New York City, April 1, 2004—There have been few takers as yet for a 2002 federal law offering certain unemployed workers tax credits to help them buy health insurance, a new Commonwealth Fund/Nathan Cummings Foundation study finds. Although enrollment likely will increase over time, some provisions of the law may be barriers to participation, the study's authors say.
The new report, which analyzes the Health Coverage Tax Credits (HCTC) program created by the 2002 Trade Act, shows that just 3.6% of 235,000 potentially eligible workers—a total of 8,400—were enrolled at the end of 2003. Additional eligible workers will take the tax credit when they file their 2003 income tax. That number will be reported by the administration in June. At this early point in the program, say report authors Stan Dorn and Todd Kutyla of the Economic and Social Research Institute (ESRI), the precise causes of this low rate of uptake are unclear, as is its future persistence. But, they say, barriers to enrollment that may need to be addressed include premiums that appear to be too high for many unemployed workers, even with a tax credit, and requirements that laid-off workers "front" one or more months of premiums in full before the advance tax credit kicks in.
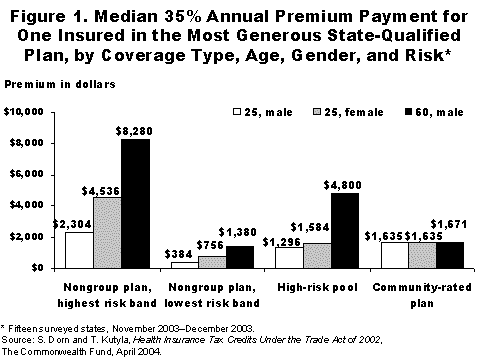
In addition, Health Coverage Tax Credits Under the Trade Act of 2002 notes concerns about the state-based health plans for which credits may be used, finding that benefits are often limited and that women, middle-aged and older workers, and individuals with prior health problems are frequently asked to pay significantly more than young, healthy men purchasing the same coverage.
 On the positive side, say the authors, the program has developed an impressive electronic system for advancing income tax credit payments to beneficiaries through an innovative federal/state/private partnership; most beneficiaries have access to state health plans for which credits can be used; and officials have been remarkably responsive in addressing emerging problems.
The study provides some of the first published data on the impact of fully refundable and advanceable federal income tax credits for health insurance. The issue is especially important as many policymakers in both political parties consider tax credits as a solution to the growing problem of uninsured Americans. For example, both President Bush and Senator Kerry propose using tax credits to cover various groups of uninsured.
"Refundable, advanceable tax credits to cover the uninsured are a new experiment, which will bear close watching to determine if barriers to enrollment can be overcome," said Commonwealth Fund President Karen Davis. "Tax credits have been an integral part of many proposals to reduce the numbers of uninsured, so it's particularly important to monitor how well the system works and learn the most effective ways of structuring such credits."
Trade Act HCTCs pay 65% of premiums for health insurance coverage of workers who lose their jobs because of international trade and certain early retirees who lose pensions due to a company's bankruptcy. They are fully refundable, meaning they may be claimed in full by all eligible individuals, regardless of whether they owe federal income tax. HCTCs may be used to buy qualified insurance, which includes COBRA coverage and state-arranged insurance. The credits are also advanceable, which means the beneficiary does not have to put up the money first and wait to file annual tax forms before receiving the credit. Rather, the HCTC can go directly to the insurer when monthly premiums are due, making it much more affordable. Alternatively, the beneficiary can wait to claim the HCTC as a refund of health insurance payments on annual income tax forms. The number of HCTC recipients thus may increase significantly when such forms are filed later this month. This is the first time in a decade federal income tax credits have been used for health coverage.
