Synopsis
A Massachusetts study found many of the criteria available to patients when selecting a physician—including years of experience, paid malpractice claims, and medical school rankings—are not associated with higher quality care.
The Issue
When selecting a physician, consumers rarely have access to measures of clinical quality. Instead, they are encouraged to consider education, board certification, and malpractice history, with the tacit understanding that these characteristics are determinants of a physician's quality. However, the value of these characteristics as predictors of quality has not been established. In this Commonwealth Fund–supported study, researchers used data from a large sample of physicians and patients to examine the relationship between physician characteristics and a range of performance measures.
Key Findings
-
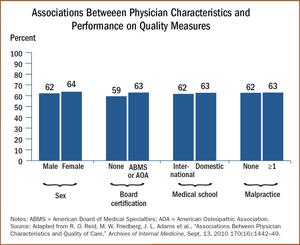 Three of the characteristics studied were associated with marginal differences in performance quality: female physicians scored 1.6 percentage points higher than male physicians; board-certified physicians scored 3.3 points higher than physicians without board certification; and U.S.-trained physicians scored 1 point higher than physicians trained abroad.
Three of the characteristics studied were associated with marginal differences in performance quality: female physicians scored 1.6 percentage points higher than male physicians; board-certified physicians scored 3.3 points higher than physicians without board certification; and U.S.-trained physicians scored 1 point higher than physicians trained abroad. - There were no statistically significant associations between performance and malpractice claims, disciplinary actions, years of practice, medical school ranking, or type of medical degree (i.e., allopathic vs. osteopathic).
- The difference in overall performance between the average physician with the best combination of characteristics (female, board-certified, domestically trained) and the average physician with the worst combination (male, noncertified, internationally trained) is only 5.9 percent.
- Among the middle 90 percent of physicians studied who had the best combination of characteristics, there was a wide range of performance scores—from 49 percent to 75 percent—very similar to the range for all physicians. This suggests that patients are unlikely to receive higher-quality care by switching to a physician who has these characteristics.
Addressing the Problem
 The results of this study show the criteria currently used by consumers in choosing a physician are poor proxies for clinical quality and thus not well suited for use by patients. "Public reporting of individual physician quality data may provide the consumer with more valuable guidance when seeking providers of high-quality health care," the authors conclude.
The results of this study show the criteria currently used by consumers in choosing a physician are poor proxies for clinical quality and thus not well suited for use by patients. "Public reporting of individual physician quality data may provide the consumer with more valuable guidance when seeking providers of high-quality health care," the authors conclude.
About the Study
The authors created performance scores for 10,408 Massachusetts physicians by analyzing claims data from 1.13 million patients enrolled in one of four Massachusetts commercial health plans between 2004 and 2005. Together these plans constituted 85 percent of the commercial market in the state. The authors correlated these scores with publicly available data on individual physician characteristics obtained from the Massachusetts Board of Registration in Medicine, including physician sex, medical school graduation date, board certification status, and payment on malpractice claims.
The Bottom Line
Individual physician characteristics are poor proxies for performance on clinical quality measures and should not be used by consumers when seeking high-quality health care providers. Public reporting of individual physician quality data would provide patients with more valuable guidance.


