An abstract is available at:
http://www.hcmrjournal.com/pt/re/hcmr/abstract.00004010-200810000-00009.htm
Synopsis
Clinical interventions designed to improve care for at-risk patients can yield returns. A recent study found that Medicaid managed care organizations were able to recoup the costs—and even earn a return on investment—for such interventions. Findings suggest a business case can be made for investing in selected quality-enhancing interventions that target high-risk, high-cost beneficiaries.
The Issue
Evidence suggests that investing in interventions to improve the quality of health care has the potential to reap substantial economic and social benefits, through reductions in utilization and associated costs. Yet in the absence of a strong business case for making such investments, widespread adoption is uncertain. Health care entities would be more likely to invest in quality-enhancing programs if the expected return were positive.
Key Findings
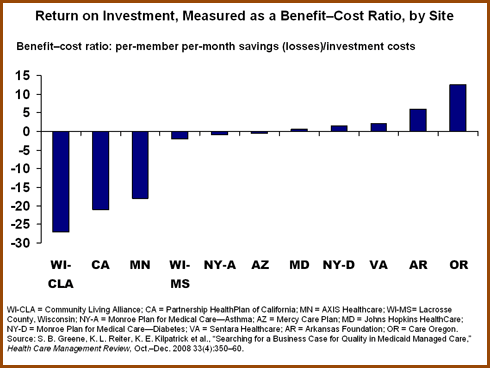
- Four of the 11 quality-enhancing interventions studied earned a positive financial return for their sponsoring organizations, and did so within the first year of implementation. A complex case-management program to treat adults with multiple illnesses achieved the biggest return (12.21:1).
- Additional interventions that saw a positive financial return included a program to treat children with a history of emergency room use and hospitalization for asthma (6.35:1), mothers with high-risk pregnancies (1.26:1), and diabetic adults (1.16:1).
- Providers that earned a positive return spent more on case managers, nurse educators, and other clinical staff; two had higher overall investment costs relative to those that failed to recoup their investment.
- Sites with a negative return on investment reported increases in hospital inpatient visits and associated per-member per-month payments. Conversely, those with a positive financial return experienced significant per-member per-month payment savings during the second year of implementation.
Addressing the Problem
 Investing in quality-enhancing interventions that focus on high-risk, high-cost patients have the greatest potential to earn a positive financial return. How the money is spent—not necessarily how much—may be the key determinant for recouping costs. In addition, the authors recommend that providers develop tracking systems for claims and financial data to help determine which quality-enhancing interventions offer a positive financial return.
Investing in quality-enhancing interventions that focus on high-risk, high-cost patients have the greatest potential to earn a positive financial return. How the money is spent—not necessarily how much—may be the key determinant for recouping costs. In addition, the authors recommend that providers develop tracking systems for claims and financial data to help determine which quality-enhancing interventions offer a positive financial return.
About the Study
The demonstration project included 10 geographically and structurally diverse Medicaid managed care organizations representing a broad range of patient populations. The providers designed and implemented quality-enhancing interventions to address a variety of chronic illnesses common in Medicaid populations, including asthma, diabetes, congestive heart failure, chronic obstructive pulmonary disease, substance abuse, high-risk pregnancy, and pressure ulcers and urinary tract infections among people with mobility-restraining disabilities. Costs to implement the intervention and per-member per-month payments were combined to calculate return on investment.
The Bottom Line
Quality improvement interventions aimed at high-risk, high-cost patient populations may have the greatest potential, at least in the short term, to realize a positive financial return.