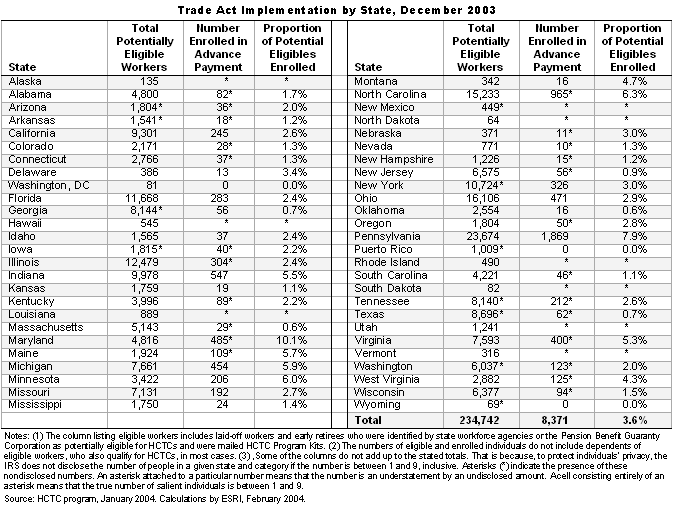
The report's analysis of enrollment in the HCTC program as of December 2003 found the proportion of potential eligibles who enrolled in advance payment ranged from zero in the District of Columbia and Wyoming, to up to 10.1% in Maryland. (See chart.)
But the study also notes a series of successes, including:
On the positive side, say the authors, the program has developed an impressive electronic system for advancing income tax credit payments to beneficiaries through an innovative federal/state/private partnership; most beneficiaries have access to state health plans for which credits can be used; and officials have been remarkably responsive in addressing emerging problems.
The study provides some of the first published data on the impact of fully refundable and advanceable federal income tax credits for health insurance. The issue is especially important as many policymakers in both political parties consider tax credits as a solution to the growing problem of uninsured Americans. For example, both President Bush and Senator Kerry propose using tax credits to cover various groups of uninsured.
"Refundable, advanceable tax credits to cover the uninsured are a new experiment, which will bear close watching to determine if barriers to enrollment can be overcome," said Commonwealth Fund President Karen Davis. "Tax credits have been an integral part of many proposals to reduce the numbers of uninsured, so it's particularly important to monitor how well the system works and learn the most effective ways of structuring such credits."
Trade Act HCTCs pay 65% of premiums for health insurance coverage of workers who lose their jobs because of international trade and certain early retirees who lose pensions due to a company's bankruptcy. They are fully refundable, meaning they may be claimed in full by all eligible individuals, regardless of whether they owe federal income tax. HCTCs may be used to buy qualified insurance, which includes COBRA coverage and state-arranged insurance. The credits are also advanceable, which means the beneficiary does not have to put up the money first and wait to file annual tax forms before receiving the credit. Rather, the HCTC can go directly to the insurer when monthly premiums are due, making it much more affordable. Alternatively, the beneficiary can wait to claim the HCTC as a refund of health insurance payments on annual income tax forms. The number of HCTC recipients thus may increase significantly when such forms are filed later this month. This is the first time in a decade federal income tax credits have been used for health coverage.
The report's analysis of enrollment in the HCTC program as of December 2003 found the proportion of potential eligibles who enrolled in advance payment ranged from zero in the District of Columbia and Wyoming, to up to 10.1% in Maryland. (See chart.)
But the study also notes a series of successes, including:
- The interagency HCTC team and its contractors met the statutory deadline of August 1, 2003 to have advance payment up and running, a significant accomplishment as no similar payment system had existed before.
- By the end of 2003, state-based coverage was available in 26 states and the District of Columbia, representing three-fourths of all projected eligible workers.
- Despite the challenges of multiple federal agencies working together, officials successfully developed program infrastructure through a federal-state-private partnership, using an electronic system for exchanging information and payments, and repeatedly adjusting the program to solve emerging problems.
- For many beneficiaries, premiums are unaffordable, even with credits covering 65% of the cost. For unemployed workers and early retirees receiving HCTCs, their 35 percent premium share averages $1,713 a year for single coverage. By contrast, American employees receiving a paycheck contribute, on average, only $508 a year for single coverage furnished by their employers.
- Enrollees must pay full premiums before advance payment begins. To obtain advance payments, beneficiaries must first enroll in a qualified health plan and pay the full premium for one or more months. While reimbursement for such payments is available after annual tax forms are filed, many laid-off workers and early retirees can't afford monthly health insurance premiums based on the hope of future refunds.
- Outreach methods may be ineffective for many potentially eligible enrollees. Outreach consists mainly of mailing potentially eligible individuals a detailed and complex 20-page booklet, which may be difficult for many in the target population to understand.
 For more detailed information, see the full report.
For more detailed information, see the full report.


