Synopsis
An 11-country survey focusing on health care access, cost, and insurance coverage found that adults in the United States are by far the most likely to go without care because of costs, have trouble paying medical bills, encounter high medical bills even when insured, and have disputes with insurers or payments denied.
The Issue
The health insurance systems of the 11 countries included in the latest Commonwealth Fund International Health Policy Survey vary widely. They range from wholly public systems to hybrid systems of public and private insurance, with varying levels of cost-sharing. In analyzing the survey findings, the researchers examined how the design of insurance coverage can affect access to care, financial protection against high costs and medical debt, and insurance complexity.
Key Findings
-
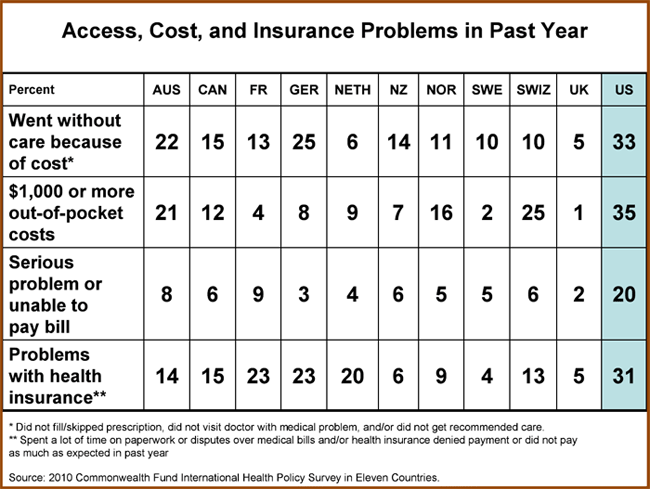
One-third (33%) of U.S. adults went without recommended care, did not see a doctor when sick, or failed to fill prescriptions because of costs, compared with as few as 5 percent of adults in the United Kingdom and 6 percent in the Netherlands.
-
One-fifth (20%) of U.S. adults had major problems paying medical bills, compared with 9 percent or less in all other countries.
-
Thirty-one percent of U.S. adults reported spending a lot of time dealing with insurance paperwork, disputes, having a claim denied by their insurer, or receiving less payment than expected. Only 13 percent of adults in Switzerland, 20 percent in the Netherlands, and 23 percent in Germany—all countries with competitive insurance markets that allow consumers a choice of health plan—reported these concerns.
-
The study found persistent and wide disparities by income within the U.S.—even for those with insurance coverage. Nearly half (46%) of working-age U.S. adults with below-average incomes who were insured all year went without needed care, double the rate reported by above-average-income U.S. adults with insurance.
-
The U.S. lags behind many countries in access to primary care when sick. Only 57 percent of adults in the U.S. saw their doctor the same or next day when they were sick, compared with 70 percent of U.K. adults, 72 percent of Dutch adults, 78 percent of New Zealand adults, and 93 percent of Swiss adults.
-
U.S. , German, and Swiss adults reported the most rapid access to specialists. Eighty percent of U.S. adults, 83 percent of German adults, and 82 percent of Swiss adults waited less than four weeks for a specialist appointment. U.K. (72%) and Dutch (70%) adults also reported prompt specialist access.
Addressing the Problem
The authors conclude that more negative access and cost experiences in the United States, plus wide disparities by income, underscore the importance of the Affordable Care Act's emphasis on insurance expansion, benefit standards, and limits on costs for those with lower incomes. They note that the U.S. has the opportunity to learn from insurance innovations in other countries, including value-based benefit design.
About the Study
The authors based their analysis on a survey of more than 19,000 adults, ages 18 and older, in Australia, Canada, France, Germany, the Netherlands, New Zealand, Norway, Sweden, Switzerland, the United Kingdom, and the United States. Interviews were conducted by telephone between March and June 2010.
The Bottom Line
Compared with the residents of 10 other industrialized countries, U.S. adults are the most likely to report health care problems related to access, cost, and insurance complexity. Comprehensive health reform could lead to improvements in many of these areas.


