Many studies have found that blacks, Hispanics, Native Americans, and Asians receive less adequate and less intensive health care than whites—and that such disparities persist even after taking into account health insurance status, age, sex, income, and education. To further understanding of the causes of these disparities, The Commonwealth Fund supported the February 2004 issue of the Journal of General Internal Medicine. Contributors examined racial or ethnic health disparities in care for depression, patients' views of Medicaid managed care, treatment of prostate cancer, mammography screening rates, Medicare expenditures, and doctor–patient communication, among other topics.
Focus on Asian American Patients
One Fund-supported study in the journal focused on the experiences of Asian mericans—one of the fastest-growing ethnic groups, but one whose health care experiences are less well studied than those of other minority groups.
"Asian Americans' Reports of Their Health Care Experiences," by Quyen Ngo-Metzger, M.D., M.P.H., a former Commonwealth Fund/Harvard University Minority Fellow now at the University of California at Irvine, College of Medicine, and colleagues, examines why, compared with white patients, Asian Americans are less satisfied with their medical care. Specifically, the study examines whether differences in satisfaction levels reported by Asian Americans and whites are due to differences in problems reported in the clinical encounter or to other patient characteristics, such as race/ethnicity, income, or education. The study uses data from the nationally representative Commonwealth Fund 2001 Health Care Quality Survey. The study sample of 3,205 white patients and 521 Asian American patients is of those with a doctor visit in the last two years.
The researchers found that Asian Americans were less likely than white patients to report that they were very satisfied with their care overall (42% vs. 64%), and less likely to have a great deal of trust in their doctor (55% vs. 71%).
After taking into account demographic characteristics, health status, insurance, and health care experiences, Asian Americans were still less likely to report that they were very satisfied with their care. Yet, there were not significant differences between Asian American and white patients in terms of their level of trust in their doctors or their desire to change doctors.
The study also found that—across all racial and ethnic groups—respondents who perceived that their doctors did not understand their background and values, or did not listen to In the Literature everything they had to say, were less likely to be very satisfied with care.
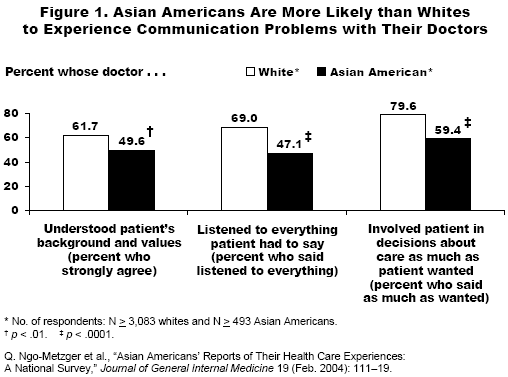
Asian Americans were more likely than white respondents to say that that their doctor did not understand their background and values (61.7% vs. (49.6%) (Figure 1). While nearly four of five (79.6%) of white patients said that their doctors involved them in care decisions as much as they wanted, only three of five (59.4%) Asian Americans reported this. Nearly 70 percent of whites said that their doctor listened to everything they had to say, but less than half (47.1%) of Asian Americans said this.
In addition, Asian Americans were less likely than other groups to report that their doctors counseled them about lifestyle issues (e.g., nutrition, exercise, or smoking) or mental health issues.
Bias and Cultural Competence
Another Fund-supported study, "Racial and Ethnic Differences in Patient Perceptions of Bias and Cultural Competence in Health Care," looked at interpersonal aspects of care, which in studies of health disparities have received less attention than have clinical aspects of care. The 2002 Institute of Medicine report, Unequal Treatment, suggested that health disparities are not explained entirely by differences in services or access, but instead exist in the broader context of social and economic inequality, prejudice, and bias.
Rachel L. Johnson, 2004 M.D./Ph.D. candidate at Johns Hopkins University, Lisa A. Cooper, M.D., M.P.H., a former Picker/Commonwealth Fund Scholar who is now associate professor of medicine at Johns Hopkins University, and colleagues, used the Commonwealth Fund 2001 Health Care Quality Survey to study: 1) whether racial and ethnic differences exist in patients' perceptions of bias related to their primary care provider (PCP) and to the health care system in general and 2) whether these differences are explained by patient demographics, source of care, or patient–provider communication. The study is based on a nationally representative sample of 3,488 white patients, 1,037 black patients, 1,153 Hispanic patients, and 621 Asian patients.
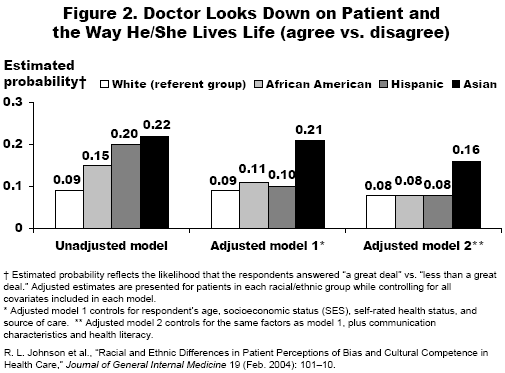
The researchers found that blacks, Hispanics, and Asians were more likely than whites to agree: that they would receive better medical care if they belonged to a different race; and that medical staff judged them unfairly or treated them with disrespect because of their race or how well they spoke English. These differences were somewhat diminished—but not fully explained—by differences between racial groups in demographics, health status, source of care, or patient–provider communication (see Figure 2). The researchers conclude that, overall, racial and ethnic minorities perceive bias and a lack of cultural competence in the health care system as a whole. Cultural competence can be defined broadly as the need for health care professionals to recognize and respond to their own and their patients' cultures.
By contrast, most racial and ethnic differences in patient ratings of bias or cultural competence on the part of individual physicians were explained, almost entirely, by demographic variables, health literacy, medical communication, and source of care.