The U.S. Congress is on the threshold of historic change that will usher in a new era in American health care. In the last 50 years, three presidents—Nixon, Carter, and Clinton—have made a serious effort to enact reform and failed. The nation simply can not afford to fail again—too much is at stake for those Americans who fail to get the life-saving care they need and for those who pay the bills of the ever-rising cost of health care. History makes clear that failing to act on health reform has serious and far-reaching economic ramifications. An examination of trends in health spending over the past 50 years shows that if health reform measures proposed by previous presidents had been enacted and slowed the growth in spending by as little as 1.0 or 1.5 percentage points annually, spending trends in the U.S. would have been closer to those seen in other major industrialized countries and fewer adverse health consequences and economic burdens would have been borne by American families, businesses, and government.
Learning from Past Efforts
Over the last half-century, the nation has made several serious attempts to ensure health insurance coverage and control health care spending, either as part of comprehensive legislation or through companion measures.
President Richard Nixon imposed wage and price controls on the entire economy in 1971 in the wake of inflation triggered by the Vietnam War, with special mechanisms developed for controlling health care costs. He then proposed a Comprehensive Health Insurance Plan that received serious legislative consideration in 1974. The central features of the plan were employer-mandated private insurance coverage for workers and their families in firms with 25 or more employees, a plan for low-income families that would replace and improve Medicaid, and a federal health insurance plan that would replace and improve Medicare.1 Reform efforts died when Nixon was removed from office, as proponents hoped to enact stronger legislation in the political aftermath of his impeachment. The Nixon health care cost controls were lifted in 1975 when the industry pledged to control costs voluntarily.2
President Jimmy Carter proposed hospital cost containment legislation in 1977. In 1979, he introduced a national health plan that included minimum standards on benefits and required employer contributions, as well as a new federal HealthCare program to replace Medicaid and Medicare and cover all low-income individuals, in addition to the elderly and disabled. The Carter hospital cost containment legislation, a response to the explosion in health care costs following the lifting of Nixon's health cost controls, was defeated when the industry mounted an alternative "Voluntary Effort." Unfortunately, this voluntary approach to cost control also quickly dissipated once the threat of legislation was removed.3 Inflation in health care spending and a deteriorating economy contributed to the demise of the Carter national health plan in 1980.
President Bill Clinton introduced legislation in 1993 with cost containment measures built into health reform. In particular, his proposal called for controls on the rate of increase in health insurance premiums. The Health Security Act included an employer mandate that required employers to pay 80 percent of the premium (up to a maximum of 7.9% of payroll), with the family share of premiums not to exceed 3.9 percent of income.4 The plan was to be financed by substantial Medicare and Medicaid savings, an increase in tobacco taxes, and cross-subsidies among employers within risk pools. President Clinton's health reform ran into major opposition from small businesses and insurers, and the legislation stalled out in Congress.
U.S. Health Spending Trends and Projections
The federal government's repeated failure to enact health reform has had serious consequences for American government, families, and businesses. The U.S. spent 5 percent of gross domestic product (GDP) on health care in 1960; health care now consumes 17 percent of the nation's economy and will reach 21 percent by 2020, if trends continue. While investment in health care has contributed to improved health and productivity, other countries have devoted a far lower share of GDP to health care and achieved comparable or better health outcomes.
Ever-higher health spending has directly contributed to stagnating incomes and rising health insurance premiums for middle-class families and workers. Commonwealth Fund analysis has shown that premiums have risen from 11 percent of family income in 1999 to 18 percent in 2009. If current trends continue, average family premiums will reach 24 percent of median income by 2020.
Rising health care costs—and the subsequent rise in health insurance premiums—have fueled an increase in the number of Americans without insurance over the past three decades. Nearly 50 million Americans are expected to be uninsured in 2010. Cost growth also has placed enormous pressure on employers' ability to provide comprehensive benefits, leading many to shift to less generous policies or drop coverage altogether. Employees of small businesses, which are much less likely to offer coverage, are at particularly high risk.
It is difficult to estimate with precision what would have happened had proposed reforms been enacted. Still, it is instructive to consider where we would be today if those efforts had succeeded. Each included provisions designed to provide health insurance coverage for all.5 Each set out regulatory restraints on the growth in provider payment or insurance premiums, or both. All had significant mechanisms to control costs, including changing provider payment, increasing competition in the insurance market, and controlling the growth in private insurance premiums.
