to pay for these services? Only if there was a track record proving that the procedure would be financially worthwhile, answers Dobis. "The issue also is that the process has to have some efficiency in the minds of the doctors, because ultimately they are the ones who are paying for it. They have to be convinced there would be value. I think long term, yes. But the track record has to be (established)," he says.
Having learned process improvement techniques, Prior says the group could apply it to another problem—provided it could find staff with the time to do it. "We would have to take a simple project with a simple goal," she says.
As for savings, the changes allowed the clinic to add slightly fewer support staff when it hired two additional doctors for the practice this year. The ratio of staff to doctors in the main office dropped to 3.1 to 1 from 3.3 to 1.
Applicability to other practices: It's easier to implement such programs in specialties that compete for patients, such as ophthalmology and plastic surgery, as well as practices where the provided services are more routine. It's not impossible to make the same improvements in a primary care practice, says Watkins. "Even in an apparently unpredictable system, there's predictability," he says.
Because of employee resistance to change, it's important to have a highly motivated person shepherding the project. This leader also needs reinforcement. When Prior was frustrated, for example, she could turn to one of the consultants, who would remind her that the things she was experiencing were typical.
For Further Information: Contact David Lalain, director of life sciences for the Automotive Industry Action Group, [email protected], or Teresa Prior, clinical director, Lansing Ophthalmology, [email protected].


