Every family wants the best care for an ill or injured family member. Most are grateful for the care and attention received. Yet, evidence in the National Scorecard on U.S. Health System Performance, 2008, shows that care typically falls far short of what is achievable. Quality of care is highly variable, and opportunities are routinely missed to prevent disease, disability, hospitalization, and mortality. Across 37 indicators of performance, the U.S. achieves an overall score of 65 out of a possible 100 when comparing national averages with benchmarks of best performance achieved internationally and within the United States.
Even more troubling, the U.S. health system is on the wrong track. Overall, performance has not improved since the first National Scorecard was issued in 2006. Of greatest concern, access to health care has significantly declined. As of 2007, more than 75 million adults—42 percent of all adults ages 19 to 64—were either uninsured during the year or underinsured, up from 35 percent in 2003. At the same time, the U.S. failed to keep pace with gains in health outcomes achieved by the leading countries. The U.S. now ranks last out of 19 countries on a measure of mortality amenable to medical care, falling from 15th as other countries raised the bar on performance. Up to 101,000 fewer people would die prematurely if the U.S. could achieve leading, benchmark country rates.
The exception to this overall trend occurred for quality metrics that have been the focus of national campaigns or public reporting. For example, a key patient safety measure—hospital standardized mortality ratios (HSMRs)—improved by 19 percent from 2000–2002 to 2004–2006. This sustained improvement followed widespread availability of risk-adjusted measures coupled with several high-profile local and national programs to improve hospital safety and reduce mortality. Hospitals are showing measurable improvement on basic treatment guidelines for which data are collected and reported nationally on federal Web sites. Rates of control of two common chronic conditions, diabetes and high blood pressure, have also improved significantly. These measures are publicly reported by health plans, and physician groups are increasingly rewarded for results in improving treatment of these conditions.
The U.S. spends twice per capita what other major industrialized countries spend on health care, and costs continue to rise faster than income. We are headed toward $1 of every $5 of national income going toward health care. We should expect a better return on this investment.
Performance on measures of health system efficiency remains especially low, with the U.S. scoring 53 out of 100 on measures gauging inappropriate, wasteful, or fragmented care; avoidable hospitalizations; variation in quality and costs; administrative costs; and use of information technology. Lowering insurance administrative costs alone could save up to $100 billion a year at the lowest country rates.
National leadership is urgently needed to yield greater value for the resources devoted to health care.
The National Scorecard
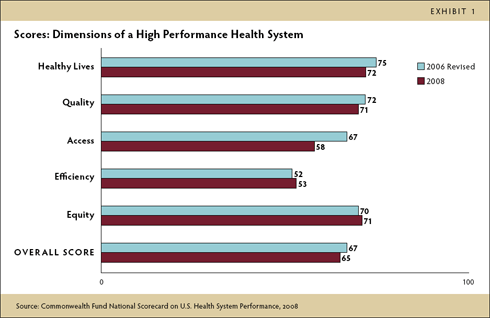
The National Scorecard includes 37 indicators in five dimensions of health system performance: healthy lives, quality, access, efficiency, and equity. U.S. average performance is compared with benchmarks drawn from the top 10 percent of U.S. states, regions, health plans, hospitals, or other providers or top-performing countries, with a maximum possible score of 100. If average U.S. performance came close to the top rates achieved at home or internationally, then average scores would approach 100.
In 2008, the U.S. as a whole scored only 65, compared with a score of 67 in 2006—well below the achievable benchmarks. Average scores on each of the five dimensions ranged from a low of 53 for efficiency to 72 for healthy lives.
On those indicators for which trend data exist, performance compared with benchmarks more often worsened than improved, primarily because of declines in national rates between the 2006 and 2008 Scorecards. Overall, national scores declined for 41 percent of indicators, while one-third (35%) improved, and the rest exhibited no change (or were not updated). Exhibit 2 lists indicators and summarizes scores and benchmark rates.
As observed in the first Scorecard, the bottom group of hospitals, health plans, or geographic regions is often well behind even average rates, with as much as a fivefold spread between top and bottom rates. On key indicators, a 50 percent improvement or more would be required to achieve benchmark levels.
Scorecard Highlights and Key Findings
The U.S. continues to perform far below what is achievable, with wide gaps between average and benchmark performance across dimensions. Despite some encouraging pockets of improvement, the country as a whole has failed to keep pace with levels of performance attained by leading nations, delivery systems, states, and regions. Following are major highlights from the Scorecard by performance dimension:
Healthy Lives: Average Score 72
- Preventable mortality: The U.S. fell to last place among 19 industrialized nations on mortality amenable to health care—deaths that might have been prevented with timely and effective care. Although the U.S. rate improved by 4 percent between 1997–1998 and 2002–2003 (from 115 to 110 deaths per 100,000), rates improved by 16 percent on average in other nations, leaving the U.S. further behind.
