Synopsis
In this study, researchers compared the effect that having a choice of health plans has on California Medicaid beneficiaries enrolled in managed care. Beneficiaries without a choice of plan enrolled more quickly, while those with a choice were more likely to delay enrollment in a plan. The authors also found that beneficiaries with a plan choice were admitted to the hospital at a higher rate for conditions that could have been treated earlier in an ambulatory care setting.
The Issue
Choice and competition are seen by many as essential to improving the quality and efficiency of the health care system. Indeed, in the United States, many consumers are able to choose among different health plans, medical groups, and providers. However, some health care analysts posit that the potential benefits of competition and choice are not being realized in practice. Researchers in this Commonwealth Fund–supported study compared two groups of Medicaid beneficiaries in California—one group with a choice of health plans and the ability to switch among plans, and another group with no choice of plans. Beneficiaries with a choice of plans had up to 45 days after gaining Medicaid eligibility to choose a plan.
Key Findings
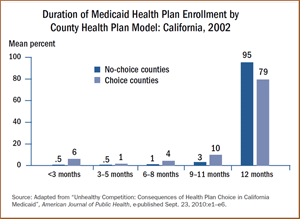
- A higher proportion of beneficiaries who had no choice of plans were continuously enrolled in a health plan for 12 months (95%) compared with beneficiaries who had a choice (79%).
- More than 95 percent of new Medicaid beneficiaries in the no-choice group were enrolled in a health plan during their first month of eligibility. Fewer than 1 percent of those with a choice were enrolled in a plan during the first month, and only half were enrolled in a plan three months after eligibility.
- Annual adjusted hospital admission rates for ambulatory care–sensitive conditions were significantly higher for beneficiaries with a choice of plans (6.58 admissions per 1,000 beneficiaries) than for those with no choice (6.27 admissions per 1,000 beneficiaries).
- Beneficiaries with a choice of plans were able to switch health plans at any time without penalty. However, the rate of plan-switching was low (2.5%), signifying that beneficiaries were satisfied with their plans, unaware they were able to switch plans, or unwilling to switch plans, the authors said.
Addressing the Problem

The findings of this study suggest that policymakers must keep in mind that providing choice in health care may produce unintended, and potentially harmful, consequences. However, interventions can help mitigate these effects, the authors say. For example, state Medicaid programs could conduct outreach to minimize delays in health plan enrollment. Another promising approach is to automatically assign beneficiaries who have not enrolled to a health plan after a fixed period.
About the Study
The authors used data from the 2002 California Medicaid Eligibility File and also accessed inpatient hospital discharge data from the same year, provided by the California Office of Statewide Health Planning and Development. They compared 2.1 million Medicaid beneficiaries who were continuously enrolled in Medicaid during the year: 1. 9 million who resided in 13 counties that offered a choice of health plans and 200,000 who resided in eight counties with a single plan.
The Bottom Line
Giving beneficiaries a choice of health plan in California Medicaid was associated with delays in health plan enrollment and poorer health outcomes. Interventions to mitigate such negative impacts, such as outreach and default enrollment options, should be considered in systems where choice is offered.


