Executive Summary
Health spending as a share of U.S. gross domestic product (GDP) has climbed steadily over the past half-century. Today, it constitutes 18 percent of GDP, up from 14 percent in 2000 and 5 percent in 1960, and we are well on our way to 21 percent by 2023, based on current projections. This increased dedication of economic resources to the health sector, however, is not yielding commensurate value in terms of improving population health or patients’ experiences with care.
On average, the U.S. spends twice as much on health care per capita, and 50 percent more as a share of GDP, as other industrialized nations do. And yet we fail to reap the benefits of longer lives, lower infant mortality, universal access, and quality of care realized by many other high-income countries. There is broad evidence, as well, that much of that excess spending is wasteful. Stabilizing health spending and targeting it in ways that ensure access to care and improve health outcomes would free up billions of dollars annually for critically needed economic and social investments—both public and private—as well as higher wages for workers.
In this report, The Commonwealth Fund Commission on a High Performance Health System endorses the goal of holding future growth in total health spending to a rate no greater than that of long-term growth in GDP, while simultaneously moving toward a high performance health care system. This is an ambitious goal, to be sure, particularly given our aging population and the commitment to access for all. But with such a high proportion of our economic resources already devoted to health care, and with abundant evidence that we can do better, such a target should be achievable. It is also a key to enabling broader economic growth and a more affordable health care system for businesses, families, and federal, state, and local governments. 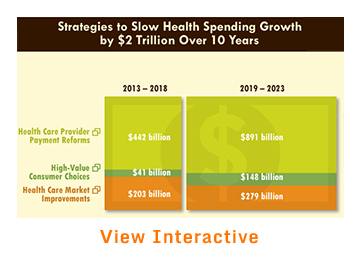
The policies described below should produce substantial reductions in health spending. But if spending growth targets are not met, further action should be taken to address areas in which spending growth is excessive. This should include more aggressive implementation of those policies, focusing particularly on both geographic areas and types of services that are found to be drivers of excessive spending and spending growth. The establishment of targets, then, can serve both as a metric to guide policy development and as an incentive for all involved parties to act to make them effective.
To show how future health spending growth could be held to a national target and stabilized while moving toward a high performance health care system, this report lays out a synergistic strategy relying on three broad thrusts:
- Provider payment reforms to promote value and accelerate health care delivery system innovation.
- Policies to expand options and encourage high-value choices by consumers armed with better information about the quality and cost of care.
- Systemwide action to improve how health care markets function, including reducing administrative costs and setting national and regional targets for spending growth.
The set of policies the Commission has identified in these three areas would interact with each other in mutually supportive ways to address market forces that contribute to high and rising costs but are failing to produce value. By applying these policies collectively—with the public and private sectors working in concert—the nation would be able to benefit from their synergy. Analysis of specific policies consistent with these approaches indicates that they could slow growth in national spending by a cumulative $2 trillion through 2023. Achieving these potential savings depends on starting now and acting together.
Strategic Approach
This report translates these three broad thrusts into 10 policies to illustrate our comprehensive approach to stabilizing spending growth. The policies reinforce each other to address concerns about both public and private health care costs while also improving health outcomes and patients’ care experiences.
Provider Payment Reforms to Promote Value and Accelerate Delivery System Innovation: Create incentives to coordinate care, lower costs, and improve outcomes.
- Revise Medicare physician fees and methods of updating payment so that we pay for value. Replace Medicare’s current system for determining physician fees (and the resulting reductions called for under current law) by holding fees constant at their current level, while adjusting relative payment rates for services that meet specified criteria as "overpriced." Provide increases in future payments only for providers that participate in payment and delivery system innovations that are accountable for the populations they serve. Institute competitive bidding for medical commodities such as drugs, equipment, and supplies.
- Strengthen primary care and support care teams for high-cost, complex patients. Promote patient-centeredness and better outcomes by changing payment for primary care to reward care management, coordination, and a team-based, systemic approach to treating patients who are covered by Medicare, Medicaid, other public programs, and by private plans participating in the new health insurance exchanges.
- Bundle hospital payments to focus on total costs and patient outcomes. Accelerate the implementation of provider reimbursement approaches in which a single payment is made for all services provided during an episode of care involving a hospital stay, including postacute services for specified procedures and conditions, for patients in Medicare, Medicaid, other public programs, and private plans participating in the new health insurance exchanges.
