The United States stands out among industrialized nations for the pronounced health care inequalities between lower- and higher-income adults, this Health Policy study finds. In "Inequities in Access to Medical Care in Five Countries"—which compares the U.S. with Australia, Canada, New Zealand, and the United Kingdom—Commonwealth Fund researchers Cathy Schoen and Michelle M. Doty report wide and significant income disparities in the U.S. regarding cost-related access problems, quality of care, and ratings of physicians. These results hold, the authors say, after controlling for health insurance status, race/ethnicity, immigration status, and other important factors.
By comparison, few significant differences by income were found in the U.K. and Australia. There were some differences in Canada and New Zealand, mostly for services less well covered by the national health care systems in those nations. The study was based on analysis of the 2001 Commonwealth Fund International Health Policy Survey, which included 1,400 adults, ages 18 years or older, in each of the five countries.
The health care systems in the five nations differ in terms of the role of private insurance, extent of patient cost-sharing and out-of-pocket expenses, and benefits covered. The U.S. is unique as the one country that does not provide universal coverage for at least a core set of benefits and for its reliance on a mixed system of voluntary private insurance and public coverage for the elderly and some of the poor. The four other nations in the survey provide universal public coverage, yet they differ in the scope of benefits and cost-sharing as well as the prevalence and role played by supplemental private insurance.
Access to Care
Adults in the U.K. were the least likely to report difficulties accessing health care due to cost or medical bill problems. In the U.K., gaps between income groups were small, and few adults with either high or low income reported cost-related access problems. In contrast, the U.S. gap by income was wide on all cost-related access problems and measures of financial burden. These measures included forgoing medicine or treatment, not seeking treatment when sick, and problems paying medical bills.
Cost Protection
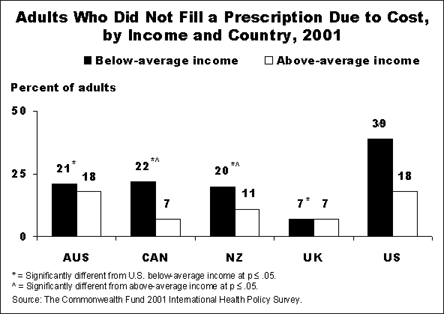
Due to variations in public insurance policies, including the scope of benefits covered by core public programs, the five countries differ substantially in the extent to which residents are exposed to out-of-pocket costs for medical bills. The U.S. stands out for high out-of-pocket expenses, with 42 percent of respondents estimating they paid $500 or more in the past year, compared with only 5 percent of adults in the U.K. Canadians were also relatively well protected, with one-third of adults reporting no out-of-pocket expense in the past year. Adults in Australia and New Zealand were more likely to encounter out-of-pocket costs than those in the U.K. or Canada, yet they had a much lower level of exposure than U.S. adults.
Quality of Care
Ratings of physician care were highest in Australia and New Zealand and lowest in the U.K. and U.S., with Canadian ratings falling between these two groups. Although adults in the U.K. reported overall low levels of physician ratings, it emerged as the one country in which ratings of care were more positive among lower-income adults than among adults with above-average incomes. This was clearly not the case in the U.S., where significant income disparities were identified on all quality and physician ratings measures. These measures included treating patients with dignity and respect, listening carefully to their health concerns, and being accessible to patients by phone or in person. Lower-income adults in the U.S. were much less likely to give their doctors positive ratings.
Having supplemental insurance protected adults from cost-related access problems in Australia, Canada, and New Zealand. However, only in Canada were adults with supplemental coverage more satisfied with their interactions with doctors than those with public coverage only. In the U.K., where rates of supplemental coverage are much lower across income groups, having supplemental coverage made little difference to general access, cost-related barriers, or quality-of-care ratings.
Health System Views
When the authors examined respondents' views of their country's medical system, they discovered that the U.S. had the widest divergence of opinion between individuals with below- and above-average incomes. In the U.S., differential access to health care by income may result in divided opinions about the need or direction of health care reform. Yet the authors note that only a minority of survey respondents in all five countries thought their system of care basically worked well, with only minor changes needed. In the U.K., there was little difference in opinion between persons with above- and below-average incomes—even though 18 percent of Britons surveyed believed that problems with the National Health Service required the system to be completely rebuilt.
The study's findings demonstrate that some health systems are more able than others to minimize financial barriers to access and quality care among low-income adults, the authors say. Furthermore, the results suggest that a health insurance system that fails to provide basic coverage to all residents will result in widespread inequities by income.
Facts and Figures
Extent of national health coverage in the five countries:
- Australia: National coverage, but private insurance allowed to make up for some permitted patient billing by doctors.
- Canada: National coverage, but prescription drugs and dental care not covered.
- New Zealand: National coverage, but dental care covered only for school children. Copayments for many services.


