For newer primary care ventures, customized electronic health record systems are one of the keys to improving population health and coordinating care provided by a wide array of team members.
In addition to creating new staffing models and office layouts for their primary care practices, companies like Iora Health and ChenMed have been investing heavily in customized electronic health record (EHR) systems and other forms of information technology to support their care models. Both companies see EHRs not as a tool for billing and documentation but rather as a means of tracking and communicating with their patients, streamlining the work of team members, and identifying opportunities to intervene across wide populations of patients.
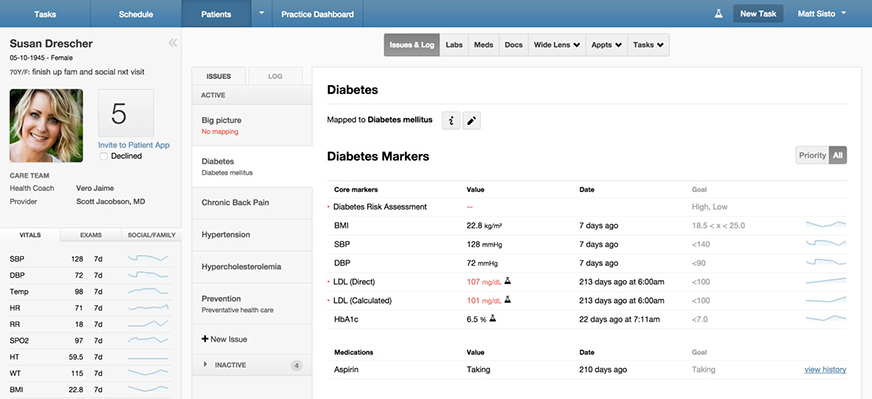
Iora Health’s electronic health record generates to-do lists for each patient and includes a picture of the patient on every page. Source: Iora Health.
For such companies, technology is also a way to wield a competitive advantage in the marketplace, one made possible by capitation agreements that provide per-member or lump-sum fees to care for designated patient panels. This financing model gives companies greater capital to invest in resources they believe are likely to benefit patients. (For Iora Health, venture capital funding has also helped.)
Below are some of the common features of the bespoke EHR systems used by Iora Health and ChenMed, neither of which has relied on federal incentives offered under the Health Information Technology for Economic and Clinical Health (HITECH) Act to adopt and use EHRs.
Focusing on communication, not documentation
Because both groups rely heavily on capitated payments, clinicians are not required to document each discrete health care service they provide. Instead the EHRs are designed as tools for communication—with providers documenting enough to clarify diagnoses and treatment plans but not so much that important information gets lost in the sea of words. “We tell our docs: ‘Write six lines. I’d rather you have conversations with patients and other providers,’” says Christopher Chen, M.D., ChenMed’s CEO.
Customizing interfaces
Like social media sites that let users control the look and feel of their personal pages, ChenMed’s EHR lets providers customize electronic records, emphasizing whatever clinical information is most relevant to patients’ medical problems, or changing where information appears on the page. Performance data for measures such as hemoglobin A1c and blood pressure also are included in patients’ records, so that clinicians can keep track of patients’ outcomes while they are working.
Supporting panel management
ChenMed and Iora Health’s leaders say it was necessary to build their own EHRs in part because commercially available products didn’t support their population health needs, including being able to segment patients, identify their level of risk, and track gaps in care.
For example, both systems organize data according to patients’ diagnoses and needs rather just as a series of encounters. This enables clinicians to see how all of their diabetes patients are faring, for example, and to identify those whose disease is not under control. Both also proactively generate to-do lists for each patient—including steps like ordering follow-up tests or connecting patients to social workers that otherwise may get lost in clinicians’ notes.
ChenMed’s system allows clinicians to visualize their patient panel on a wheel: the closer patients are to the center, the healthier they are; the farther out, the worse. “You can hover over outliers and find out who that is—then open up their clinical data, claims data and analyze it,” says Chen. Iora’s EHR system uses patient data—including management of chronic conditions, lab test results, and social factors, among other information—to generate a “worry score” (1 to 4) for each patient. Clinicians continually provide input to tweak the algorithm.
Using claims data to promote continuity of care
Because of partnerships with payers that put them at risk for patients’ total health care costs, ChenMed (and Iora Health, in some cases) are able to access all of patients’ medical claims data. This allows clinicians to see exactly what procedures occurred during hospitalizations or under past providers, and track prescribing records from outside their organizations. “That reconciliation process is really important,” says Chen. It can also reduce utilization: “If someone said ‘I had a colonoscopy three years ago,’ you can access prior claims records and say ‘Oh yeah, it was actually two years ago, here’s the doctor, we’re going to get the records, don’t worry about it,’” says Andrew Schutzbank, M.D., vice president for clinical development at Iora Health.
Providing accessibility to patients
To avoid having computers create a barrier between patients and providers, with physicians gazing at screens instead of patients, patients’ records at Iora Health are projected onto the wall of exam rooms so they see exactly what their providers see. Health coaches, physicians, and other clinicians serve as one another’s scribes, freeing them from needing to document during the visit. “The rough rule is whoever is talking isn’t typing,” says Schutzbank. The care team also uses video chats, texting, and other tools to communicate with patients.


