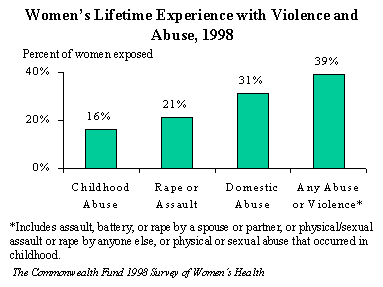The just-released Commonwealth Fund 1998 Survey of Women's Health reveals that while more women are receiving preventive care and taking better care of their health, they are still experiencing alarmingly high rates of violence and abuse, and many continue to have difficulties obtaining quality health care. The survey, which compares findings with the Fund's 1993 Survey of Women's Health, reveals no change in smoking rates and a considerable discrepancy in the receipt of needed health care among high-, medium-, and low-income groups. In addition, many women are providing care for disabled relatives while balancing work and family responsibilities, yet they often have unmet health needs of their own and do not have the help they need to carry out their essential role.
The survey, conducted by Louis Harris and Associates, Inc., from May to November 1998, included 2,850 women and 1,500 men. The good news is that more women age 50 and older and more minority women are receiving mammograms, women are more aware of osteoporosis and how to prevent it, and more are exercising. No difference, however, was found in the use of lifesaving clinical preventive services such as Pap tests and clinical breast exams. Notably, upper-income and college-educated women appeared more likely than low-income women to receive regular preventive care services and counseling on decisions regarding hormone replacement therapy.
"Today's thriving economy provides an excellent opportunity to make long-overdue progress toward improving women's health." said Karen Davis, president of The Commonwealth Fund. "But too many women are being left behind—women who have low incomes, lack health insurance, or must care for sick and disabled family members."
Preventive Care Moving in the Right Direction on Some Measures, Lagging on Others
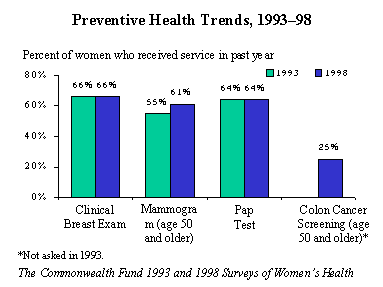
The survey found an increase in the rate of women over age 50 receiving mammograms, from 55 percent to 61 percent. However, rates of women receiving Pap tests (64%) and clinical breast exams (66%) remained the same over the five-year period. Use of preventive care was higher among women with higher incomes, pointing to coverage and cost problems as likely causes of lack of progress. While over four of five (83%) women age 50 and older with incomes above $50,000 had received a mammogram in the past year, only half (49%) of women with incomes of $16,000 or less had done so. Women in managed care plans reported higher rates of some preventive care: three of four (74%) had received a Pap test in the past year, compared with two of three (67%) women in fee-for-service.
The number of minority women over age 50 who received mammograms, however, did rise substantially in the past five years, from 37 percent in 1993 to 66 percent for African American women, and from 54 percent to 64 percent for Hispanic women. Colon cancer screening rates were low, however, with one of four (25%) women receiving this test.
"Barriers still exist—whether due to education, culture, physician communication, or access—to potentially lifesaving women's health care and information," said Karen Scott Collins, M.D., assistant vice president at The Commonwealth Fund. "All of these issues must be addressed by medical practitioners, policymakers, and women themselves. We have come too far in the fight for better health care and recognition from the medical community to stop efforts to ensure that every woman is provided with her best chance to lead a healthy life."
Education Works but Physician Counseling Is Often Lacking
Awareness of the importance of healthy behaviors has increased. Women are more knowledgeable about osteoporosis and are taking calcium supplements, and more women are exercising. However, physicians are more likely to counsel women about exercise (49%) and diet or weight (46%) than more difficult issues such as smoking (29%), alcohol or drug use (23%), sexually transmitted diseases (16%), or violence in the home (8%).
The proportion of women age 50 and older using hormone replacement therapy (HRT) grew from under one of four (23%) in 1993 to one of three (34%) in 1998. Use of HRT corresponds to education and income: one of five (22%) women with less than high school education used HRT, compared with half (49%) of women with a college degree. Only one of five (21%) women with an income of $16,000 or less used HRT, compared with over half (57%) with incomes above $50,000. The rate of women using HRT appears linked to physician counseling: only one of four (25%) low-income women had received counseling about HRT in the past year, compared with three of five (61%) women with high incomes.
