EXECUTIVE SUMMARY
Since the Institute of Medicine's landmark reports, To Err Is Human (2000) and Crossing the Quality Chasm (2001), revealed widespread incidence of medical errors in U.S. hospitals, there has been a great deal of effort to measure and improve the quality of hospital care.1 Much progress has been made in developing quality indicators and risk-adjustment mechanisms to compare quality across institutions, and in examining practices and cultures in high-performing hospitals. Little is known, however, about the dynamics of hospital performance: the degree to which hospitals are improving (or deteriorating) over time, and how they achieve and sustain that improvement. This study examines such trends and change strategies. It combines quantitative analysis of quality and efficiency trends, using three hospital databases, with case study analysis of four hospitals that experienced significant improvement in a composite quality indicator based on risk-adjusted mortality, complication, and morbidity rates.
The quantitative analysis, led by Eugene Kroch and Michael Duan of CareScience, Inc., and described in the companion report, Hospital Performance Improvement: Trends in Quality and Efficiency, found significant improvements in mortality rates, likely indicating that hospitals have been getting better at keeping people alive through error reduction, improved technologies, adherence to evidence-based protocols, and other strategies.2 The improved mortality scores may also be attributed in part to more conscientious coding of comorbidities, and to discharging of sicker patients who may expire in home or hospice settings.
WHAT IT TAKES TO BE A "TOP IMPROVER" IN QUALITY: CASE STUDY ANALYSIS SUMMARY
Based on interviews with key informants at four hospitals that were among the top improvers (displaying significant, steady improvement in the composite quality measure from 2002–2004), we found a common temporal and ultimately cyclical sequence of factors resulting in change (Figure ES-1).3
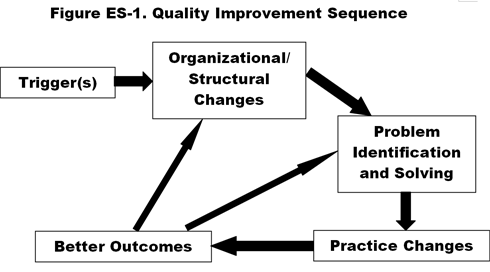
- A trigger serving as a "wake-up call" that prompts the hospital to begin or renew an emphasis on quality improvement, marking the beginning of cultural shift and leading to . . .
- organizational and structural changes such as establishment of quality-related councils and committees, empowerment of nurses and other staff, and investments in new technology and infrastructure that facilitate . . .
- a new problem-solving process, involving a standardized, systematic, multidisciplinary team approach to identify and study a problem area, conduct root cause analysis, develop action plans, and hold team leaders accountable, resulting in establishment of . . .
- new protocols and practices, including evidence-based policies and procedures, clinical pathways and guidelines, error-reducing software, and patient flow management techniques, leading to . . .
- improved outcomes in process and health-related measures (e.g., patient flow, errors, complications, mortality), satisfaction and work environment, and "bottom line" indicators such as reduced length of stay and increased market share. Experiencing such positive results then served as motivation to hospital staff to expand their efforts, thus turning the above sequence into a self-sustaining cycle. That is, the improved outcomes led to further impetus to change, accelerated change, and a spreading of the "change culture" to other parts of the institution. This entire sequence reflects the establishment, growth, and reinforcement of a culture of quality.
"Trigger" Situations or Events
All four hospitals cited negative or positive trigger events that motivated a new emphasis on quality, including:
- a series of medical errors with tragic results, which were reported in the media;
- arrival of a new CEO with a strong interest in patient service and quality;
- noticeable increases in length of stay and readmissions for certain conditions;
- significant loss in market share for certain services that led to dissatisfaction among staff and patients;
- new evidence and awareness of the potential for hospitalists and intensivists to promote multidisciplinary care, based on a growing body of literature indicating their ability to coordinate care, leading to improved outcomes;4 and
- the Institute of Medicine report, To Err Is Human, that provided clear evidence of widespread medical errors in hospitals nationwide.
A few hospitals mentioned that changes to payment (e.g., pay-for-performance incentives, reimbursement adjustments) as well as assistance from quality improvement organizations (QIOs) served as incentives to improve quality in the period after study (2002–2004). Such factors could potentially act as triggers for hospitals in the future.
Organizational and Structural Changes
After the trigger events, the hospitals made organizational changes that both reflected and nurtured a "culture of quality." They also created structures and processes to monitor performance, identify deficiencies, and devise, test, and implement solutions. The organizational changes included:
- creating or reenergizing councils, committees, or commissions responsible for monitoring and ensuring success of quality improvement efforts;/li>
- elevating the role of the quality improvement and performance departments and providing them with sufficient resources (including increasing budgets for quality activities beyond one-time capital expenditures);
- instituting policies that encouraged staff to express concerns, identify deficiencies, and challenge the status quo such as nurse empowerment programs (along with granting nurses greater autonomy), anonymous reporting systems, CEO "open door" policies, and staff-wide open discussions on topics of concern;
- creating multidisciplinary teams to provide patient care and/or address deficiencies made up of staff who can best devise, test, and implement solutions and are held accountable for success;
- establishing or expanding hospitalist and intensivist programs to improve care coordination and access to physician services for inpatients;
- nurturing physician and nurse champions to take the lead in developing protocols to address deficiencies and to encourage and educate their peers on new practices and procedures;
- using public performance reports as opportunities to identify deficiencies and improve care, health outcomes, and patient satisfaction (the Joint Commission on Accreditation of Healthcare Organizations' Core Measures were uniformly deemed extremely valuable);
- reporting to Boards of Directors and parent health systems that closely monitor and set quality-related goals; and
- acquiring executives who communicate a culture of quality through personal example, supportive policies, and investment of resources (e.g., state-of-the-art diagnostic equipment, health information technology, and quality improvement staff).
