Background
Improving care for high-need, high-cost patients has long been a priority for both public and private sector purchasers of health care. In 2009, the Pacific Business Group on Health (PBGH) partnered with Boeing to implement a care management initiative that Boeing had successfully piloted with about 700 of its employees, retirees, and dependents. Called the Intensive Outpatient Care Program (IOCP),1 the initiative aims to improve outcomes for medically complex patients and prevent unnecessary hospital use by providing care coordination, self-management support, and effective ambulatory care. The overall goal of IOCP is to keep participants at home and in their communities by providing intensive, person-centered outpatient care.
Shortly after IOCP was introduced, the California Public Employees’ Retirement System (CalPERS) and Pacific Gas and Electric Company (PG&E) followed suit with a pilot in Northern California. From 2013 to 2015, PBGH, with a $19.1 million Health Care Innovation Award from the federal Centers for Medicare and Medicaid Services (CMS), expanded the IOCP model to 23 medical groups in five states.2 The grant enabled PBGH to implement IOCP in primary care practice sites in Arizona, California, Idaho, Nevada, and Washington, serving some 15,000 participants, including those enrolled in Medicare Advantage or Medicare fee-for-service, those dually eligible for Medicare and Medicaid, and a small number of Medicaid-only beneficiaries. In 2016 and 2017, PBGH has continued to provide technical assistance and training on the IOCP model to additional providers. Moreover, Boeing has incorporated aspects of the IOCP model in its accountable care organization (ACO) contracts by including specific intervention guidelines and performance guarantees for medically complex patient populations.
While the CMS grant provided an important source of funding for initial training, after the grant period ended 90 percent of participating delivery systems continued the core elements of the program for Medicare patients and 15 of 23 expanded programs into their commercial populations.
Key Program Features
The IOCP model calls for embedding dedicated care coordinators in primary care physician practices and medical groups. These care coordinators build relationships with patients and work closely with them to stabilize their health. While IOCP is similar to other models for complex patients, it is differentiated by a unique combination of elements — called the IOCP Guardrails — and close coordination with primary care providers. Participating delivery systems are expected to adhere to the Guardrails (described below), but may adapt implementation to their local environment.

IOCP Guardrails
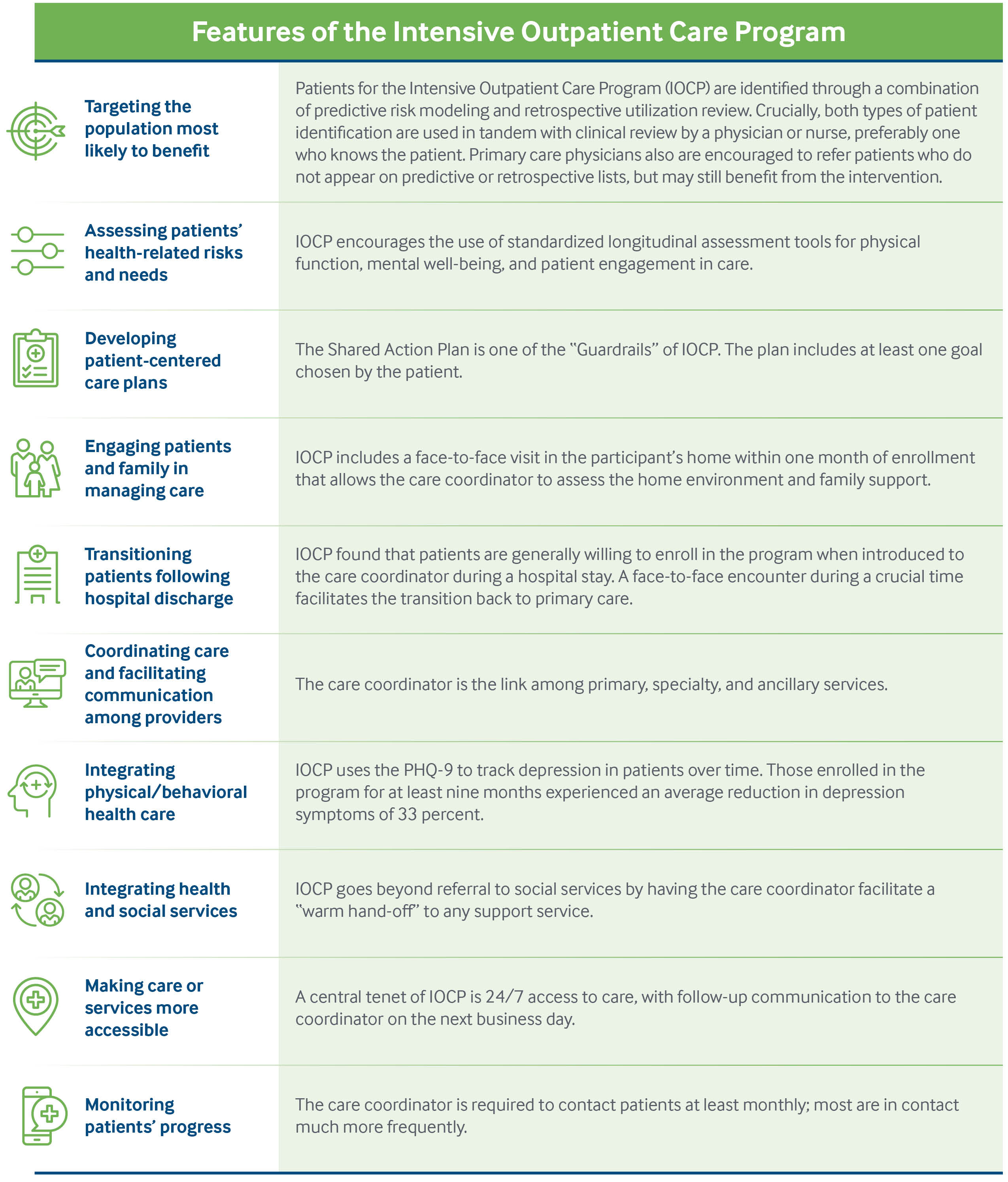
Six necessary elements have been identified as Guardrails in IOCP:
- A care coordinator (who could be a nurse, social worker, community health worker, or medical assistant), trained in person-centered care techniques, maintains a close, ongoing relationship with the participant over time and across the care continuum.