Violence and Abuse Rates Are High and Have Lasting Health Effects
The 1998 survey was the first to ask women nationwide about their lifetime experiences of abuse and violence, and rates were found to be disturbingly high. Nearly one of three (31%) women reported that she had experienced violence or physical abuse from a spouse or partner. Three percent of women—the equivalent of 3 million women nationwide—reported experiencing domestic abuse in the past year. One of five (21%) women had been raped or assaulted in her lifetime. Nearly two of five women (39%) reported experiences with either childhood abuse, rape or assault, or domestic abuse. The survey revealed strong links between abuse and a wide range of negative health effects and experiences, including higher rates of depression, reports of fair or poor health, and problems obtaining access to health care. "Violence in the home is a serious and widespread problem—and it is just the tip of the iceberg," said Robert McAfee, M.D., past president of the American Medical Association. "Even one incident of abuse or violence can have lasting, damaging effects on women's health. Physicians must begin to communicate about violence and its effects as a start toward reversing this intolerable threat to the health of women." Fewer than one of ten (8%) women reported their physician had a discussion with them about safety and violence at home.
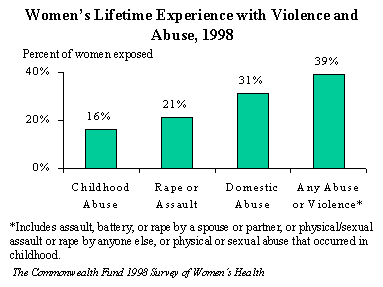
The link between abuse and mental health is striking: over half (53%) of women reported a history of any abuse or violence—whether domestic abuse, childhood abuse, rape, or assault—had a high level of depressive symptoms, compared with 30 percent of women who said they had not been abused or experienced violence.
Gaps in Insurance Coverage Widen for Working-Age Women
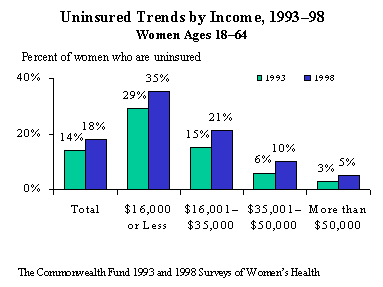
Despite tight labor markets in a thriving economy, in 1998 the proportion of working-age women without health insurance increased. One of four (26%) women ages 18–64 was either uninsured (18%¾ up from 14% in 1993) or had spent a time without insurance at some time in the past year (8%). Although women were still less likely than men to be uninsured, the rate of women without insurance had gone up since 1993, while the rate for men had not changed. Women with low incomes were the hardest hit, pointing to the possible impact of women leaving welfare rolls for low-wage jobs that do not provide health insurance. Over one of three (35%) women with incomes of $16,000 or less were uninsured, up from 29 percent in 1993. In contrast, only 5 percent of women with incomes above $50,000 lacked insurance.
Working-age uninsured women and those who had a lapse in coverage during the past year had lower rates of preventive care and more access problems than those who were continuously insured. While one of six (17%) continuously insured women had at least one of three access problems (did not get needed care or specialty care, or did not fill a prescription because of cost), two of five (40%) women who had spent a time uninsured and nearly half (46%) of women currently uninsured had at least one access problem.
"The extent of the problem of uninsured women is understated," said Cathy Schoen, vice president for research and evaluation at The Commonwealth Fund. "Women who have gaps in coverage experience health and access problems at nearly the same rate as uninsured women. They are falling through the cracks of the system and are often not counted among those with unmet health needs."
Low-Income and Minority Women Are at Greatest Risk
Low-income women are at greater risk for physical and mental health problems on virtually every measure. Women with incomes of $16,000 or less were six times as likely to report fair or poor health as were women with family incomes above $50,000 (32% vs. 5%). More than half (55%) of women in the lowest income category reported high levels of depressive symptoms and were more than twice as likely to report a physician diagnosis of depression or anxiety compared with higher-income women (26% vs. 12%). Low-income women were also more than twice as likely to smoke as women with high incomes (32% vs. 13%).
African American and Hispanic women were more likely than white women to be uninsured: while one of eight (13%) white women under 65 lacked insurance, nearly one of four (23%) African American and over two of five (42%) Hispanic women were uninsured. Hispanic women also had the greatest increase in lack of insurance since 1993, from 33 percent to 42 percent. Some education messages are not reaching minority women: black women (25%), Hispanic women (19%), and Asian American women (17%) were less likely to say they were "very familiar" with osteoporosis than white women (41%).
Caregivers Play an Essential Role
The survey found that nearly one of ten women (9%) and 4 percent of men were informal caregivers for a sick or disabled relative. Low-income women caregivers were likely to devote substantial time providing care: over half of women with incomes of $35,000 or less who were caregivers provided over 20 hours per week of care, compared with 29 percent of caregivers with incomes above $35,000.