Protocol and Practice Changes
As structural and organizational changes established standardized, systematic processes for problem-solving, hospitals were able to test and implement major practice changes. Examples include:
- clinical guidelines, protocols, or "care maps" for specific conditions or procedures;
- department-specific quality plans, with short- and long-term goals;
- improved educational and training materials for clinical staff on error reduction, hand-washing, and infection prevention;
- strategies for reducing need for patient restraints;
- educational materials for patients regarding fall prevention; and
- information technology that reduced medication errors and improved data collection.
Improved Outcomes
The practice changes appear to have resulted in improved outcomes for patients and the institutions themselves. In addition to major improvements in the combination quality measure (based on mortality, morbidity, and complication rates), interviewees cited the following examples of improvements:
- process/operations: faster receipt of test results, faster patient flow, easier and more efficient data sharing and recording, fewer medication errors;
- health-related: reductions in mortality, blood infections, pneumonia, complications, readmissions, patient falls, and use of or need for restraints;
- work environment and reputation: increases in patient satisfaction and staff satisfaction/morale, improved status in community, greater ability to attract quality;
- staff and physicians; and
- bottom line: decreased costs per hospitalization and length of stay for certain conditions and increased admissions and/or market share.
These positive outcomes motivated staff and hospital leaders to strengthen their efforts and in this way reinforced the quality improvement process.
CHALLENGES AND LESSONS LEARNED
Change does not happen easily, as these hospitals learned. Further, the amount of time after changes were made before meaningful results were seen varied considerably within each of the hospitals, depending on the nature of the change and the rate of acceptance and adoption by staff. The hospitals studied struggled with:
- resistance to change in culture and specific protocols from physicians and nurses;
- limited resources available to make or maintain quality-related investments; and
- complacency with past improvements.
Lessons from the four hospitals' experiences that could assist other hospitals trying to establish a culture of quality include the following:
- set short-term, attainable goals and celebrate successes (and the individuals involved) in reaching them;
- keep the staff involved in problem identification and problem-solving, valuing everyone's experiences and encouraging as well expecting all to participate;
- nurture dedicated leaders and champions who encourage and "bring along"
their peers; - be patient but unrelenting, recognizing that change takes time and continuing to keep quality improvement "on the front burner"; and
- balance quality and financial goals, considering investments in quality improvement from a short- and long-term perspective.
HOW CAN PUBLIC POLICY HELP?
Representatives of the four hospitals suggested the following potential roles for public policy in facilitating quality improvement efforts:
- standardize reporting requirements;
- ensure accuracy and clarity of public reporting;
- educate consumers in interpreting information and using it appropriately;
- supporting pay-for-performance (P4P) programs that use "carrots" (rewards)
rather than "sticks" (penalties); - offer incentives such as tax credits to providers who participate in P4P programs; and
- continue to document and publicize quality issues.
Table ES- 1 summarizes this improvement process at the four case study hospitals.
Table ES-1. Summary of Case Study Sites and Their Improvement Processes | ||||
| Organization/ Setting | Trigger | Organizational/ Structural Changes | Examples of Practice Changes (processes, procedures) | Results (examples) |
Beth Israel Medical Center, New York, N.Y. Very large, 1,080-bed teaching hospital in urban setting, part of a five-hospital not-for-profit system |
|
|
|
|
Legacy Good Samaritan Hospital, Portland, Ore. Large 539-bed hospital in an urban setting, part of a six-hospital system |
|
|
|
|
Rankin Medical Center, Brandon, Miss. Small 90 (active acute care) bed community hospital serving rural and suburban counties, part of a 65-hospital for-profit system |
|
|
|
|
St. Mary's Health Care System, Athens, Ga. Small 165-bed suburban hospital, part of 33-hospital Catholic Hospital system |
|
|
|
|
1Institute of Medicine, Committee on Quality of Health Care in America, To Err Is Human: Building a Safer Health System (Washington, D.C.: National Academies Press, 2000); and Crossing the Quality Chasm: A New Health System for the 21st Century (Washington, D.C.: National Academies Press, 2001).
2E. Kroch, M. Duan, S. Silow-Carroll, and J. Meyer, Hospital Performance Improvement: Trends in Quality and Efficiency (New York: The Commonwealth Fund, Apr. 2007); available at http://www.commonwealthfund.org/publications/publications_show.htm?doc_id=471264.
3Unlike the companion report that focuses on both quality and efficiency trends, the case study hospitals featured in this report were selected based on improvement in quality measures, although we excluded hospitals that displayed declining efficiency over the period examined.4The National Association of Inpatient Physicians defines hospitalists as "physicians whose primary professional focus is the general medical care of hospitalized patients." Their activities include patient care, teaching and research, and leadership related to hospital care. An intensivist
is a hospitalist who specializes in the care of critically ill patients, usually in an intensive care unit.


