Synopsis
As part of their accountable care organization (ACO) contracts with physician practices, payers offer providers incentives to keep down costs and improve the quality of care that patients receive. A Harvard study found that these incentives can have positive spillover effects for patients not specifically targeted by the incentives—in this case, significantly lower spending on outpatient care. The findings suggest that providers’ responses to the ACO initiative led to broad changes in patient care.
The Issue
A growing number of provider organizations are taking on financial risk for the cost and quality of care they provide to designated patient groups under ACO contracts with public or private payers. But since most provider organizations contract with multiple payers, the incentives to lower spending and improve quality under an ACO contract apply only to a subset of patients in any given organization. Commonwealth Fund–supported researchers sought to examine whether payment incentives implemented under a commercial ACO had spillover effects on the costs and quality of care for patients not covered by the contract. The Harvard researchers focused on Blue Cross Blue Shield of Massachusetts’ Alternative Quality Contract, an ACO initiative implemented in 2009 that has been associated with reduced spending and improved quality for commercial plan enrollees.
Key Findings
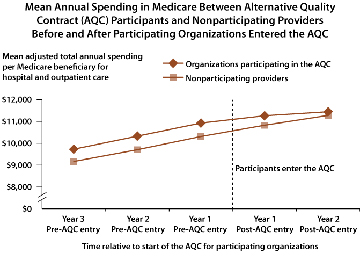
- Prior to participation in the Alternative Quality Contract, quarterly spending per Medicare beneficiary in physician practices was $150 higher than spending in practices not signed on to the contract. By the second year of the contract, this difference in spending was reduced to only $51.
- Savings came largely from reduced spending on outpatient care—including significant changes in spending on office visits, emergency department visits, minor procedures, laboratory tests, and imaging. Savings were greatest among Medicare beneficiaries with five or more medical conditions.
- Rates of cholesterol testing for beneficiaries with diabetes in participating practices improved by 3.1 percentage points, and rates for those with cardiovascular disease improved by 2.5 percentage points.
- Performance on other quality measures did not change substantially.
Addressing the Problem
The study suggests that the ACO payment model has the potential to foster systematic changes in care delivery. Evaluations of ACO programs should consider spillover effects to other patient populations to assess ACOs’ full clinical and economic benefits.
About the Study
The Harvard research team used Medicare enrollment and claims files to compare spending levels and care quality among elderly fee-for-service Medicare beneficiaries served by 11 provider organizations participating in the Alternative Quality Contract in 2009 or 2010 with spending and quality among beneficiaries served by nonparticipating providers. Specifically, the team examined total quarterly medical spending per beneficiary, spending by setting and service type, five process-of-care measures, potentially avoidable hospitalizations, and 30-day hospital readmission rates.
The Bottom Line
The Alternative Quality Contract, which has led to reduced spending and improved quality among targeted commercially insured patients, is also associated with significant reductions in spending for Medicare beneficiaries treated at participating practices, though improvements in quality of care are not consistent. The study’s findings suggest that the new payment incentives can lead to broad changes at participating organizations, bringing benefits to patients not specifically targeted by the contract.