- Within one month of enrollment, the care coordinator visits the participant at home for up to 90 minutes to review the patient’s medical history, complete a needs assessment, establish treatment goals, and develop a shared action plan.
- The care coordinator and participant communicate regularly, monthly or more frequently.
- The participant and care coordinator together create a shared action plan that includes at least one goal chosen by the patient.
- In-person introductions — known as “warm hand-offs” — are made to workers from relevant support services (e.g., home health, behavioral health, transportation, drug assistance programs, food banks, and other community services).
- Patients have access to a non-emergency department care provider 24 hours a day, seven days a week, with follow-up communication to the care coordinator on the next business day.
Financing
In the initial pilot, Boeing paid participating clinicians an additional monthly fee based on the severity of the patient’s condition and the number of patients being managed. Anthem also used this model in its ACO contracts in California: Medical groups are given a higher per member, per month fee for members with more than two chronic condition diagnoses.
Funding from the CMS Innovation grant involved both a uniform infrastructure payment per medical group and a per member, per month payment. This allowed participating medical groups to hire more than 200 full-time care coordinators across approximately 600 clinical sites. The grant also funded technical assistance and training, including attendance at a three-day in-person training for care coordinators and periodic webinars on topics such as end-of-life care and motivational interviewing.
Implementing the IOCP model requires up-front investment in staff training, baseline infrastructure (e.g., electronic medical records), and delivery system capacity (e.g., after-hours access to non-emergency department care). Sustainable financing for the program is best accomplished within population-based, accountable care systems, which can offset initial outlays with long-term reductions in per member, per month spending for medically complex patients. Delivery systems that operate in traditional fee-for-service payment environments can support transformation work through per member, per month care coordination fees.
Challenges
Identifying eligible patients was an initial challenge in the CMS-funded program. Initially, it was thought that patients could be identified through Medicare fee-for-service claims data and Medicare Advantage encounter data. However, the standard risk score reports produced by the program’s third-party data vendor used data that were three to six months old, and medical groups found the data too outdated to help identify suitable IOCP patients. Medical groups devised several alternative methods for identifying patients:
- Direct referral from PCPs. Once primary care physicians (PCPs) became familiar with the program, they could refer patients who were good candidates.
- Transfer from an existing care management program. Often patients enrolled in disease-specific care management programs were identified as patients who could benefit from a more intensive, comprehensive program, like IOCP.
- Identification from hospital records. Some groups had access to hospital EHRs in integrated delivery systems and could use those data to refer patients to IOCP.
- Identification from internal reporting. Some groups had their own reporting systems or risk stratification methods that they used to identify patients for IOCP.
Recruiting patients into the program also proved initially challenging. During the first few months of program operations, care coordinators contacted eligible patients through cold calls and letters, but patients were not receptive to these approaches. Medical groups were more successful when they modified their strategies to incorporate “warm hand-offs.” This involved PCPs introducing the care coordinator during a visit or approaching eligible patients during a hospital or skilled nursing facility stay. Eventually, the warm hand-off approach was incorporated not only in patient recruitment, but in all relevant referral services.
Results
Previously released data from IOCP in commercial populations show a reduction in costs among medically complex patients by up to 20 percent.3 PBGH used several metrics to measure success in patient-reported outcomes, utilization, and cost for the CMS-funded program over the 30-month period between July 1, 2012, and December 31, 2014. The results on patient-reported health status surveys — including the Veterans Rand 12 Item Health Survey (VR12), Patient Health Questionnaire (PHQ), and Patient Activation Measure (PAM) — show statistically significant (p ≤ .05 levels) improvements in patients’ engagement in their own care and in physical and mental health. An actuarial analysis by Milliman shows reduced cost of care. Specifically, the program achieved a:
- 3.6 percent increase in patient engagement
- 33 percent reduction in depression symptoms
- 3.4 percent improvement in mental health functioning
- 4.1 percent improvement in physical health functioning
- 21 percent reduction in the cost of care for high-risk patients enrolled for at least nine months.
Lessons
The IOCP model has been successfully implemented in varied settings with different populations. This has enabled analysts to identify several common factors that contribute to the program’s success:
- strong senior leadership support, including a dedicated physician champion
- a commitment to the IOCP Guardrails
- staff who can work collaboratively in a team-based care model
- rigorous performance measurement and quality improvement processes
- modern health IT infrastructure
- in-person care coordinator training.
Next Steps
The Intensive Outpatient Care Program model continues to evolve, and the Pacific Business Group on Health is training additional providers to implement it. In 2016, elements of the IOCP model were included in technical assistance and training that PBGH led for California Medicaid providers under the Health Homes Program.4 In 2017 and 2018, with support from The SCAN Foundation, PBGH will provide training to 21 health systems providing care to 250,000 Medicare beneficiaries under its Building Care Solutions program, which builds upon the IOCP model. This work will update the model to ensure it incorporates the most recent patient-centered care principles (such as those used by the National Committee for Quality Assurance’s Patient-Centered Medical Home Recognition Program), and provide training to delivery systems on developing a business case for medically complex care programs like IOCP.



