In the Literature
Many Americans experience instability in their health insurance coverage. After being uninsured for a time, they may gain coverage for several months or several years, only to become uninsured again when they lose their job or family circumstances change. The problem is particularly acute for minorities and people with low incomes. Children covered by public programs—Medicaid and the State Children's Health Insurance Program—have a built-in source of instability: they must have their eligibility requirements verified periodically, which can create breaks in coverage.
In How Stable Is Medicaid Coverage for Children? (Health Affairs, March/April 2007) Gerry Lynn Fairbrother, Ph.D., of Cincinnati Children's Hospital, and colleagues examine enrollment patterns for children covered by Medicaid. The researchers find that while the program provides a "long-term continuous source of coverage for millions of children," it also creates "a revolving door for others." Many children are covered for reasonably long periods, but many others experience short gaps—from two to four months—in coverage. The authors note that "[e]ven brief gaps are likely to cause disruption in care management and possibly in heath care itself."
Continuity and Gaps
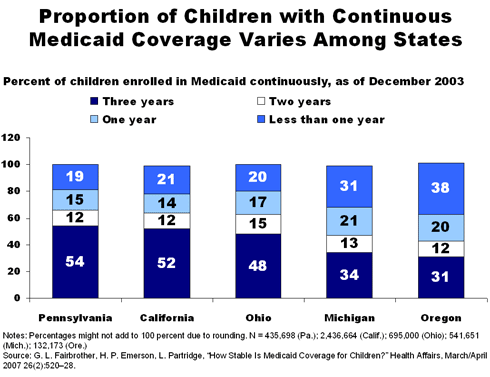
The researchers analyzed Medicaid enrollment data for children in California, Michigan, Ohio, Oregon, and Pennsylvania from January 2001 to December 2003. They found considerable variation in coverage stability, proportion of children with gaps, and the number of gaps. Look-ing across states, 43 to 68 percent of children were covered for two or more years, but 16 to 41 percent had gaps in coverage.
Children were more stably covered in some states than others. Over half the children in Pennsylvania and California had been in Medicaid for three or more years, and nearly two-thirds had been in the program for two or more years. In contrast, only a third of the children in Michigan and Oregon had been enrolled three or more years. Even in these states, however, 43 percent and 47 percent, re-spectively, had continuously enrolled for at least two years. In all five states, at least 60 percent of the children had been in Medicaid for at least one year.
Most gaps were short: half of the Michigan children who lost coverage were reenrolled within two months. In California, Ohio, and Pennsylvania, half were back on the program in three months. In all states, more than 70 percent of the children with breaks in coverage had only one gap, while 8 percent to 24 percent had two gaps. Michigan and Oregon had higher proportions of children with a gap, as well as children with the most gaps.
Implications: Revisit Policies to Reduce Gaps for Eligible Children
The short duration of coverage gaps imply "that states should be encouraged to adopt eligibility policies and administrative procedures designed to keep children enrolled," say the authors. While periodically checking eligibility requirements is necessary to ensure the appropriate use of public funds, frequent checks and cumbersome application and recertification procedures can create barriers to coverage. Despite efforts to simplify the process, beneficiaries are sometime confused about coverage renewal, which can lead to breaks in coverage.
The finding that many children remained covered for two or more years means that states can effectively monitor and improve quality, the authors write. Efforts to manage disease for chronic conditions, improve immunization coverage, or increase the numbers of well-child visits have time to show results and states can be assured they are reaching a majority of their Medicaid-enrolled children.
Unanswered Questions
Studies have found that children with gaps in health care coverage commonly go without medical care, including preventive check-ups, and do not fill prescriptions. Gaps in coverage can also create administrative inefficiencies, as program staff process the same enrollees over and over. High costs and poor outcomes, meanwhile, result from delayed care.
While this study provides new information, it also raises questions, the authors say. We do not know why children lose coverage, or more important, the effect these gaps in coverage may have on children's health and health care. However, the large numbers of children continuously covered by Medicaid suggests that states can demand more of the health system to improve quality of care. Federal and state policies, the authors say, "should be revisited to try to minimize the number of coverage gaps for children."
- A study found that approximately 85 million Americans—or one of three—were uninsured at some point between 1996 and 1999.
- During this same period, more than 40 per-cent of children experienced a gap in coverage; almost half of these children were repeatedly or continuously uninsured.
- Research has shown that more than half of children who lose Medicaid coverage are still eligible.
- California, Michigan, Ohio, Oregon, and Pennsylvania account for nearly 30 percent of the Medicaid population.