For the first time in almost three years, states will soon resume redetermining whether Medicaid beneficiaries are still eligible for the program. Since February 2020, enrollment in Medicaid and the Children’s Health Insurance Program (CHIP) has grown by 19 million people. Under COVID-19 relief legislation, state Medicaid programs were given a boost in federal financing so long as they refrained from terminating coverage during the public health emergency. But recent legislation puts the gains in insurance coverage in jeopardy — starting April 1, 2023, states can once again terminate Medicaid and CHIP coverage for people they deem ineligible.
The U.S. Department of Health and Human Services estimates that 15 million people could lose their Medicaid and CHIP coverage under this new legislation. Of those, only about 2.7 million will be eligible for subsidized marketplace coverage and another 5 million for employer-sponsored insurance. Other studies have made similar projections.
As states prepare to resume Medicaid eligibility redeterminations, government officials are focused on strategies to promote continuity of coverage to minimize the number of people who become uninsured or face gaps in coverage. The federal Centers for Medicare and Medicaid Services has provided states with guidance on when and how to conduct redeterminations, and the federal health insurance marketplace has dramatically increased funding for consumer outreach and assistance. Several state-based marketplaces also are preparing innovative programs, such as autoenrolling people into health plans and premium assistance, to ease coverage transitions.
But continuity of coverage is only one piece of the puzzle — even those who successfully shift to another coverage option face the risk of disrupted care and loss of access to providers they were seeing under their Medicaid plans. Many of these people will be in the midst of treatment, pregnant, or have serious chronic conditions. It is, therefore, critically important for states to develop strategies to promote continuity of care.
Gaps in “Continuity of Care” Protections
Provisions in the federal No Surprises Act require group health plans and insurers to allow certain patients, for a specified period, to pay no more than in-network cost sharing for services from providers that leave their plan’s network. These “continuity of care” protections apply to patients with serious and complex conditions who are undergoing treatment, such as those who are pregnant, terminally ill, scheduled for nonelective surgery, or undergoing a course of institutionalized or inpatient care. The protection is available for up to 90 days or for the duration of the patient’s treatment. Twenty-nine states offer similar protections to enrollees who lose access to an in-network provider because the provider has left or been terminated from their health plan’s network.
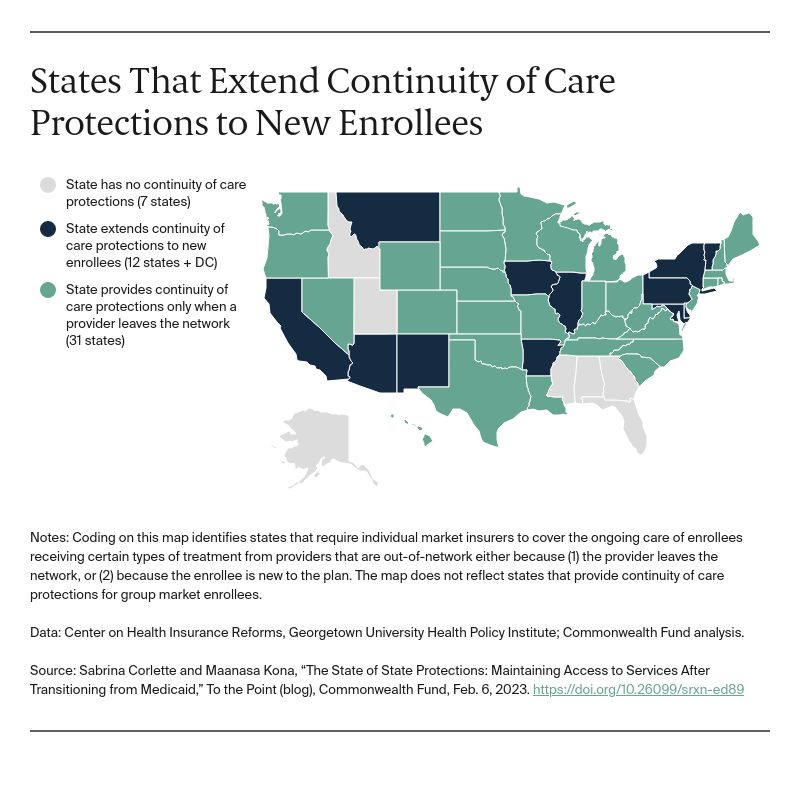
While critical, the federal and most state continuity of care protections are limited, since they are triggered only after a provider leaves a plan network. These protections do not extend to scenarios in which patients lose access to providers they are receiving treatment from because patients enroll in new plans. This could occur if a patient loses eligibility for Medicaid and has to enroll in marketplace insurance, for instance. Currently, only 12 states and the District of Columbia extend their continuity of care protections to certain high-need patients as they transition from Medicaid to a new plan that does not include their treating providers.