- Adopt payment reforms across markets, with public and private payers working in concert. Align payment incentives across public and private payers to enable and support care systems that are more accountable for providing high-value care. Require private plans participating in health insurance exchanges to incorporate alternative payment approaches to support delivery system innovation, such as payment for primary care medical homes, care teams, bundled payment for episodes involving hospital care, and shared savings or global payment arrangements with networks of providers. Encourage private insurance plans in each state to negotiate health care prices that are consistent with value and efficiency—and not just pass on higher prices to consumers.
Policies to Expand Options and Encourage High-Value Choices by Consumers: Create incentives for consumers to choose high-value care and high-performing care systems based on comparative information about quality and costs.
- Offer Medicare beneficiaries a new "Medicare Essential" plan that provides more comprehensive benefits and better protection against catastrophic costs and includes provider and enrollee incentives to achieve better care, better health, and lower costs. Develop a value-based benefit design that encourages beneficiaries to obtain care from high-performing care systems. These incentives would be aligned with payment reforms that give providers incentives to develop and join innovative care systems that improve patient outcomes and care experiences.
- Provide positive incentives for Medicare and Medicaid beneficiaries to seek care from high-value, patient-centered medical homes, care teams, accountable care organizations, and integrated delivery systems. Work with local employer coalitions to spread the same value-based approach, with positive incentives for patients in private plans.
- Enhance information on clinical outcomes of care and patient experiences to inform treatment decisions and choices of providers and care systems. Accelerate the "meaningful use" of health information technology to assess and compare clinical outcomes over time from alternative treatment choices and, through use of patient registries, to enable post-marketing surveillance of safety and care outcomes. Provide consumers and clinicians with transparent information on costs and prices to further inform choices.
Systemwide Action to Improve How Health Care Markets Function: Reduce administrative costs, reform malpractice policy, and set targets for total spending growth nationally and at other geographic levels.
- Simplify and unify administrative policies and procedures across public and private health plans to reduce provider and plan administrative costs and complexity.
- Reform medical malpractice policy and link to payment in order to provide fair compensation for injury while promoting patient safety and adoption of best practices.
- Establish spending targets. Target total combined public and private spending to grow at a rate no greater than economic growth per capita. Set targets for the nation (long-term GDP growth per capita), as well as for states, regions, or localities, and adjust policies as appropriate based on progress in meeting targets. Collect data to inform and enable state and local action to develop focused policies if growth exceeds targets.
Setting a target for overall spending growth—across all payers, public and private, and across all providers in all areas—of no greater than economic growth per capita would provide guidance for these policies and any further policy action that is needed. Collecting data on total spending and sources of spending growth at the national, state, and local levels would enable state and local governments to set their own targets and develop focused policies to meet them.
More consistent payment approaches across payers also could help counteract the concentration of market power among providers. Allowing multiple payers to negotiate jointly to employ similar payment methods and more consistent pricing under state or federal government auspices and aligning payment with efficient care and value, rather than simply passing on higher prices in consolidated markets, could lower private insurance premium costs for businesses and families. Joint negotiations among health care purchasers would need to take place under public auspices to ensure accountability.
Over time, the policies described in this report should generate evolutionary forces that lead to the formation of health care delivery organizations that are held accountable for the costs of care as well as health outcomes and care experiences. By assessing system performance continually relative to the spending target, flexible policies could be calibrated to address areas in which there is excessive cost growth.
Synergistic Policies
Our synergistic approach is intended to build on the substantial movement already afoot to improve health system performance. The policies would interact to accelerate and focus that momentum to achieve the goals of better health, better health care experiences, and lower costs.1
The need for action applies not only to the federal government, but also to state and local governments, businesses, and households—all of which are under increasing financial pressure from rapid health spending growth. The overarching goal should be moving the U.S. health system toward a higher level of performance, one marked by access to affordable care for all, improved quality and patient-centeredness, greater accountability for both health outcomes and treatment costs, and enhanced population health. A high performance health system is not only consistent with stability in health care spending, it is essential for it.
