Care coordination is described in a Commonwealth Fund report as one of seven elements needed to organize care around patients. The Institute of Medicine has explicitly stated that care coordination is needed to improve the quality of health care in the United States. Yet there is a lack of consensus regarding care coordination’s competencies and core functions, who should provide them, the desired outcomes, and how to measure and pay for these services.
This report proposes a framework for pediatric care coordination. It includes a definition of care coordination; outlines its principal characteristics, competencies, and functions; and sets forth a detailed process for its delivery. It also describes a model to implement care coordination across all health care settings and related disciplines.
We employed multiple strategies to develop this framework, including a literature review and consultation with key informants representing families, public and commercial payers, pediatric nurses, pediatric and geriatric social workers, pediatric health care providers, and federal partners including the Maternal and Child Health Bureau and the Agency for Healthcare Research and Quality.
The proposed framework takes a family-centered approach and a health systems view with attention to interdisciplinary and environmental structures, processes, and outcomes (Figure 1). Effective care coordination is best provided in the context of a health care team, real or virtual, that has established working relationships with families, clinicians, community partners, and other professionals.
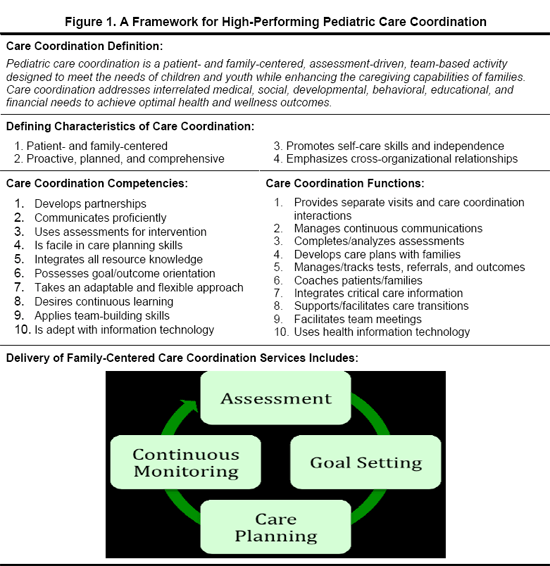
We conclude that an integrated care coordination infrastructure is essential to create and sustain a high performance pediatric health care system. The success of this process will depend on multiple factors at all levels within the health care system and across multiple sectors of the community. Supporting this transformation will be the development of performance and outcome measures, as well as mechanisms for workforce development, education, policy support, and financing.
It is critical to note that the scope of services for care coordination for children and youth is markedly different from the scope of such services for typical adult populations. With the exception of geriatric services, care coordination for many adults is essentially management of chronic health conditions. While both adult and pediatric health care must focus on chronic conditions, care coordination that supports the comprehensive needs of children, youth, and families must be broader than this strictly medical view.
The effectiveness of a care coordination system can be measured by the experiences of the families that receive these services. Therefore, families must play a proactive role in informing the design of the infrastructure and policies that will support the development of care coordination as an integral part of the health care system.