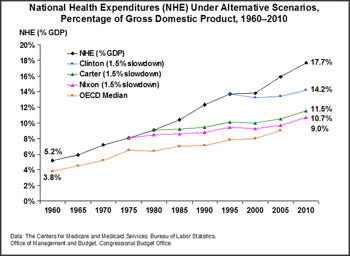
Exhibit 1 shows the growth in national health expenditures as a percentage of GDP and what we would have spent as a nation if effective measures to slow the growth in health expenditures by 1.5 percentage points a year had been adopted in 1975, 1980, and 1995. In 1960, we spent 5.2 percent of GDP on health care, compared with the 3.8 percent of GDP median rate in all major industrialized nations. Today, we spend 17.7 percent—nearly twice the rate of 9 percent that is devoted to health care in other industrialized countries.
If President Nixon's health reform plans had been enacted in 1975 and slowed the annual rate of spending by 1.5 percentage points a year, today we would be spending 10.7 percent of GDP on health care. In dollar terms, we would spend only $1.6 trillion on health care in 2010, instead of projected health spending of $2.6 trillion. This savings of $1 trillion in 2010 alone would remove much of the financial burden on families, businesses, and government. Even if Nixon reforms had slowed spending growth by "only" 1 percentage point a year, health spending as a percent of GDP would have been $1.9 trillion in 2010, or 12.7 percent of GDP—a savings of 5 percent of GDP.
If cost containment measures slowing spending by 1.5 percentage points a year had been enacted in 1980 under President Carter, the trends would be similar, with spending rising to $1.7 trillion in 2010, or 11.5 percent of GDP. Even if we had acted as late as 1995 under President Clinton, health spending in 2010 would be $2.1 trillion, or 14.2 percent of GDP.
The federal government would have been a major beneficiary of comprehensive health reform under Presidents Nixon, Carter, or Clinton. Instead of consuming 6.2 percent of GDP in 2010, federal health outlays would have been 3.7 percent in 2010 under Nixon reforms that slowed spending growth by 1.5 percentage points, 4.0 percent under Carter, and 5.0 percent under Clinton.
Bending the Health Care Cost Curve Today
In the current round of health reform, the primary strategy for controlling costs has been legislative changes to Medicare and a public health insurance plan that encourages private insurers to control costs. While enrollment in the public health insurance plan in the House bill has been narrowly targeted on the uninsured and small businesses, the proposal faces an uncertain future in the legislative process.
The House of Representatives has added provisions to negotiate pharmaceutical drug prices, review insurance premium increases, and set standards on the share of premiums devoted to health care. Both the House and Senate have provisions for rapid testing of new methods of provider payment in Medicare. The Senate bill calls for an independent Medicare advisory board to facilitate rapid consideration of recommendations to limit the rate of increase in Medicare outlays.
Several commentators have questioned whether the cost containment provisions in the health reform bills passed by the House and under consideration in the Senate are sufficient. Neither bill includes the aggressive system-wide cost control measures that were part of the Nixon, Carter, and Clinton proposals. But the House and Senate bills would begin to bend the curve in total health spending and encourage the development of mechanisms for extending cost control measures more broadly once experience is gained. A recent analysis by the Council of Economic Advisers estimates that private and governmental spending would be slowed by 1.0 percentage points a year.
History shows that even modest cost-cutting has a significant impact over time and that inaction has a cost. The longer we wait to address the underlying problems in the U.S. health care system, the more health spending will continue on its rapid rise and the more drastic the measures that will be required to right our economy and our federal budget. Congress is right to move ahead. After 50 years of spiraling health care costs and the resulting price paid by American families, business, and government, we can no longer afford to postpone health reform.
1 K. Davis, National Health Insurance: Benefits, Costs, and Consequences (Washington, D.C.: The Brookings Institution, 1975).
2 K. Davis, G. Anderson, D. Rowland, and E. Steinberg, Health Care Cost Containment (Baltimore: The Johns Hopkins University Press, 1990).
3 K. Davis, "Recent Tends in Hospital Costs: Failure of the Voluntary Effort," Testimony before the House Committee on Energy and Commerce, December 15, 1981.
4 Congressional Research Service, Health Care Reform: President Clinton's Health Security Act, (Washington, D.C.: Congressional Research Service, 1993).
5 K. Davis, "Universal Coverage in the United States: Lessons from Experience of the 20th Century," Journal of Urban Health: Bulletin of the New York Academy of Medicine, March 2001 78(1).