New York, NY, January 5, 2016—Low-income adults in Kentucky and Arkansas, which both expanded Medicaid eligibility under the Affordable Care Act, were more likely to be insured and to report fewer problems paying medical bills or skipping prescriptions because of cost than adults in Texas, which did not expand coverage, according to a Commonwealth Fund-supported study released in Health Affairs today. Despite the fact that the expansion states used different methods to offer coverage to more people (traditional Medicaid in Kentucky versus private insurance in Arkansas), adults in both states saw greater increases in coverage rates and ability to afford needed health care compared to adults in the non-expansion state. 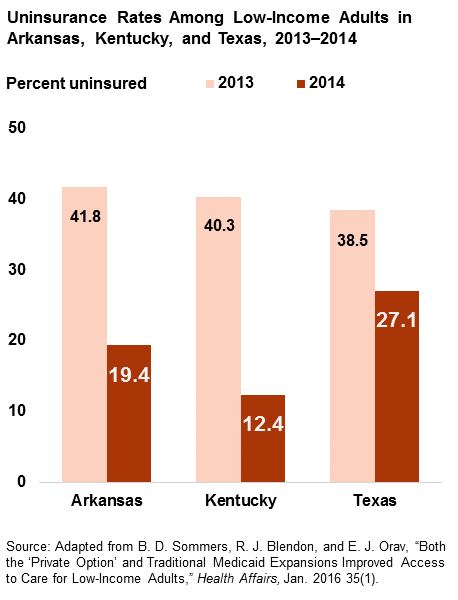
The study, conducted by Benjamin Sommers, Robert Blendon, and E. John Orav at Harvard University, compared the health care experiences of low-income adults in Kentucky, Arkansas, and Texas in late 2013 and again 12 months later. Arkansas expanded Medicaid by using federal funds to purchase private health insurance for enrollees through the ACA’s marketplaces, while Kentucky expanded eligibility through its traditional Medicaid program. Texas did not expand its Medicaid program.
The survey of more than 5,600 low-income adults found that:
- Uninsured rates dropped more in the expansion states.
- The uninsured rate in Kentucky and Arkansas dropped 14 percentage points more than it did in Texas between 2013, prior to full implementation of the ACA’s health insurance provisions, and 2014, after the expansion’s first full year.
- The uninsured rate for low-income adults was about 40 percent in all three states in 2013 but had dropped to 19 percent in Arkansas, 12 percent in Kentucky, and 27 percent in Texas in 2014.
- Fewer people reported problems with medical bills or skipping prescriptions because of cost in the expansion states.
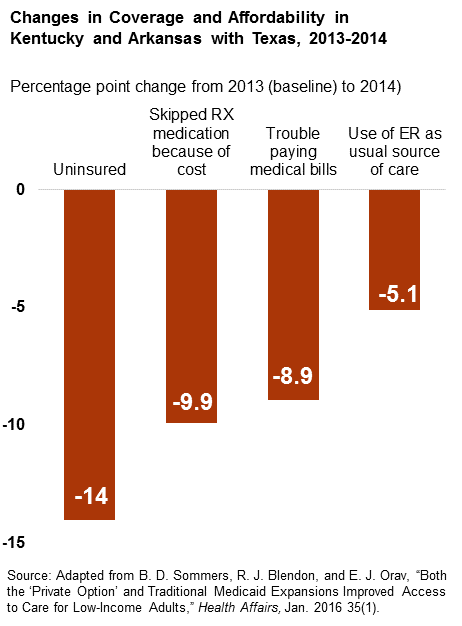
- In Kentucky and Arkansas the share of people who said they were struggling to pay medical bills fell by nearly 9 percentage points more than in Texas over 2013–2014.
- Adults reporting not filling a prescription because of the cost fell by nearly 10 percentage points more in Kentucky and Arkansas than in Texas.
- Low-income adults in Kentucky experienced an even larger reduction in problems paying medical bills than those in Arkansas, which the authors suggest indicates the greater financial protection provided by Medicaid compared to private coverage, even with subsidies.
- Care for chronic conditions improved more in the expansion states.
- In Kentucky and Arkansas, the share of adults with chronic conditions (such as high blood pressure or diabetes) who reported receiving regular care for their condition climbed by nearly 12 percentage points more than in Texas.
- Fewer people use the emergency department as their main care source in Kentucky and Arkansas.
- The share of adults reporting that the emergency room was their usual source of care fell by 5 percentage points in Kentucky and Arkansas compared to Texas.
- But demand for outpatient visits overflowed to the emergency room in the expansion states: people reporting visiting the emergency room because they couldn’t get an outpatient appointment rose nearly 5 percentage points.
“This study provides evidence that expanding Medicaid eligibility matters more than how it is expanded, on most indicators,” said Commonwealth Fund President David Blumenthal, M.D. “As states that have not yet taken steps to expand their programs weigh their options, these findings demonstrate the value of Medicaid in making health care more accessible and affordable. New approaches to expanding Medicaid should be monitored to ensure these goals are being achieved.”