To examine the potential of our proposed synergistic policies, The Commonwealth Fund contracted with Actuarial Research Corporation (ARC) to estimate the cumulative impact on health care spending by 2023 if an illustrative set of policies were to take effect in 2014, assuming the policies are enacted in 2013. The analysis examined the net impact on spending by the federal government, state and local governments, private employers, and households as well as total health spending.2
The estimates suggest the policies consistent with the strategic approach could reduce projected health spending by a cumulative $2.004 trillion over the first 10 years (2014–2023). The savings would accrue to the federal government ($1.036 trillion), state and local governments ($242 billion), employers ($189 billion), and households ($537 billion).
For the federal government, the analysis indicates net savings well beyond the level necessary to offset the 10-year costs of replacing current Medicare policies that call for steep cuts in payments to physicians under the sustainable growth rate (SGR) formula. By instituting broader Medicare payment reforms and ensuring these spread to Medicaid as well, the pace of delivery system reform would be accelerated without resorting to across-the-board reductions in provider payments and would produce substantial net savings for federal programs. Targeted policies to lower administrative costs for providers could furthermore support growth in clinician incomes.
U.S. households would be the major winners over time from the strategic approach we describe here, with the potential for better care and health outcomes as well as an estimated $537 billion in direct savings over 10 years. These savings result from lower future insurance premium and out-of-pocket costs resulting from more efficient insurance markets serving Medicare beneficiaries, and from slower growth in the underlying costs of care as the delivery system responds to new incentives for enhanced, high-value care and care systems. In the end, reduced health spending by federal, state, and local governments and private employers also would accrue to households, which ultimately bear the burden of health spending through higher taxes, reduced wages, and direct out-of-pocket costs.
It is important to note that, even with these savings, the health sector would continue to grow. This growth would provide resources to innovate and develop new medical breakthroughs, as well as allow us to meet the needs of an aging population.
Notably, the bulk of the estimated $2 trillion in savings comes from pay-for-value reforms that accelerate delivery system innovation and from lowering insurance-related administrative costs by simplifying and standardizing reporting and other policies. Administrative simplification savings would largely accrue to providers, freeing up physicians and their staff to spend more time on patient care.
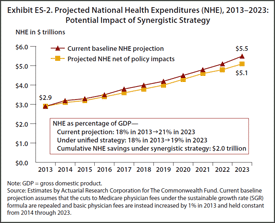
The analysis indicates that such a comprehensive and synergistic approach, with all payers pulling together in the same direction, would stabilize health care spending and bring it more in line with growth of the economy. The percentage of GDP spent on health care by 2023 would be an estimated 19 percent—similar to the 18 percent projected in 2013 (before the policies begin to take effect) and considerably lower than the 21 percent projected under current law.
The growth in Medicare spending per beneficiary would be below GDP growth for most of the decade, with substantial net savings compared with current projections. In contrast with Medicare, however, although private spending per enrollee would slow, it would continue to exceed GDP growth as it has in recent years. If focused policies at the local, state, regional, or national level slowed private per-person spending growth to bring it more in line with economic growth, the estimates indicate that national health expenditures (NHE) as a share of GDP by 2023 would be near the 2013 level.
Spending growth targets and data for assessing change will be instrumental to inform future action. At the state or local market level, it will be particularly important to have reliable information on baseline total spending and trends so that policies can be developed as needed, since patterns would likely vary in different parts of the country. Policies could be adjusted over time to achieve targets by the end of the decade.
To get these results, it will be necessary to act quickly and for major payers to pull together with a sense of urgency. The net impact of these policies accelerates over time as the health care delivery system and markets respond to new incentives and as the policies spread across the public and private sectors.
The Commonwealth Fund Commission on a High Performance Health System offers this synergistic set of policies as a way forward for federal and state policymakers and private-sector health care leaders confronting escalating health care costs. We also offer criteria to guide national discussions related to the federal deficit and federal health programs. Building on the three pillars of payment reform, high-value choices, and other market reforms, the United States has the potential to accelerate health care innovation while ensuring access for all.
1 D. Berwick, T. Nolan, and J. Whittington, "The Triple Aim: Care, Health, and Cost," Health Affairs, May/June 2008 27(3):759–69.
2 For details regarding data used and modeling assumptions see J. Mays, D. Waldo, R. Socarras et al., Technical Report: Modeling the Impact of Health Care Payment, Financing, and System Reforms (prepared for The Commonwealth Fund by Actuarial Research Corporation, Jan. 2013).


