In the Literature
Health care coverage leads to dramatic improvement in health trends for previously uninsured older individuals, particularly those with cardiovascular disease or diabetes, according to a Commonwealth Fund-supported study published in the Journal of the American Medical Association.
A team of Harvard Medical School researchers assessed the effect of acquiring Medicare coverage on the health of previously uninsured adults. In the article, "Health of Previously Uninsured Adults After Acquiring Medicare Coverage" (Journal of the American Medical Association, Dec. 26, 2007), J. Michael McWilliams, M.D., and his colleagues present the strongest evidence to date that health improves significantly when people gain health insurance. For example, for every 100 uninsured adults with heart disease or diabetes before age 65, the researchers found that with Medicare coverage they had 10 fewer major cardiac complications, such as heart attack or heart failure, than would be expected by age 72.
Coverage Benefits Chronically Ill Most
The research team assessed data from the Health and Retirement Study for 7,233 participants, all of whom entered the study in 1992 when they were at least age 55. Using comprehensive self-reported health measures to assess overall general health, mobility, agility, pain, depression, and cardiovascular outcomes, the team collected survey data every two years from participants between 1992 and 2004. They also calculated a summary score by adding these components. Of the participants, 5,006 were continuously insured, while 2,227 were either persistently or intermittently uninsured until they qualified for Medicare at age 65.
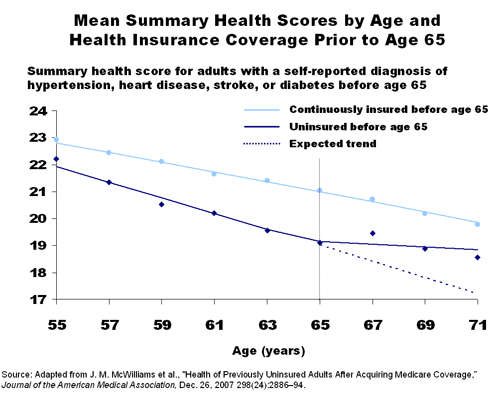
While individuals who had continuous health insurance coverage did not report a significant change in their health trends as they transitioned to Medicare, those who had no or little coverage reported substantial improvements. Uninsured individuals who had heart disease or diabetes reported the most dramatic improvements in health trends after gaining Medicare coverage. Among adults with such conditions, health declined at a much faster rate for the uninsured when compared with insured individuals before age 65. This trend, however, changed at age 65, so that by age 70, predicted health differences between uninsured and insured were cut by half.
"Proper management of blood pressure, glucose, and cholesterol substantially reduces morbidity and mortality for adults with these conditions, and expanded use of effective treatments may produce considerable benefits for under-served populations," the authors write. "Having prescription drug coverage after age 65 years was associated with particularly improved health trends for adults with cardiovascular disease or diabetes, suggesting greater benefits of Medicare coverage for previously uninsured adults now eligible for Medicare prescription drug coverage."
Differences Measure by Measure
Compared with previously insured adults with cardiovascular disease or diabetes, previously uninsured adults with such conditions reported significantly improved trends in their summary health scores, as well as in general health, mobility, agility, and adverse cardiovascular outcomes, but not in depressive symptoms. Previously uninsured adults without these conditions reported differential improvement in depressive symptoms but not in summary health or any other measure.
Conclusions
The new Harvard study builds on earlier research, published by the authors in the New England Journal of Medicine, which suggested that uninsured adults entering Medicare end up costing the health system more in annual medical spending after age 65. (See "Use of Health Services by Previously Uninsured Medicare Beneficiaries," NEJM, July 12, 2007).
The authors earlier found that acquiring Medicare coverage was associated with greater increases in physician visits for previously uninsured adults with these conditions. Thus, improvements in health trends may have been mediated in part through expanded access to ambulatory care and effective medications for primary and secondary prevention of coronary heart disease and congestive heart failure.
"Our findings have important policy implications," the authors note in their JAMA article. "Proposals to extend insurance coverage to uninsured near-elderly adults have been introduced in the U.S. Congress and endorsed by the American College of Physicians. Providing earlier health insurance coverage for uninsured adults, particularly those with cardiovascular disease or diabetes, may have considerable social and economic value for the United States by improving health outcomes."
Facts and Figures
- Among the study sample, 61% reported diagnoses of hypertension, heart disease, stroke, or diabetes before age 65. Of these, 70% were insured and 30% were uninsured.
- Relative to insured near-elderly adults, uninsured near-elderly adults, particularly those with cardiovascular disease or diabetes, experience worse health outcomes before age 65, and use more health services as Medicare beneficiaries after age 65.