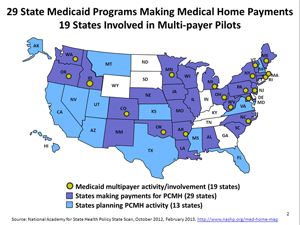
Strong primary care is essential to improved health outcomes, lower costs, and increased equity, and the patient-centered medical home is a potentially key strategy for transforming primary care. The medical home is a model of primary care that leverages a team of health care providers to offer comprehensive, coordinated care available around the clock. Private health plans in 49 states are testing this model and 19 states are involved in multipayer medical home pilots.
On May 3, more than 180 congressional and administration staff, journalists, and other Washington, D.C., policy stakeholders convened for a briefing to discuss the status of the medical home pilots and preliminary results of their effect on health outcomes, quality of care, patient and provider satisfaction, and health care costs.
The briefing featured Meredith Rosenthal, Ph.D., a professor of health economics and policy at Harvard School of Public Health; Sean Cavanaugh, acting deputy director, programs and policy, at the Center for Medicare and Medicaid Innovation; and Barbara Tobias, M.D., medical director at the Health Collaborative in Cincinnati. The briefing was comoderated by Alliance for Health Reform chairman Robert Graham, M.D., and Commonwealth Fund vice president of patient-centered coordinated care Melinda Abrams.
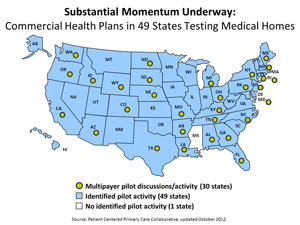 Abrams opened the discussion with a review of the value of primary care and its potential to reduce health care costs, as well as a look at the weaknesses in U.S. primary care today. A majority of Americans report difficulty obtaining timely access to care and many do not have a designated primary care provider, resulting in poorly coordinated care. Concurrently, primary care’s longer hours and lower wages make it a more difficult practice environment than is seen in other specialties. Abrams said the transformative potential of the medical home is widely recognized, however, pointing to the pilots under way across the country.
Abrams opened the discussion with a review of the value of primary care and its potential to reduce health care costs, as well as a look at the weaknesses in U.S. primary care today. A majority of Americans report difficulty obtaining timely access to care and many do not have a designated primary care provider, resulting in poorly coordinated care. Concurrently, primary care’s longer hours and lower wages make it a more difficult practice environment than is seen in other specialties. Abrams said the transformative potential of the medical home is widely recognized, however, pointing to the pilots under way across the country.
Rosenthal addressed the growing body of literature around medical homes, which shows improved quality measures and increased patient and provider satisfaction. Rosenthal underscored that transformation requires a sequence of steps and that cost savings will not be realized right away. She has found that cost savings are more likely to occur when there is alignment in incentives and care coordination across the whole system, such as among primary care practices, specialists, and hospitals.
|
Lessons from Multipayer Patient-Centered Medical Home Pilots
Source: M. Rosenthal, "What Do We Know About the Effects of Medical Homes on Health Care Costs?" presentation at the Alliance for Health Reform briefing sponsored by The Commonwealth Fund, Washington, D.C., May 3, 2013. |
Sean Cavanaugh provided an overview of the Center for Medicare and Medicaid Innovation’s investment in primary care transformation. There are currently four active demonstrations: Independence at Home, Federally Qualified Health Center Advanced Primary Care Practice, Multi-Payer Advanced Primary Care Practice, and the Comprehensive Primary Care Initiative. Cavanaugh emphasized that fostering collaboration among multiple payers, both public and private, and offering providers a common payment method, are essential to promoting primary care transformation.
 One of the seven markets selected to participate in the Comprehensive Primary Care Initiative is Cincinnati, and Tobias of the Health Collaborative discussed her organization’s experience as part of this demonstration. The participating practices have already seen improved clinical outcomes, such as in diabetes reporting factors. And preliminary results show that there was lower utilization of emergency department care and shorter hospital stays, both of which could reduce costs over time.
One of the seven markets selected to participate in the Comprehensive Primary Care Initiative is Cincinnati, and Tobias of the Health Collaborative discussed her organization’s experience as part of this demonstration. The participating practices have already seen improved clinical outcomes, such as in diabetes reporting factors. And preliminary results show that there was lower utilization of emergency department care and shorter hospital stays, both of which could reduce costs over time.
During the question-and-answer session, the panelists and audience explored how to sustain the momentum of the pilots and spread the medical home model. The panelists agreed that there is a need for stronger evidence to conclude that the primary care medical home will be successful in every environment. Early results, however, indicate that good relationships with other specialists and hospitals, a sophisticated information system, and regular reporting of data are critical to the success of any medical home program.
The panelists also recognized that the payment model will need to be tweaked continually to maintain momentum and offer a mix of value-based and fee-for-service payments and positive consumer incentives. The Alliance’s Graham closed the briefing by observing that many providers are excited about the primary care model because it ultimately creates the kind of system they want to work—one that satisfies patients by delivering better-quality care.