- Activity limitations: More than one of every six working-age adults (18%) reported being unable to work or carry out everyday activities because of health problems in 2006—up from 15 percent in 2004. This increase points to the need for better prevention and management of chronic diseases to enhance quality of life and capacity to work, especially among younger adults as they age.
Quality: Average Score 71
- Effective care: Control of diabetes and high blood pressure improved markedly from 1999–2000 to 2003–2004 for adults, according to physical exams conducted on a nationally representative sample. Among adults with diabetes, rates of at least fair control of blood sugar increased from 79 percent to 88 percent from 1999–2000 to 2003–2004. Among adults with hypertension, rates of control of high blood pressure increased from 31 percent to 41 percent over the same time period. Yet, a 30 to 60 percentage point difference remains between top- and bottom performing health plans. Hospitals' adherence to treatment standards for heart attack, heart failure, and pneumonia also improved from 2004 to 2006, but with a persistent gap between leading and lagging hospital groups. Delivery rates for basic preventive care failed to improve: as of 2005, only half of adults received all recommended preventive care.
- Coordinated care: Heart failure patients were more likely to receive hospital discharge instructions in 2006 (68%) than in 2004 (50%), but rates varied widely between top and bottom hospital groups (from 94% to 36%). Hospitalizations increased among nursing home residents from 2000 to 2004, as did rehospitalizations for patients discharged to skilled nursing facilities—signaling a need to improve long-term care and transitions between health care providers.
- Safe care: One key indicator of patient safety—hospital standardized mortality ratios—improved significantly since the first Scorecard, with a 19 percent decline. Safety risks, however, remain high as one-third of adults with health problems reported mistakes in their care in 2007. Drug safety is of particular concern. Rates of visits to physicians or emergency departments for adverse drug effects increased by one-third between 2001 and 2004.
- Patient-centered, timely care: In 2007, as in 2005, less than half of U.S. adults with health problems were able to get a rapid appointment with a physician when they were sick. They also were the most likely among adults in seven countries surveyed to report difficulty obtaining health care after hours without going to the emergency department, and this rate increased from 61 percent to 73 percent since 2005. Within the U.S., there is wide variation among hospitals in terms of patient reports of how well staff responded to their needs.
Access: Average Score 58
- Insurance and access: As of 2007, 75 million working-age adults (42%) were either uninsured or underinsured, a sharp increase from 61 million (35%) in 2003. More than one-third (37%) of all U.S. adults reported going without needed care because of costs in 2007, versus only 5 percent in the benchmark country.
- Affordable care: As insurance premiums rose faster than wages, the share of nonelderly adults living in a state where group health insurance premiums averaged less than 15 percent of household income dropped sharply, from 58 percent in 2003 to 25 percent in 2005. By 2007, two of five adults (41%) reported they had medical debt or problems with medical bills, up from 34 percent in 2005.
Efficiency: Average Score 53
- Inappropriate, wasteful, or fragmented care: In 2007, as in 2005, U.S. patients were much more likely—three to four times the benchmark rate—than patients in other countries to report having had duplicate tests or that medical records or test results were not available at the time of their appointment.
- Avoidable hospitalizations: Average rates of hospital readmissions within 30 days remained high, at 18 percent in both 2003 and 2005. Rates in the highest regions were 50 percent higher than in the lowest regions. Rates of hospitalizations for preventable conditions decreased somewhat from 2002–2003 to 2004–2005, but continued to vary two- to fourfold across hospital regions and states.
- Variation in quality and costs: Among Medicare patients treated for heart attacks, hip fractures, or colon cancer, a high proportion of regions with the lowest mortality rates also had lower total costs, indicating that it is possible to save lives and lower costs through more effective, efficient systems. The total costs of caring for patients with chronic disease varied twofold across regions.
- Administrative costs: U.S. health insurance administrative costs as a share of total health spending are 30 percent to 70 percent higher than in countries with mixed private/public insurance systems and three times higher than in countries with the lowest rates.
- Information systems: U.S. primary care physicians' use of electronic medical records (EMRs) increased from 17 percent to 28 percent from 2001 to 2006. Still, the U.S. lags far behind leading countries, where EMRs are now used by nearly all physicians (98%) to improve care.
Equity: Average Score 71
- Disparities: Compared with their white, higher-income, or insured counterparts, minorities, low-income, or uninsured adults and children were generally more likely to wait when sick, to encounter delays and poorly coordinated care, and to have untreated dental caries, uncontrolled chronic disease, avoidable hospitalizations, and worse outcomes. They were also less likely to receive preventive care or have an accessible source of primary care.
- Reducing gaps: Among blacks and Hispanics, it would require a 19 percent to 25 percent decrease in the risk of poor health outcomes and inadequate or inefficient care to reach parity with whites. Gaps for uninsured and low-income populations are still wider: it would require a 34 percent to 39 percent improvement on indicators of health care access, quality, and efficiency to achieve equity with insured and higher-income populations.
