The problem of nearly 43 million Americans without health insurance can be virtually eliminated in a single generation by building on the current system, says Commonwealth Fund president Karen Davis in A 2020 Vision for American Health Care, the lead article in the December 11 issue of the Archives of Internal Medicine. Davis and co-authors Cathy Schoen and Stephen C. Schoenbaum, M.D., also of The Commonwealth Fund, argue that because at least a fourth of the federal budget surplus results from savings in Medicare and Medicaid, health care should be a priority when deciding how to allocate the surplus. The "2020" health plan's basic features include:
- Automatic and affordable health insurance coverage for all;
- Easy access to health care;
- Patient-responsive health care;
- Information-driven health care, and
- Commitment to quality improvement.
"Americans want to see the problem of the uninsured solved, and those currently insured hope for more secure future coverage for themselves," says Davis. The "2020" health plan builds on employer-based health care coverage because studies show that a majority of working Americans prefers that system.
"2020" PLAN FEATURES CHOICE AND UNIVERSAL COVERAGE
The "2020" health plan is based on universal, automatic coverage that allows choice of plan and provider. An important difference between the current system and the new proposal is that the "2020" plan provides default coverage: a person will automatically have health insurance until a conscious, informed choice is made to join a specific plan-or to opt out of any coverage. By expanding the existing system in the following ways and providing a safety net for those who fall outside the system, Davis calculates that the number of uninsured would fall to under 6 million:
- All workers, including part-time, temporary, and new employees, would be automatically enrolled in that employer's plan unless the employee opted out. Workers not getting coverage from employers could join the Federal Employees Health Benefits Program (FEHBP).
- Anyone not able to obtain private coverage for health reasons would be covered by Medicare.
- Medicaid and the State Children's Health Insurance Program (CHIP) would automatically cover all families and single people below the federal poverty level who are not otherwise covered by an employer plan or Medicare.
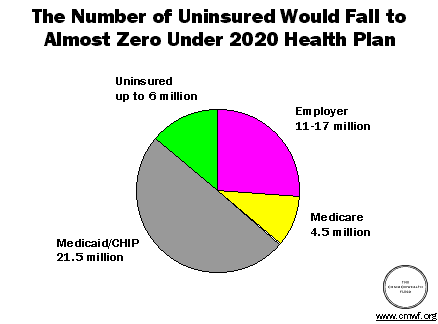
WHO WILL PAY?
Costs would be allocated among all parties that currently finance health care to make the system fairer and more affordable. Employers would continue to contribute at current levels, with a cap based on a percentage of payroll. Employers paying more than that percentage could be eligible for tax credits or other incentives. Employers could choose to not offer coverage, but would be asked to contribute to a pool for uninsured workers. Individual and family contributions for medical expenses and premiums would also be capped at a percentage of family income and excess expenses would be offset through tax credits or other incentives. Health care providers, health insurers, and managed care plans would also continue to contribute a portion of revenues for uninsured care, or for uncovered services such as outreach or patient education.
ACCESS TO PATIENT-REPONSIVE, QUALITY CARE IS KEY
An important component of the "2020" plan is the assurance of comprehensive benefits providing easy access to a full range of services, including preventive care, prescription drugs, mental health care, and dental care. Each person will be encouraged to have a personal physician responsible for coordinating their care; an annual covered visit will provide incentive to choose a doctor.
Practices would be encouraged to adopt open access scheduling, allowing patients to schedule their own appointments by phone or over the Internet. Patients would be assured easy access to their complete medical records, and the right to know about their treatment and the quality of care provided by their doctors. Finally, the "2020" health plan would build in a commitment to improve quality of care through clinical information systems to aid decision-making, measure quality of care, and promote quality management. In an editorial in the same issue, Archives of Internal Medicine editor James E. Dalen, M.D., called the "2020" plan "the first feasible plan for achieving near-universal health care insurance that I have seen."
The article is based on the John R. Hogness Award Lecture, delivered by Davis in October at the annual meeting of the Association of Academic Health Centers in Tucson, Arizona. According to Davis, "we need a bold approach, one that does justice both to the magnitude of the problems in the current system and to our economic resources, technological capacity, creativity, and commitment of health care professionals and leaders."


