In the Literature
Ideally, in a high performance health care system, all the providers caring for a patient work together—sharing medical records, coordinating prescriptions, making test results available. The patient is also well-informed, receiving instructions about next steps and the right people to contact with questions. Most patients in the United States, however, do not receive this kind of care, despite the Institute of Medicine's designation of care coordination as a critical element of patient safety and quality.
In "Beyond Our Walls: Impact of Patient and Provider Coordination Across the Continuum on Outcomes for Surgical Patients" (Health Services Research, Feb. 2007), lead author Dana Beth Weinberg, Ph.D., of Queens College, and researchers, including Jody Hoffer Gittell, Ph.D., of Brandeis University, surveyed knee-replacement surgery patients about the coordination of their discharge care. Patients identified serious communication breakdowns between providers, as well as between providers and patients. Measured six weeks post-surgery, coordination of care problems were associated with adverse health outcomes—greater joint pain, lower functioning, and reduced satisfaction.
What Do Patients Experience?
Most research on the subject of care coordination has focused on a single institution, typically a hospital or an outpatient setting, say the authors. This study examines post-surgical care involving multiple settings and types of care providers. Surgical patients' experiences of post-discharge coordination were examined as they moved between hospitals, rehabilitation facilities, and their homes. A total of 222 unilateral knee replacement patients at Brigham and Women's Hospital in Boston between 2003 and 2004 were surveyed before surgery and at six and 12 weeks post-surgery.
Problems Along the Continuum
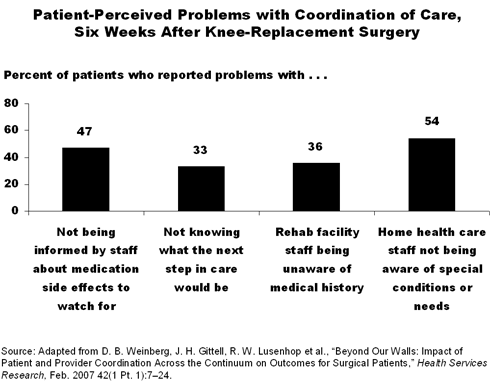
Patients in the study, overall, reported high levels of satisfaction and significant improvements in pain and functioning post-surgery. However, patients also reported numerous coordination-of-care problems, which suggest "difficulties coordinating across settings, within settings, and between patients and providers," say the authors. The average patient reported problems on 42 percent of the indicators related to coordination of discharge. At six weeks post-surgery, 46 percent of patients reported not being told what problems related to surgery to watch for and 47 percent reported not being informed about the side effects of medications. A smaller percentage (20%) reported that staff did not explain the purpose of medications effectively.
For patients who were discharged to rehabilitation facilities, common coordination problems included staff not being aware of the results of patients' surgeries (25%), patients' histories (36%), or any special conditions or needs (43%). Overall, patients reported problems on 44 percent of the indicators related to coordination at such facilities. Fewer problems were reported from patients at home health care agencies; the average patient reported problems with 35 percent of the indicators. Handoffs from the sending organizations—whether a hospital or rehab facility—remained problematic, with 27 percent of patients reporting staff were not aware of the results of surgery. The quality of communication between patients and providers was reportedly better at the home care agencies; only 16 percent of patients at such sites reported having problems finding someone to talk with about concerns, compared with 39 percent of patients at rehab facilities.
Follow-up with surgeons proved the least difficult from the patients' viewpoint, with the average patient reporting problems on 17 percent of the indicators. Twenty-six percent of respondents reported that surgeons did not know about their progress in physical therapy, and 17 percent said that the surgeon did not explain what to do if problems or symptoms continued, got worse, or came back. When asked about general coordination issues, the average respondent reported problems with 30 percent of the indicators. Almost one-fifth (18%) of patients did not get the information they wanted from providers; nearly one-fourth (22%) did not know to whom to go with questions, and one-third (33%) did not know what the next steps in care should be.
Conclusions
Coordination across settings affects clinical outcomes and satisfaction with care. Patients who reported coordination problems were more likely to have greater joint pain, lower functioning, and decreased satisfaction six weeks after knee replacement surgery. At 12 weeks after surgery, coordination problems were associated with greater joint pain, but not with functional status. "These findings are striking," say the authors, "because they were obtained in connection with a highly routine, elective procedure with a high rate of patient satisfaction and success in improving pain and functioning. Even within this successful scenario, improvements in coordination made significant improvements in clinical outcomes."
The study has important implications for health care providers and policymakers, the researchers say. Efforts must be made to improve coordination across the continuum of care, ensuring that health status is not undermined when a patient transfers to a new setting and another set of providers. Success will hinge upon changes in reward structure, performance measures, and in the hiring and training of providers, the researchers conclude.