System Capacity to Innovate and Improve: Not Scored
The capacity to innovate and improve is fundamental to a high-performing health care system. It includes:
- a care system that supports a skilled and motivated health care workforce, with an emphasis on primary care and population health;
- a culture of quality improvement and continuous learning that promotes and rewards recognition of opportunities to reduce errors and improve outcomes; and
- investment in public health initiatives, research, and information necessary to inform, guide, and drive health care decisions and improvement.
On all three aspects, the U.S. currently under-invests in the capacity of the health system to innovate and improve. U.S. payment systems undervalue primary care and fail to support providers' efforts to manage and coordinate care. Studies indicate that health care teams and well-organized work processes can achieve significant gains in quality and safety with more efficient use of resources. Yet, health professionals are rarely trained to work in teams, and larger organized delivery systems that employ multidisciplinary health professionals are not the norm. There is little investment in spreading best practices, and incentives are rarely designed to reward or support improved quality and greater efficiency. In an era of rapid medical advances, national investment in research regarding clinical and cost-effectiveness—what works well for which patients and when—has failed to keep pace to inform health care decision-making.
Summary and Implications
Potential for Improvement
Overall, the National Scorecard on U.S. Health System Performance, 2008, finds that the U.S. is losing ground in providing access to care and has uneven health care quality. The Scorecard also finds broad evidence of inefficient and inequitable care. Average U.S. performance would have to improve by more than 50 percent across multiple indicators to reach benchmark levels of performance.
Closing performance gaps would bring real benefits in terms of health, patient experiences, and savings. For example:
- Up to 101,000 fewer people would die prematurely each year from causes amenable to health care if the U.S. achieved the lower mortality rates of leading countries.
- Thirty-seven million more adults would have an accessible primary care provider, and 70 million more adults would receive all recommended preventive care.
- The Medicare program could potentially save at least $12 billion a year by reducing readmissions or by reducing hospitalizations for preventable conditions.
- Reducing health insurance administrative costs to the average level of countries with mixed private/public insurance systems (Germany, the Netherlands, and Switzerland) would free up $51 billion, or more than half the cost of providing comprehensive coverage to all the uninsured in the U.S. Reaching benchmarks of the best countries would save an estimated $102 billion per year.
Studies further document the cost in lives and lost productivity from the nation's failure to provide secure health insurance to all. Based on areas within the U.S. that achieve superior outcomes at lower costs, it should be possible to close gaps in health care quality and access, and to reduce costs significantly.
Several implications for policy emerge from the Scorecard findings:
What Receives Attention Gets Improved
Notably, all of the quality indicators showing significant improvement have been targets of national and collaborative efforts to improve, informed by data with measurable benchmarks and indicators reached by consensus. Conversely, there was failure to improve in areas such as mental health care, primary care, hospital readmission rates, or adverse drug events for which focused efforts to assess and improve at the community or facility level are lacking. Further, the continued failure to adopt interoperable health information technology makes it difficult to generate the information necessary to document performance and monitor improvement efforts.
Better Primary Care and Care Coordination Hold Potential for Improved Outcomes at Lower Costs
Hospital readmission rates and rates of potentially preventable hospitalizations for ambulatory care-sensitive conditions remain high and variable across the country, as do total costs for the chronically ill. Studies indicate that it is possible to prevent hospitalization or rehospitalizations with better primary care, discharge planning, and follow-up care—an integrated, systems approach to care.
Multiple indicators highlight the fact that the U.S. has a weak primary care foundation. Investing in primary care with enhanced capacity to provide patients with round-the-clock access, manage chronic conditions, and coordinate care will be key steps in moving to more organized care systems.
However, current payment incentives for hospitals, physicians, and nursing homes do not support coordination of care or efficient use of expensive, specialized care. information also fails to flow with patients across sites of care due to lack of health information technology and information exchange systems. These inefficiencies require innovative payment policies as well as care delivery approaches to improve outcomes for patients and use resources more efficiently.
Aiming Higher
The 2008 National Scorecard documents the human and economic costs of failing to address the problems in our health system. Recent analysis suggests it could be possible to insure everyone and achieve significant savings with improved value over the next decade. Health care expenditures are projected to double to $4 trillion, or 20 percent of national income, over the next decade, and millions more U.S. residents are on a path to becoming uninsured or underinsured, absent new policies. We need to change directions, starting with the recognition that access to care, health care quality, and efficiency are interrelated.
Aiming higher and moving on a more positive path will require strategies targeting the multiple sources of poor health system performance. These strategies include:
- universal and well-designed
- coverage that ensures affordable access and continuity of care, with low administrative costs;
- incentives aligned to promote higher quality and more efficient care;
- care that is designed and organized around the patient, not providers or insurers;
- widespread implementation of health information technology with information exchange;
- explicit national goals to meet and exceed benchmarks and monitor performance; and
- national policies that promote private-public collaboration and high performance.
Rising costs put families, businesses, and public budgets under stress, pulling down living standards for middle- as well as low-income families. New national policies that take a coherent, whole-system, population view are essential for the nation's future health and economic security.