Synopsis
A study of more than 10,000 primary care physicians in 11 countries finds the United States lags far behind in terms of access to care, the use of financial incentives to improve the quality of care, and the use of health information technology. In other countries, national policies have sped the adoption of such innovations.
The Issue
Research shows that strong primary care is associated with good health outcomes and lower costs. It also can help meet the challenges presented by aging populations and the rising incidence of chronic disease. Across the globe, countries are working to redesign their primary care systems by investing in information technology, round-the-clock access, teamwork, integration, and quality improvement. They also are working to reform delivery systems and payment policies. This study surveyed primary care physicians in 11 countries to find out what is happening on the front lines of health care. 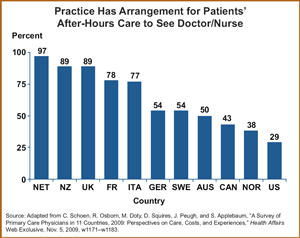
Key Findings
- More than half (58%) of U.S. physicians—by far the most of any country surveyed—said their patients often have difficulty paying for medications and care. Half of U.S. doctors spend substantial time dealing with the restrictions insurance companies place on patients’ care.
- Only 29 percent of U.S. physicians said their practice had arrangements for getting patients after-hours care—so they could avoid visiting a hospital emergency room. Nearly all Dutch, New Zealand, and U.K. doctors said their practices had arrangements for after-hours care.
- Only 46 percent of U.S. doctors use electronic medical records, compared with over 90 percent of doctors in Australia, Italy, the Netherlands, New Zealand, Norway, Sweden, and the United Kingdom.
- Twenty-eight percent of U.S. physicians reported their patients often face long waits to see a specialist, one of the lowest rates in the survey. Three-quarters of Canadian and Italian physicians reported long waits.
- While all the countries surveyed use financial incentives to improve the quality of care, primary care physicians in the U.S. are among the least likely to be offered such rewards; only one-third reported receiving financial incentives. Rates were also low in Sweden (10%) and Norway (35%), compared with large majorities of doctors in the U.K. (89%), the Netherlands (81%), New Zealand (80%), Italy (70%), and Australia (65%).
- Patients with chronic illness require substantial time with physicians, education about their illness, and coaching about treatment, diet, and medication regimens. Care teams composed of clinicians and nurses have been shown to be effective in providing care to people with chronic conditions and in improving outcomes. The use of such teams is widespread in Sweden (98%), the U.K. (98%), the Netherlands (91%), Australia (88%), New Zealand (88%), Germany (73%), and Norway (73%). It is less prevalent in the U.S. (59%) and Canada (52%), with France (11%) standing out on the low end.
Addressing the Problem
The advanced health information technology and extensive use of quality incentives and care teams reported by Australian, Dutch, and New Zealand doctors reflect national payment and information system policies focused on primary care. Lacking such policies, the U.S. lags far behind its peers in these areas—even as it spends far more on health care overall. In addition, insurance coverage restrictions make it difficult for many U.S. physicians to provide their patients with timely access to care. 
About the Study
The authors surveyed more than 10,000 primary care physicians in Australia, Canada, France, Germany, Italy, the Netherlands, New Zealand, Norway, Sweden, the United Kingdom, and the United States. Data were collected by mail, by telephone, and over the Internet between February and July 2009.
The Bottom Line
Despite spending more on health care than other countries, an international survey finds the United States lags behind on important measures of access, quality, and use of health information technology. There are opportunities to learn as other countries move ahead to enhance the primary care foundations of their health care systems.


