Rising health care costs are putting financial pressure on all tiers of government, as well as businesses and individuals. While the rate of health spending growth has slowed in recent years, policymakers are looking for long-term solutions. Over the past year, several prominent groups have proposed policy options to contain costs and transform the health care delivery system. Even though these organizations represent a variety of perspectives, there are substantial areas of consensus among their proposals. The Commonwealth Fund, working with The George Washington University Department of Health Policy, examined reports from seven organizations with comprehensive approaches to controlling health spending.
After careful analysis, this examination revealed substantial agreement on areas where action is needed. Moreover, even where the reports differ on specific recommendations, they are close enough to suggest commonality among these approaches to slowing health spending through health system reform. A matrix summarizing and comparing the policies in these reports is available on our website, and in this post, we briefly review the high-level areas of consensus.
Paying for Value, Not Volume
The need to move from paying for the volume and intensity of health care services provided to paying for the value of those services is an area of strong consensus. Policies in this area would accelerate the transition from our current fee-for-service payment system, which largely disregards appropriateness or effectiveness, to a system that rewards better health outcomes and focuses on using resources efficiently. 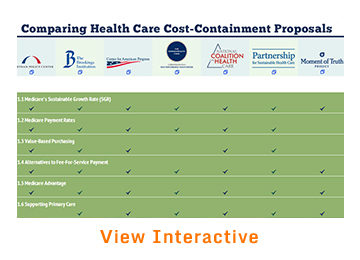
All of the proposals call for expanding payment and delivery system reforms already under way and for developing and implementing new reforms. Each proposal recommends incentives for providers and patients to participate in patient-centered medical homes and other models of coordinated care. There is also strong support for building on the accountable care organization (ACO) model to establish networks of providers that focus on effective and efficient care and reward providers and their patients for achieving those objectives. All of the proposals recognize the importance of establishing consistent payment policies across public programs, such as Medicare and Medicaid, and private payers.
Several reports suggest using the new health insurance marketplaces as a vehicle for encouraging payment and delivery system reform, by encouraging the plans participating in the exchanges to develop and implement innovative approaches to payment.
Quality Improvement and Patient Engagement
All of the reports reflect the importance of improving the quality of care and engaging patients in that process. The policies include identifying and encouraging the adoption of best practices, including better-targeted and more consistently applied quality measures, enhancing availability of preventive care, shared decision-making among patients and providers, value-based insurance design and purchasing of health care, and better access to support services to complement medical care. Several proposals also call for malpractice reforms that would protect physicians who adopt evidence-based clinical practices.
Enhancing patient engagement, for example by making information about the quality and price of health care services available to patients, is also a common focus. New Medicare coverage options that rationalize cost-sharing requirements and incorporate incentives for beneficiaries to choose high-performing health care providers are also recommended in several of the reports.
Improving Market Competition
Another major area of consensus is the need to improve market competition to enhance quality and lower costs. Most of the reports recognize the need for improved information, administrative simplification, and increased oversight efforts at the federal level to combat fraud and enforce the rules of a well-functioning health care market.
Most of these proposals also support increasing the use of competitive bidding, so that Medicare can obtain the best prices for drugs, durable medical equipment, laboratory tests, and other medical commodities. They also call for policies promoting increased generic drug use and more aggressive purchasing. Various mechanisms are suggested for doing this, including reducing the exclusivity period for brand-name biologics, prohibiting “pay for delay” agreements for drug exclusivity, and modifying Medicare Part B payment for outpatient drugs.
Setting Spending Targets
All of the reports recommend establishing some type of spending target to stabilize health care spending growth. These include spending caps or targets at the federal or state level. In addition, as a way of setting limits on spending for certain high-cost or inefficient health care services, all of the reports propose increasing bundled payment approaches within hospital, postacute care, and other services. Several organizations note that by establishing a single fee for care that involves multiple providers and provider types (often across care settings), quality and efficiency problems could be reduced.
The Way Forward
As policymakers continue to search for ways to control health spending, the policies described in these reports could point the way toward a solution that preserves the ability of Medicare to serve the needs of its aged and disabled beneficiaries and enables other public programs to fulfill their missions. If implemented, these policies could help both the public and private sectors benefit from improved engagement of both providers and patients in making health care decisions.
The way forward will not be easy, and it will take coordination and cooperation among the various stakeholders in the health system, but the potential benefits are great—and the answers are becoming clearer.





