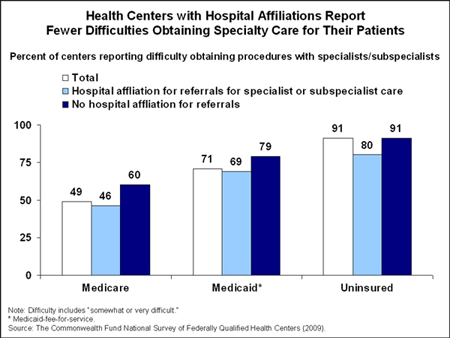
New York, NY, May 27, 2010—Community health centers that are closely affiliated with hospitals have fewer difficulties getting their patients appointments for specialty procedures like x-rays, diagnostic tests, and visits with specialist physicians, according to a new Commonwealth Fund survey of community health centers released today. Centers without hospital affiliations reported they had more difficulty getting off-site specialty appointments regardless of a patient's insurance status—pointing to the need for incentives that will promote connections between health centers and specialty care providers.
 The report, Enhancing the Capacity of Community Health Centers to Achieve High Performance, is a comprehensive national survey of nearly 800 Federally Qualified Health Centers across the country. It examines centers' capacity to provide high quality health care and function as patient-centered medical homes.
The report, Enhancing the Capacity of Community Health Centers to Achieve High Performance, is a comprehensive national survey of nearly 800 Federally Qualified Health Centers across the country. It examines centers' capacity to provide high quality health care and function as patient-centered medical homes.
Coming on the heels of health reform legislation that will increase community health centers' funding by $11 billion dollars over the next five years—a doubling of current funding—the report spotlights areas where improvements can be made, including: payment incentives to encourage high quality care; policies and incentives that encourage centers to take the necessary steps to function as patient-centered medical homes; and infrastructure support like health information technology (IT) that will allow health centers to better meet patients' needs.
A critical component of the health care safety net, community health centers serve an estimated 16 million patients who are predominantly low-income, uninsured, or insured through Medicare or Medicaid. According to the report, many community health centers already provide high quality, well-coordinated care, but the passage of the Patient Protection and Affordable Care Act could increase demand for their services nationwide, much as it did after Massachusetts passed comprehensive health reform.
"Community health centers are a vital component of our health care system and this survey gives us a comprehensive picture of their current capacity to provide patient-centered, high-quality care," said Commonwealth Fund President Karen Davis. "Moving forward, we should continue to invest in strategies—payment reform, health IT, and partnerships—that will strengthen community health centers' ability to provide comprehensive care to patients and reduce barriers to obtaining needed specialty care."
Community Health Centers as Medical Homes
The patient-centered medical home approach to primary care focuses all aspects of a physician practice—from appointment scheduling to the way medications are prescribed—on the needs of patients. The survey used five different medical home indicators to determine the extent to which a center functioned like a medical home. It found that 29 percent of centers had all five of the indicators of a medical home, 55 percent had three or four indicators, and 16 percent had zero to two.
Specifically:
- Seventy-one percent of community health centers can usually provide patients with same/next day appointments, or can usually provide patients with telephone advice on clinical issues during office hours or on weekends or after-hours;
- Seven in ten centers have office systems which allow them to easily generate lists of patients by diagnosis (69%) or easily track referrals until the consultation report returns to the referring provider (70%).
The more medical home characteristics a center possessed, the more likely it was to report better communication and coordination with specialty care providers and local hospitals. For example, 45 percent of centers with all of the attributes of a medical home are notified if a patient goes to the emergency room, compared with only 20 percent of centers with only a few medical homes attributes.
The survey also found that health centers with greater medical home capacity were more likely to report they have an adequate workforce and not face shortages of physicians: 43 percent of centers with all the characteristics of a medical home have an adequate physician workforce, compared to only 24 percent of centers that only have a few.
"There are real benefits when a health center functions like a medical home—better communication with other clinicians in the community, a more stable workforce, and ultimately better care for patients. These ingredients are critical for a health center to achieve high performance," said Commonwealth Fund Assistant Vice President Melinda Abrams, a co-author of the report.
Use of Health Information Technology
Forty percent of health centers use electronic medical records, which is nearly the same rate as practitioners in other settings, where 46 percent use electronic medical records. Fifty-seven percent of centers reported they electronically access patients' laboratory tests results on a routine basis and 45 percent routinely order laboratory tests electronically.
However, having more advanced health IT features, such as creating and maintaining patient registries and providing alerts or prompts to clinic staff, is variable among community health centers. For example, only 35 percent of clinics electronically prescribe medications, only 38 percent use electronic systems to issue medication alerts or prompts, and only 38 percent use computerized systems for clinical notes.
The report found that enhancing a center's use of health IT is related to better coordinated patient care. The authors state that funds specifically designated towards health IT improvement in the American Recovery and Reinvestment Act combined with new funding from the Affordable Care Act could go a long way towards helping more health centers increase their health IT capacity.
Additional Survey Findings:
-
Sixty-nine percent of centers reported that they can usually or often track ordered lab tests until the results reach clinicians. But only 46 percent indicate that their providers receive an alert or prompt to notify patients of test results.
-
25 percent of clinics can electronically determine which patients are overdue for tests or preventive care, and 18 percent usually send patients reminder notices for preventive or follow-up care.
-
Almost all centers (99%) indicate that they collect and report performance data at the provider and/or practice level in order to analyze clinical outcomes and gauge patient satisfaction.
In order to put community health centers on a long-term path to high performance, the authors recommend:
- Developing a policy to urge health centers, specialty care providers, and public hospitals to formalize referral and coordination partnerships;
- encouraging health centers to improve office systems and processes that will enable them to function as patient-centered medical homes;
- reforming payment to health centers in a way that will promote patient-centered medical homes; and
- forwarding adoption and use of health IT.
Methodology
The Commonwealth Fund 2009 Survey of Federally Qualified Health Centers was conducted by Harris Interactive Inc. from March 2, 2009 though May 27, 2009 among 795 Executive Directors or Clinical Directors at Federally Qualified Heath Centers. The survey consisted of an 8-page questionnaire that took approximately 20-25 minutes to complete; a $100 incentive for the health center was included in the original mailing. The sample was drawn from a list provided by the Bureau of Primary Health Care (BPHC) of all FQHC grantees that have at least one site that is a community based primary care clinic. A total of 1,007 FQHCs were sent the questionnaire and 795 responded, yielding a response rate of 79 percent. The data were weighted by the number of patients, number of sites, region, and urbanicity in order to more accurately reflect the universe of Primary Care Community Health Centers.


