The medical care that minority children receive often is inferior to the health care services enjoyed by other children. Current research on racial and ethnic disparities documents widespread failings in both access to care and the quality of care for millions of minority children.
But methods to reduce these disparities do exist, particularly when implemented by the federal government, says The Commonwealth Fund's Anne C. Beal, M.D., M.P.H. In her article, Policies to Reduce Racial and Ethnic Disparities in Child Health and Health Care (Health Affairs, Sept./ Oct. 2004), Beal describes an arsenal of weapons available for reducing racial disparities in health care: broadening health care coverage, adopting common quality improvement efforts, improving the training of health care providers, and boosting the ranks of minority clinicians.
Expanding Coverage
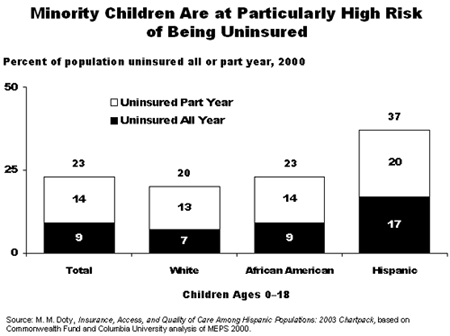
Many minority children lack health insurance, making it more difficult for their parents to access care compared with white families. National surveys show that 37 percent of Hispanic children had a period without health coverage during the last year, compared with 23 percent of African American children and 20 percent of white children (see figure). Despite substantial gains in insurance coverage since the creation of the State Children's Health Insurance Program (SCHIP) in 1997, it is estimated that fewer than half of all eligible children are enrolled in SCHIP.
Currently, states set their own eligibility caps for SCHIP. But more minority children would benefit if states had uniform eligibility requirements, Beal argues, since SCHIP and Medicaid both have large minority enrollments. If all states enrolled all children in families up to 200 percent of the federal poverty level, for example, three-quarters of uninsured children would have coverage. Further analysis could determine the best ways to increase enrollment.
Improving Quality
If quality-of-care interventions were supported through publicly funded health programs such as SCHIP and Medicaid, they would have a strong impact on racial and ethnic disparities in quality, the author writes.
Currently, many health care systems with a minority patient base rely largely on Medicaid for funding and thus have fewer resources to deliver higher-quality care than providers with a wealthier, privately insured patient base. A recent study of Medicaid managed care plans cited by the author found that Medicaid plans underperformed commercial plans on a variety of pediatric clinical measures.
It is important, then, to frame health care disparities as a quality issue, Beal says. If a health care system is allowed to provide poor-quality care to any segment of the pediatric population, she argues, then all children are at risk for receiving inferior medical care.
Unfortunately, current child health care quality measures are not designed to monitor racial disparities. One method to correct this failing, the author says, is to require the collection of data on patients' race and ethnicity and link them to quality indicators. Currently accepted measures of quality (HEDIS, for example) could be altered so that the reports are stratified by race and ethnicity. Identifying race and ethnicity, the author notes, would improve the ability to track minority child health disparities during the process of monitoring the quality of care of all children.
Role of Health Care Providers
The work of individual clinicians and other health care providers can lessen racial disparities in health care, notes Beal. For example, providers who receive training in cross-cultural interaction are better able to communicate and connect with patients from different racial and ethnic backgrounds. And providers well trained in cross-cultural sensitivity can help foster greater patient satisfaction, engagement, and involvement in health care regimens.
Medical schools now include "cultural competency" training as part of their curricula, and this will benefit future generations of physicians. But what about doctors already in practice? Beal argues that one way to improve cultural sensitivity among currently practicing physicians would be to require training in this area as part of the maintenance of board specialty certification and license renewal that doctors in all states must undergo periodically.
Boosting the number of minority providers should be another policy goal, Beal says. Minority providers are more likely to work in low-income, underserved communities, and more likely to care for Medicaid patients and patients of color. But the ranks of minority providers are thin: in 2001, only 11 percent of students accepted to medical schools belonged to racial or ethnic minority groups, even though minorities represent 25 percent of the U.S. population.
In addition, Beal says minority youth need to be better prepared for the rigors of college and medical school. Building upon the federal No Child Left Behind Act—which increases the accountability of schools that perform poorly—the government could designate communities with health care disparities and academically inferior schools as "Health and Education Empowerment Zones." These communities would receive additional federal funding for improved education and expansion of science and health curricula. Linking these two fields could encourage young people from communities most affected by health disparities to become health providers.
Need for Federal Leadership
Although individual federal, state, and private sector programs have been launched to take on disparities in health care, coordination and monitoring of these efforts at the federal level is needed to maximize their effectiveness, Beal says. She suggests creating an advisory council of minority health experts charged with oversight of disparity-reduction programs, coordinating efforts across federal agencies, and obtaining reports on locally based programs to improve minority health care. Such a council, Beal says, could include a special focus on priority populations, such as children, to ensure their unique needs are addressed.
Facts and Figures
- Fewer than half of all children who are eligible for health insurance coverage under SCHIP are thought to be enrolled (Kaiser Commission on Medicaid and the Uninsured, June 2002).
- If all states raised their SCHIP eligibility to enroll all children within 200 percent of the federal poverty level, then 6.6 million uninsured children—75.2 percent of all uninsured children—would be covered (J. D. Reschovsky and P. J. Cunningham, 1998).
- Medicaid managed care plans were found to have lower performance scores than commercial plans on childhood immunizations (54% vs. 69%, respectively) and on the number of well child care visits (31% vs. 53%) (J. W. Thompson et al., 2003).


