New York City, April 4th, 2006—Despite spending more than twice as much per capita as other countries do on health care, the U.S. health care system ranks lower than several other countries in patients' perspectives of the safety, efficiency, equity, and patient-centeredness of health care. The U.S. scored well on effectiveness of care, especially preventive care. However, the U.S. also stands out for having wide and pervasive health care disparities based on income.
The findings are from two new Commonwealth Fund reports analyzing cross-national surveys of adults' health care experiences in Australia, Canada, Germany, New Zealand, the U.K., and the U.S. One report focuses on overall U.S. performance, ranking the national average based on patient reports in two cross-national surveys. The companion report examines patients' experiences with primary care by income.
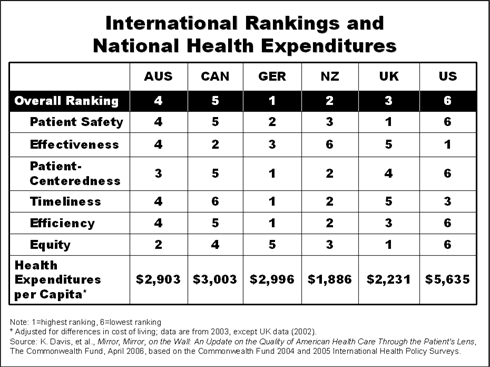
On overall performance, the studies find that the U.S. ranks last on patient safety, patient-centeredness, efficiency, and equity, and third on timeliness compared to adults in the other five nations surveyed. The U.S. performed best of the six countries on delivering preventive care services, an indicator of effective quality of care.
"While it is heartening that the U.S. ranks first on measures of effectiveness, the low rankings of the U.S. in other dimensions of quality of care are particularly disturbing considering we lead the world in health care spending. Our fragmented health care system and lack of a strong primary care foundation show up in performance gaps throughout the studies, with particularly negative results for patients vulnerable due to poor health or lower incomes," said Commonwealth Fund President Karen Davis. "Contrasting the experiences of patients in the U.S. with those in other countries provides evidence that it is possible to provide care that is more efficient, effective, safe, patient-centered, and equitable."
In Mirror, Mirror, on the Wall: An Update on the Quality of American Health Care Through the Patient's Lens, Commonwealth Fund President Karen Davis and colleagues analyze data from two Commonwealth Fund International Health Policy Surveys using a framework set out by the Institute of Medicine to evaluate the quality of a health care system. The findings are based on a 2004 survey of primary care experiences in five countries and 2005 survey of patients with health problems in six countries. Out of 51 indicators of quality of care, the U.S. ranked first on six indicators and last or tied for last on 27.
Key findings from Mirror, Mirror include:
- Patient safety: The U.S. ranked last on patients experiencing a lab test error, including wrong tests or delays in being notified about abnormal test results.
- Effectiveness: The U.S. ranks first on preventive services such as pap tests (85% in the U.S. compared to 58%–70% in other countries) and mammograms (84% in the U.S. compared to 63%–77% in other countries) and on providing counseling on diet and exercise (35% in the U.S. did not receive counseling, compared to 40%–54% in other countries). However, the U.S. ranks last on patients not filling a prescription, skipping a recommended test, treatment, or follow-up, or not visiting a doctor when needed due to cost (51% in the U.S. compared to 13%–38% in other countries).
- Patient-centeredness: The U.S. ranks last on patients leaving a doctor's appointment without getting important questions answered (24% for U.S. compared with 15%–21% for other countries).
- Timeliness: The U.S. ranks last on difficulty of getting needed care on nights or weekends, although Australia also ranks low on this measure (61% for U.S. compared with 25%–59% for other countries).
- Efficiency: The U.S. ranks last on visiting the emergency room for a condition that could have been treated by a regular doctor, if he or she had been available (26% for U.S. compared to 6%⁷21% for other countries).
- Equity: The U.S. ranks worst on differences between below and above-average income patients not filling a prescription or skipping doses due to cost (26% difference for U.S. compared to 0% to 16% for other countries).
The second study, The U.S. Health Care Divide: Disparities in Primary Care Experiences by Income—Findings from the Commonwealth Fund 2004 International Health Policy Survey by Phuong Huynh, associate director of the Fund's International Health Policy program and colleagues, presents new analysis of data from the Fund's 2004 survey of primary care in five countries by income, with comparisons within and across countries. The researchers found widespread disparities by income in the U.S., and also that U.S. patients with lower incomes were more likely to have negative care experiences than their counterparts in other countries.
The U.S had significant disparities between below- and above-average income patients on 21 of 30 measures of primary care access, coordination, and doctor-patient relationships included in the study. In the other countries, differences by income in patient-reported care experiences were relatively rare. The U.K. had the most equitable patient-reported care experiences by income, but income-related disparities were also relatively rare in Australia, Canada and New Zealand.
Comparing care experiences of below-average income U.S. adults to their counterparts in the other countries, the U.S. also performed poorly. U.S. lower-income adults ranked last or tied for last with lower-income adults on more than half (16) of the 30 primary care indicators in the study.
"In a country with a wealth of medical care resources that prides itself on equal opportunity, these patient reports reveal a health divide, with negative consequences for the health and productivity of our workforce as well as for modest and lower-income families." said Commonwealth Fund Senior Vice President Cathy Schoen, a co-author of the study. "The nation stands to gain if we could move forward toward insurance and delivery system changes to provide more timely and coordinated access to care with financial protection."
The study further finds that U.S. uninsured adults are particularly at risk for access barriers, lower quality care and less efficient care. U.S. uninsured adults stand out within the U.S. and cross-nationally for high rates of going without care because of costs, emergency room use, more negative experiences in doctor-patient communication and care and for poorly coordinated care, including duplicate tests and never hearing about diagnostic test results.
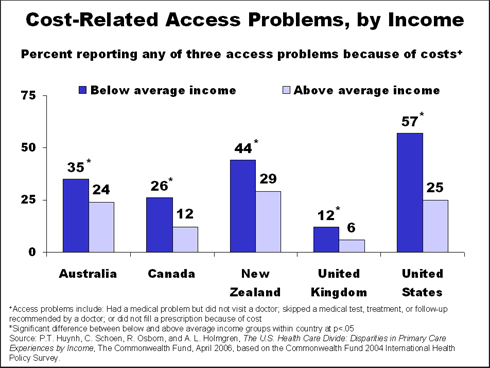
Selected findings from The U.S Health Care Divide include:
- One–fifth (22%) of below-average income U.S. patients rated their doctor fair or poor, compared with 7% of above-average income U.S. patients. Negative ratings of doctors ranged between 4% and 12% in other countries.
- Lack of insurance intensified disparities within the U.S. Three-quarters (76%) of uninsured US adults went without needed care because of cost in the past year. Uninsured adults also experienced more fragmented and disconnected care.
- Yet, even with insurance, below-average income Americans still report greater rates of access barriers and coordination concerns than above average income, insured Americans.


